39 y/o male presents with acute kidney injury, creatinine 3.5 mg/dl. Bland urinalysis, serologic studies negative. Immunofluorescence study of the renal biopsy was negative for all stains. EM showed no deposits and was otherwise unremarkable.
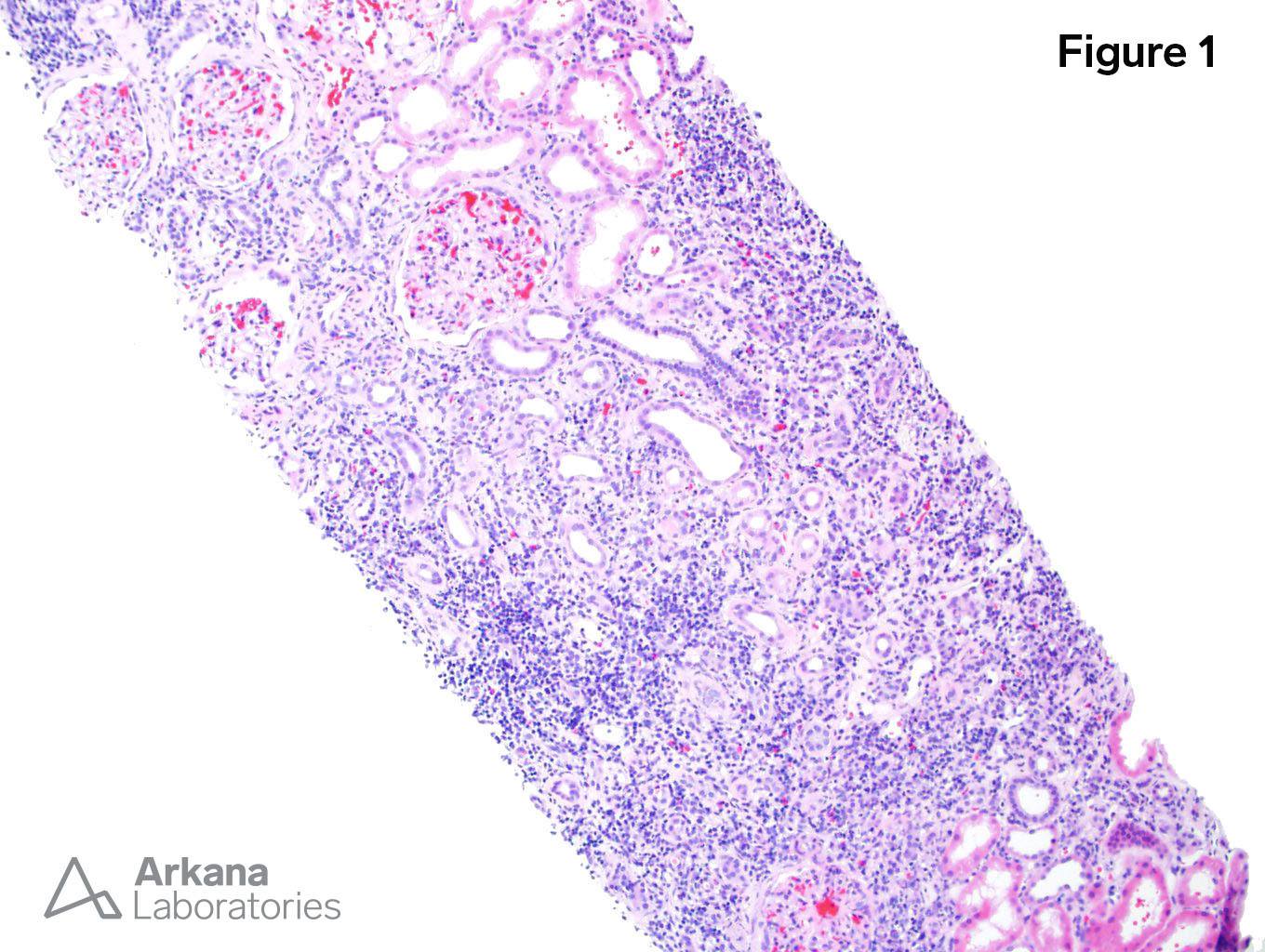
1. Tubulointerstitial nephritis (H&E x100).
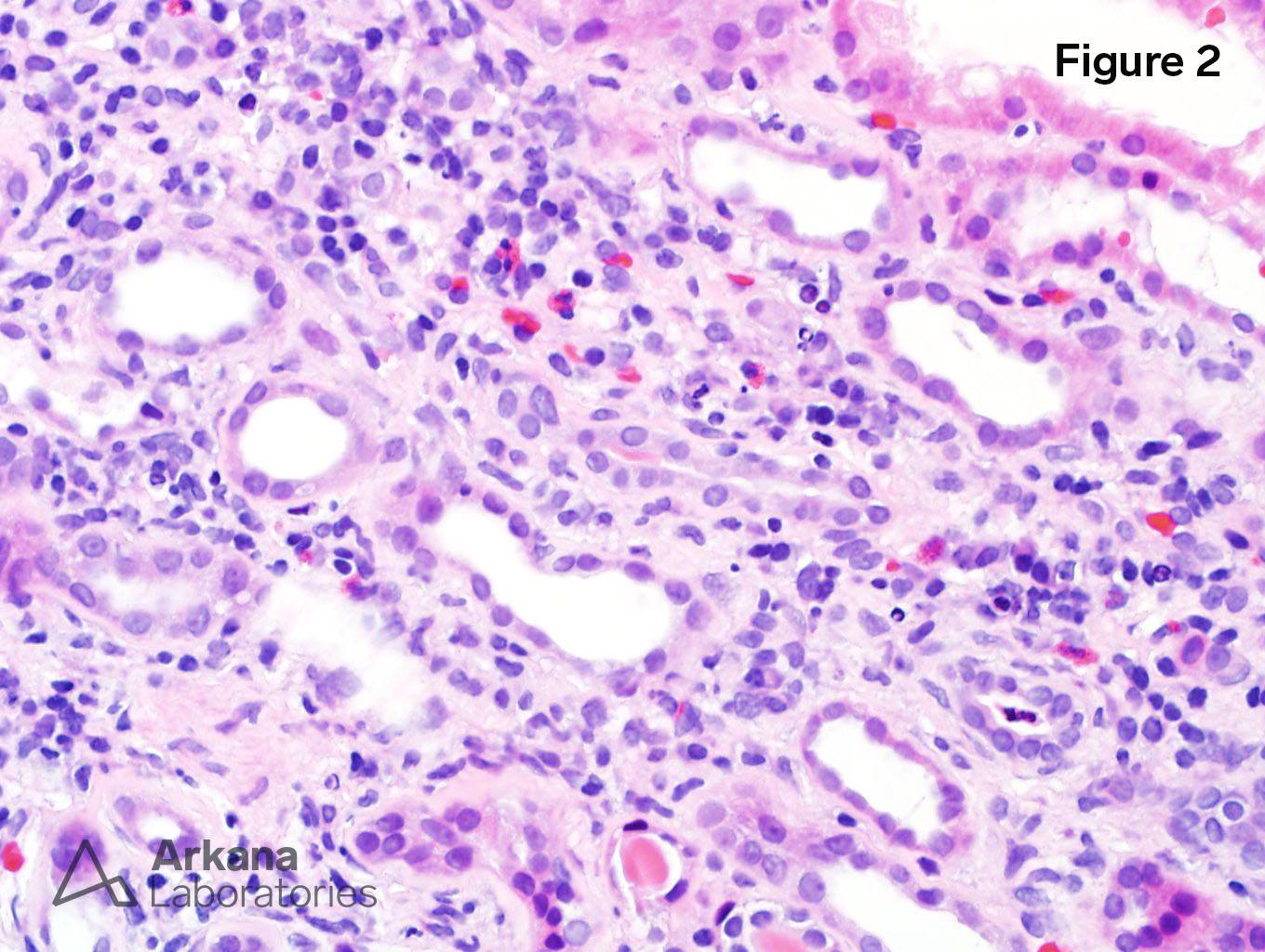
2. Lymphocytes, plasma cells, neutrophils and eosinophils (H&E x400).
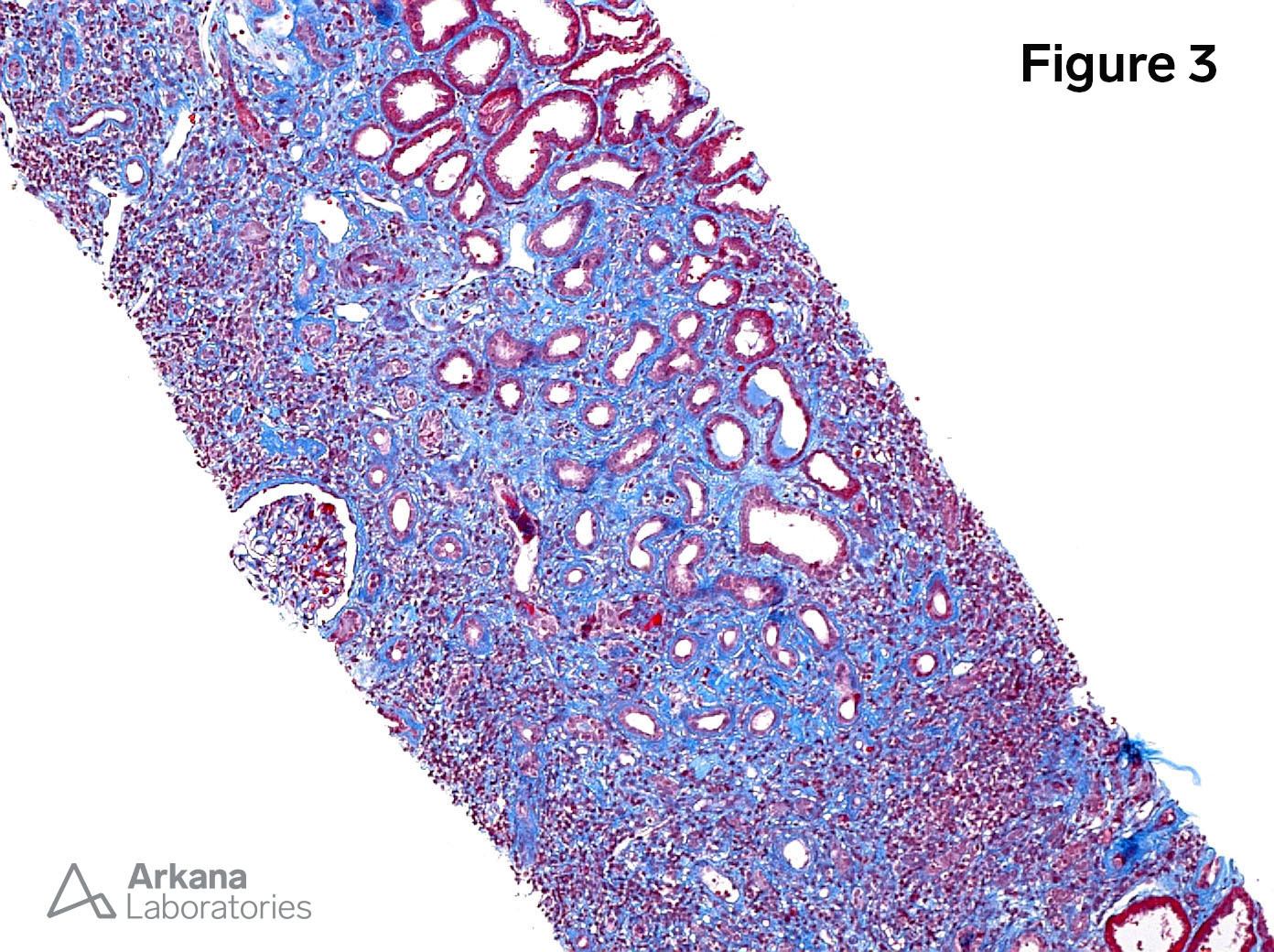
3. Interstitial inflammation and fibrosis (Trichrome x100)
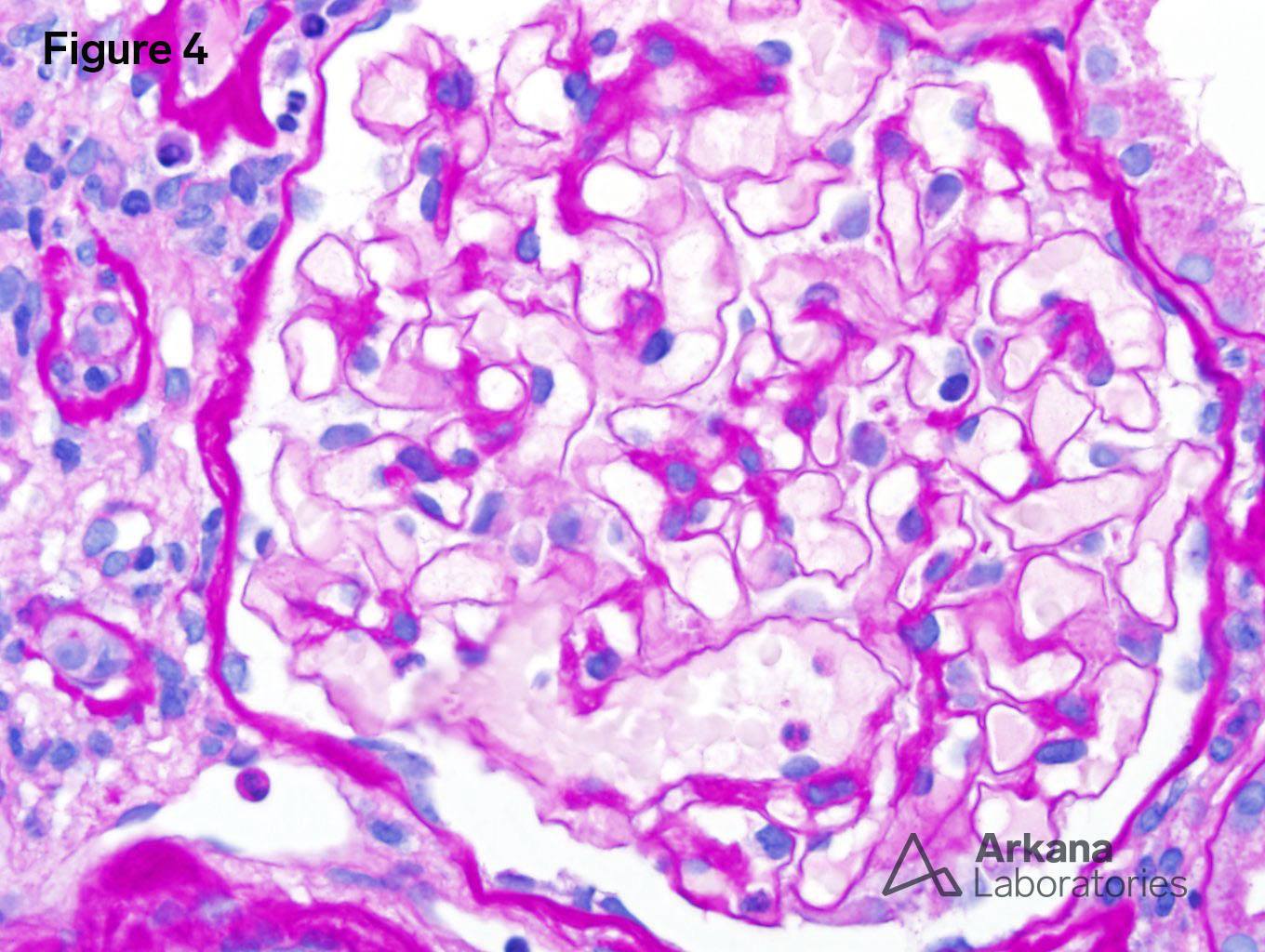
4. Intact glomerulus (PAS x400).
Diagnosis: Chronic Active Tubulointerstitial Nephritis
Comment: Most likely drug-induced but other causes include Sjogren’s syndrome, tubulointerstitial nephritis with uveitis (TINU), Behcet’s syndrome, sarcoid among others.
Further discussion with the clinician after giving the above pathologic diagnosis: “Oh, that fits well. This patient has ulcerative colitis and has been on mesalamine for three years. No one has checked creatinine till two days ago. I brought him in and did the biopsy yesterday.”
“Chronic active” is sometimes miscalled “acute and chronic”. But that is an oxymoron since both refer to the time course. So they cannot be both ‘short’ (acute) and ‘long’ (chronic) at the same time. So, in this case, ‘chronic’ means that this condition has been going on for a while. ‘Active’ means that the causative process is continuing. The chronic part is evidenced by interstitial fibrosis and the active part by the vigorous inflammation.
Reference:
1. Ambruzs JM, Walker PD, Larsen CP: The histopathologic spectrum of kidney biopsies in patients with inflammatory bowel disease. Clin J Am Soc Nephrol 2014, 9:265-70. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3913236/
Quick note: This post is to be used for informational purposes only and does not constitute medical or health advice. Each person should consult their own doctor with respect to matters referenced. Arkana Laboratories assumes no liability for actions taken in reliance upon the information contained herein.