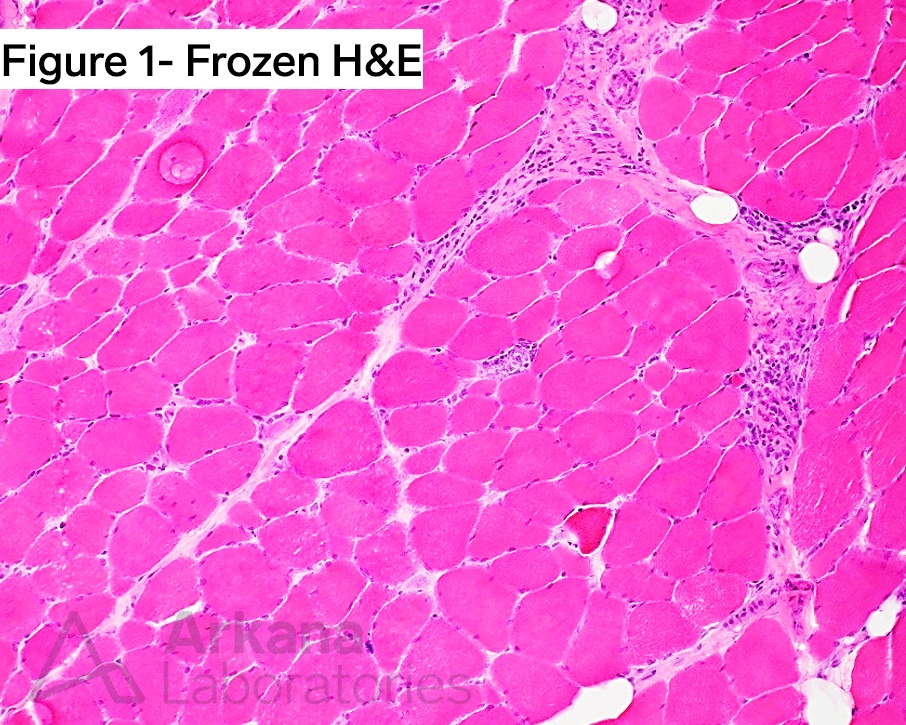
The patient is an elderly female who presents with chief complaint of progressive symmetric proximal muscle weakness over the past one to two months. She also complains of dysphagia, as well as neck and low back pain. The patient’s medication list includes a statin. No prior steroid treatment is reported. Physical exam shows 3/5 strength of the upper and lower extremities. No skin rash is seen. Laboratory work-up reveals elevated CPK ~2000, and routine myositis panel is negative, including anti-SRP with add-on anti-HMGCR serology also negative. Additional myositis serology was ordered, and showed a high positive for anti-U1-RNP. Muscle biopsy of the left thigh was performed, which showed features consistent with an at least partially sampled immune-mediated necrotizing myopathy (IMNM).
Using the images, what is your diagnosis?
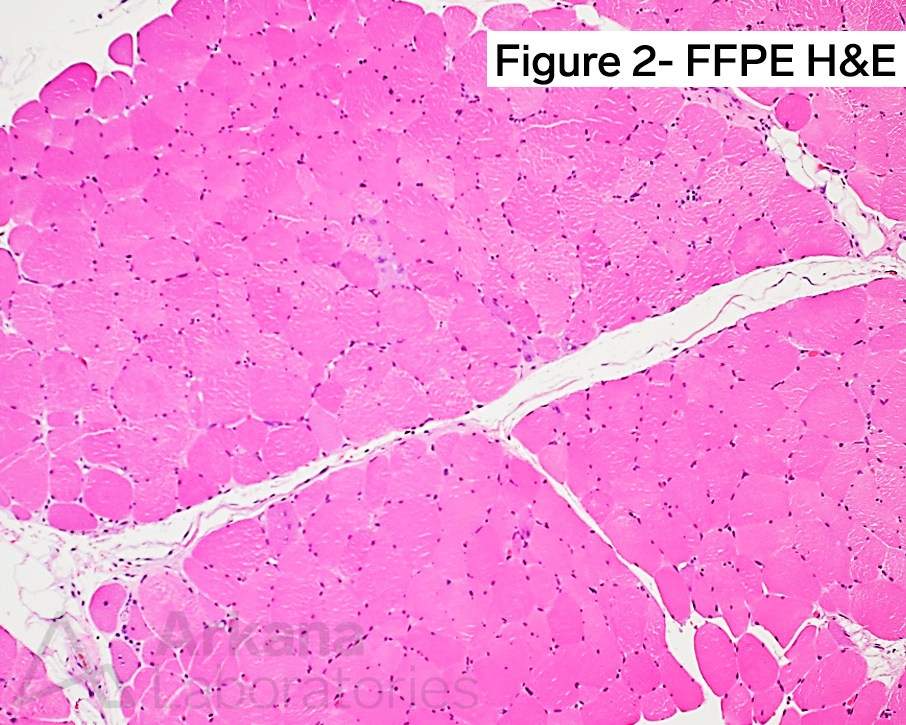
H&E-stained section of formalin-fixed paraffin-embedded (FFPE) tissue demonstrates similar features to those described in the frozen section material. Original magnification: A. Frozen H&E-stain, 100x; and B. FFPE H&E-stain, 100x.
Answer: Anti-U1-RNP Myositis
In the patient’s clinical context and autoimmune profile of positive anti-U1-RNP autoantibodies, these findings are those of a necrotizing myopathy, most compatible with anti-U1-ribonucleoprotein (RNP)-related myositis/myopathy, answer choice (D). See references.
Muscle biopsies from patients with positive anti-U1-RNP autoantibodies typically show necrotizing features; therefore, one approach this diagnosis is to assign a necrotizing myopathy injury pattern to the overall findings. This in combination with increased MHC1 (HLA-ABC) immunostaining (not shown in this case), favors an immune-mediated process (i.e. immune-mediated necrotizing myopathy, IMNM).
Recent literature states that the most common extramuscular findings in these patients are arthritis, dermatitis, and interstitial lung disease (ILD).
Why were the other answers wrong?
The clinical vignette helps to clarify the patient’s autoimmune profile, which shows that the patient is negative for anti-signal recognition particle (anti-SRP) and negative for anti-3-hydroxy-3-methylglutaryl-coenzyme A reductase (anti-HMGCR). The positive anti-U1-RNP and the necrotizing myopathic features in Figure 1, point one to the correct diagnosis.
Classical teaching puts anti-HMGCR, anti-SRP, and seronegative etiologies into the class of prototypical immune-mediated necrotizing myopathies (IMNMs).
Anti-HMGCR is most commonly associated with statin medication; however, a significant subset (up to ~30%) of patient may be statin naïve.
Seronegative etiologies may present an unique diagnostic dilemma, and one may suggest possible a paraneoplastic syndrome associated with occult neoplasia. Clinical work-up will help to further elevated these patients.
References
Casal-Dominguez M, Pinal-Fernandez I, Corse AM, et al. Muscular and extramuscular features of myositis patients with anti-U1-RNP autoantibodies. Neurology. 2019 Mar 26;92(13):e1416-e1426. PMID: 30824556.
Coppo P, Clauvel JP, Bengoufa D, et al. Inflammatory myositis associated with anti-U1-small nuclear ribonucleoprotein antibodies: a subset of myositis associated with a favourable outcome. Rheumatology (Oxford). 2002 Sep;41(9):1040-6. PMID: 12209039.
Pinal-Fernandez I, Casal-Dominguez M, Mammen AL. Immune-Mediated Necrotizing Myopathy. Curr Rheumatol Rep. 2018 Mar 26;20(4):21. PMID: 29582188.
Watanabe Y, Uruha A, Suzuki S, et al. Clinical features and prognosis in anti-SRP and anti-HMGCR necrotising myopathy. J Neurol Neurosurg Psychiatry. 2016 Oct;87(10):1038-44. PMID: 27147697.
Quick note: This post is to be used for informational purposes only and does not constitute medical or health advice. Each person should consult their own doctor with respect to matters referenced. Arkana Laboratories assumes no liability for actions taken in reliance upon the information contained herein.