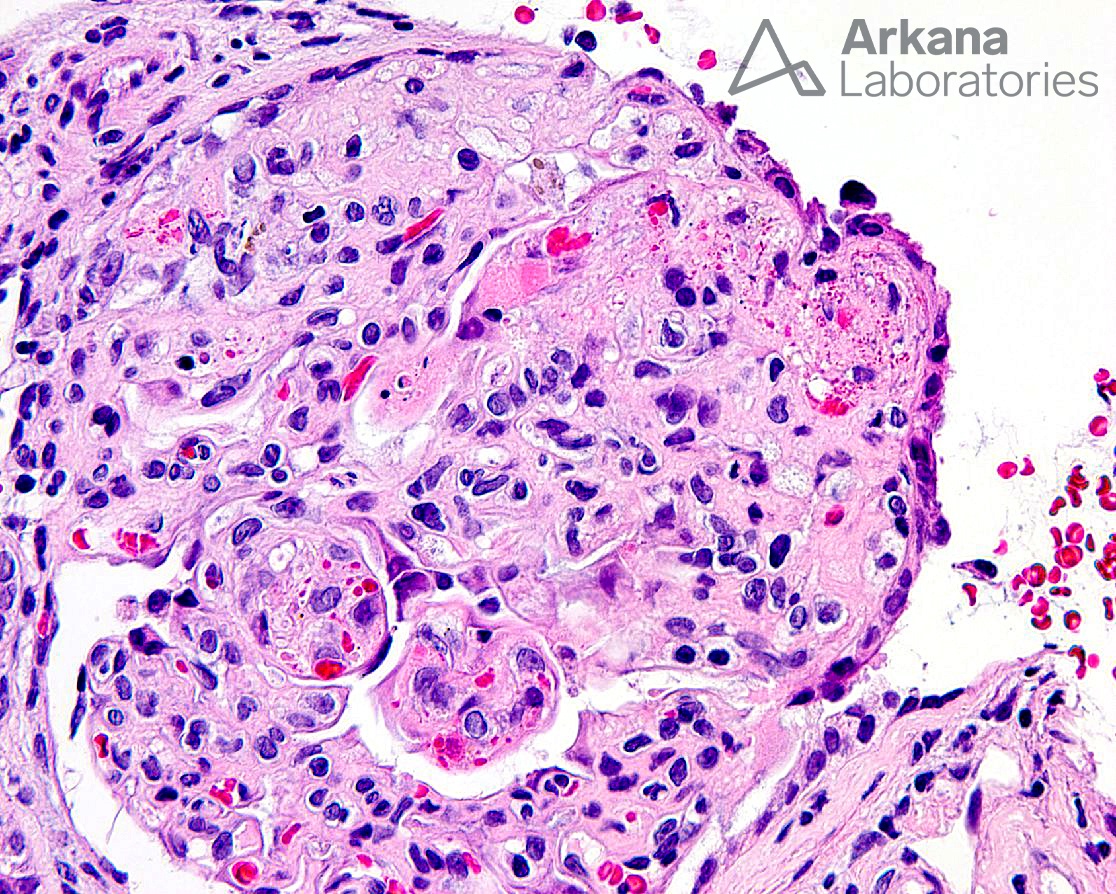
What is your diagnosis and possible differential for the finding?
The light microscopic image of an H&E stain depicts a glomerulus with areas of mesangiolysis, endothelial cell swelling with occlusion of capillary loops, numerous entrapped and fragmented red blood cells, and focal fibrin material, consistent with an acute thrombotic microangiopathy. Other glomerular findings that may be seen in the acute phase include a “bloodless” appearance, capillary loop thickening, and ischemic collapse of the glomerular tuft. The tubulointerstitium typically shows non-specific tubular injury, interstitial edema, and, in severe cases, cortical necrosis. Blood vessels in the acute phase will show similar features as seen in glomeruli with swollen endothelial cells, intimal mucoid edema with entrapped and fragmented red blood cells, and intraluminal fibrin thrombi.
Chronic changes seen in a case of thrombotic microangiopathy include duplication of the glomerular basement membranes, areas of mesangial expansion and mesangiolysis, arterioles with intimal fibrosis and narrowing of the vessel lumen along with concentric lamination of the intima (i.e. “onion skinning”).
The differential diagnosis for TMA is long and includes, but is not limited to, TTP, HUS secondary to Shiga-toxin producing bacteria (i.e. E. coli), atypical HUS, drugs (such as cyclosporine), bone marrow transplant, radiation, pregnancy, malignant hypertension, malignancies, autoimmune disease, and others. In this case, our patient presented with severe headache and malignant hypertension.
Reference:
Brocklebank V et al. Thrombotic Microangiopathy and the Kidney. Clin J Am Soc Nephrol. 2018 Feb 7;13(2):300-317.
Quick note: This post is to be used for informational purposes only and does not constitute medical or health advice. Each person should consult their own doctor with respect to matters referenced. Arkana Laboratories assumes no liability for actions taken in reliance upon the information contained herein.