In this episode of Banff and Beyond, we continue the discussion on infections that occur in the transplant setting.
The patient today is a 73-year-old male with AKI and increased urine frequency status post-transplant ~3.5 yrs. ago. Past medical history includes diabetes, hypertension, CAD, and prior prostate cancer. The patient was started on Augmentin empirically for presumptive UTI, however, this was discontinued when cultures were found to be negative. As we look at the biopsy from low power, we can appreciate that there is minimal “blue” throughout the majority of the interstitium however one area does show a patch of dense interstitial inflammation. On higher magnification, we can see the interstitial infiltrate is composed of lymphocytes, plasma cells, histiocytes, and neutrophils. In addition to the brisk inflammation, there are white blood cell casts, apoptotic debris, and reactive appearing tubular epithelial nuclei. Lymphocytic and neutrophilic tubulitis is also present along with rare tubules showing tubular epithelial necrosis with epithelial sloughing.
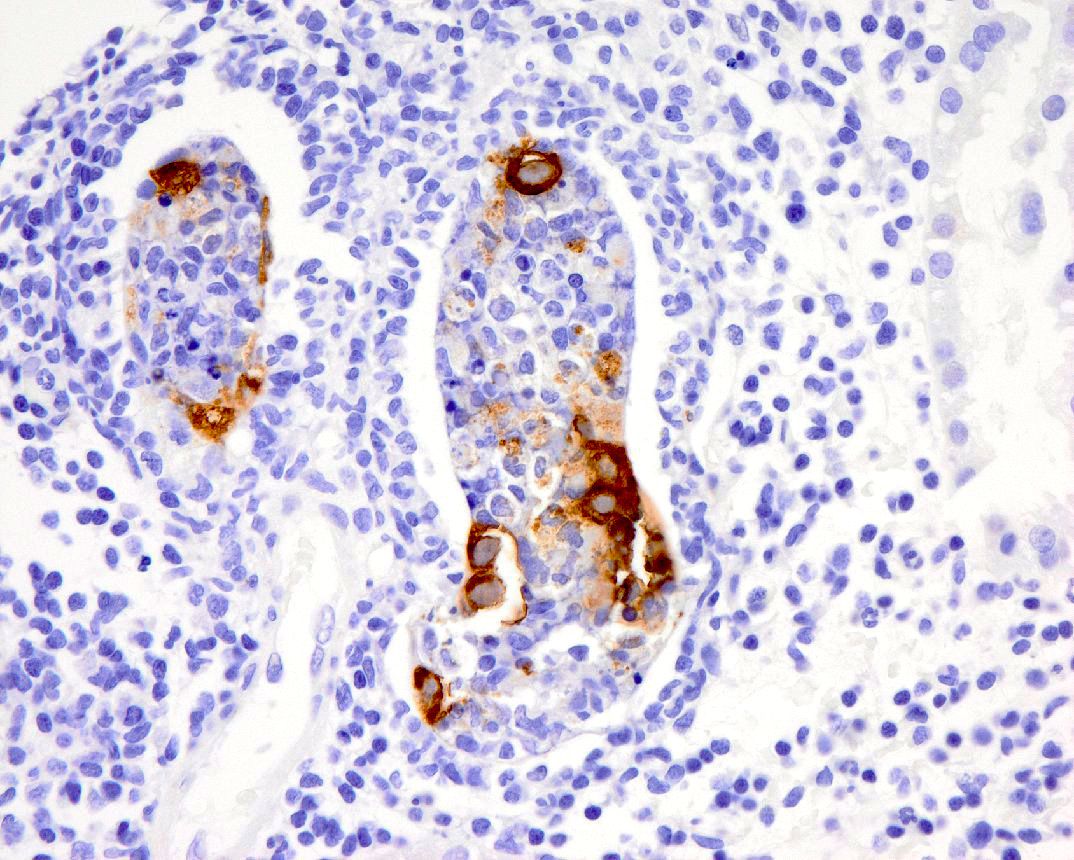
This constellation of findings is again suspicious for an underlying viral infection, and while our SV40 stain is negative, the adenovirus stain was focally positive in the tubular nuclei within the area of brisk interstitial inflammation. The patient was subsequently found to have a positive adenovirus titer and was treated appropriately.
Quick note: This post is to be used for informational purposes only and does not constitute medical or health advice. Each person should consult their own doctor with respect to matters referenced. Arkana Laboratories assumes no liability for actions taken in reliance upon the information contained herein.