Hello everyone and welcome back to Banff and Beyond!
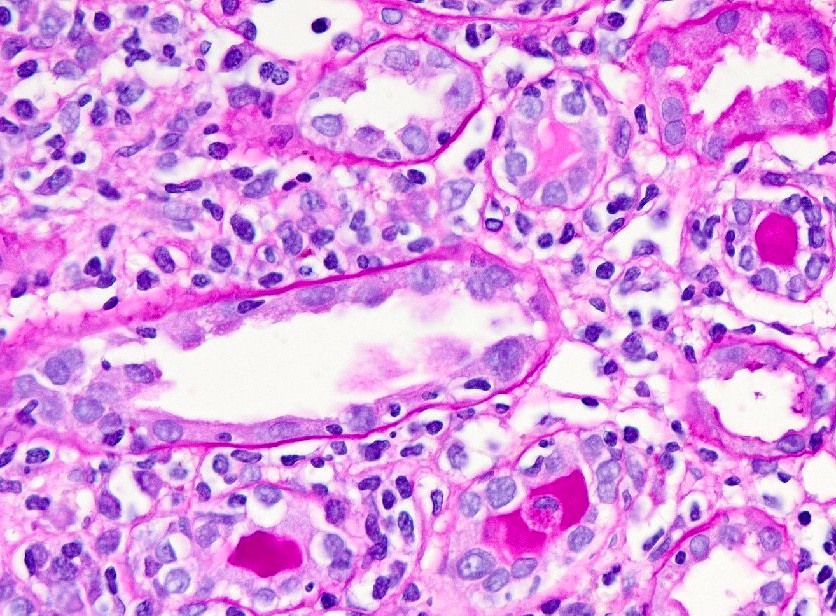
Today’s episode is a biopsy from a 40 y/o male status post-transplant of approximately 1.5-2 yrs. ago who presents for routine follow-up. Pertinent clinical history also includes a previous autologous stem cell transplant for myeloma. Laboratory evaluation reveals a serum Cr: 1.4 mg/dL. At low power, we can see we have a good sample of cortex with multiple glomeruli. Next, as we continue to evaluate our biopsy, we can see we have a small portion of interstitial “blue” or interstitial inflammation which overall comprised approximately 10-15% of the entire sample and, at higher power, we can see that the infiltrate is predominately lymphocytic with scattered plasma cells. In addition, we also have moderate tubulitis within non-atrophic tubules; thus, with an “I1” “T2” we have met the criteria for borderline T-cell mediated rejection. However, now as we continue our exam of the case, we can see we have mesangial matrix expansion with mesangial hypercellularity as well as segmental endocapillary hypercellularity. Moving to our immunofluorescence, we can see we have granular mesangial staining with IgG, C3, C1q, and kappa while lambda is negative. Additionally, IgG subtypes demonstrate staining with IgG3 while all others are negative. By electron microscopy, we can see mesangial electron-dense deposits correlating with our immunofluorescence pattern. So, in addition to borderline rejection, the biopsy demonstrates an entity known as proliferative glomerulonephritis with monoclonal immunoglobulin deposits or PGMID. Thanks for stopping by for this interesting case and see you next time!
Quick note: This post is to be used for informational purposes only and does not constitute medical or health advice. Each person should consult their own doctor with respect to matters referenced. Arkana Laboratories assumes no liability for actions taken in reliance upon the information contained herein.