Post-Streptococcal Acute Glomerulonephritis (PSAGN)
Clinical Presentation:
A 15-year-old male presented with a two-week history of decreased urine output, edema, and dark urine. He reported a recent history of a pharyngitis illness, for which he was treated with amoxicillin. Laboratory tests revealed proteinuria, hematuria, and elevated creatinine. A kidney biopsy was performed.
Kidney Biopsy Findings:
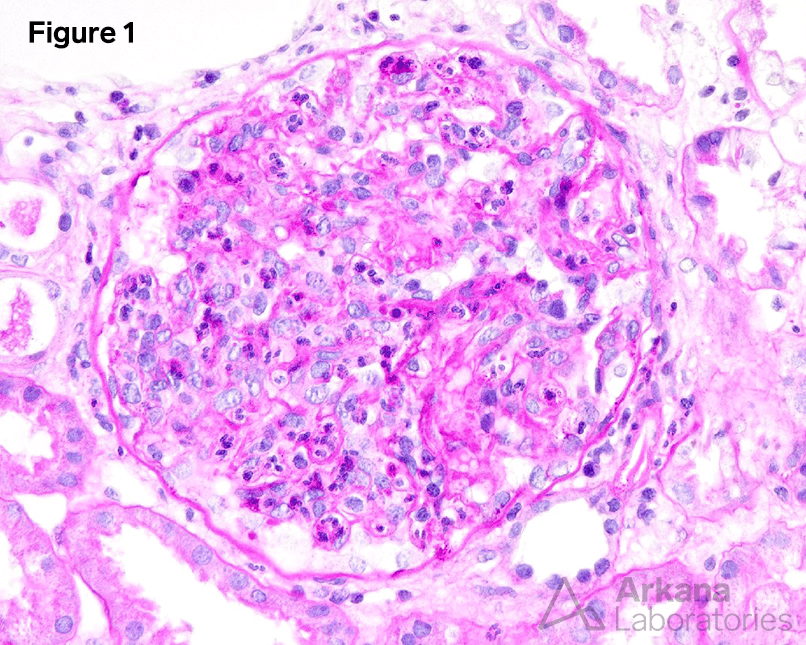
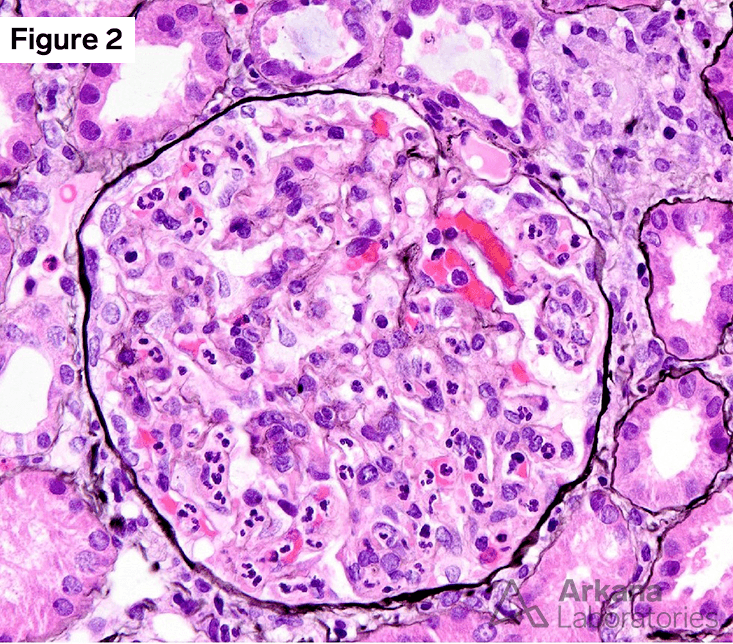
Figures 1 and 2 show the main finding on light microscopy (PAS and Jones silver stain respectively). There is diffuse endocapillary proliferative and exudative glomerulonephritis composed of mononuclear cells and numerous neutrophils. No crescent was identified. The tubules showed evidence of minimal to mild degenerative changes, and the interstitial space showed edema and mild infiltration.
Additional Clues:
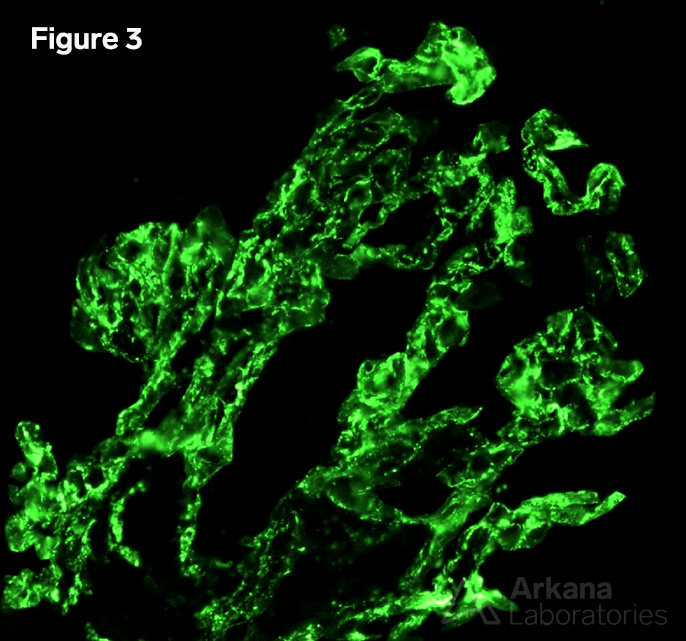
Our final clues are seen on immunofluorescence, which shows granular mesangial and capillary loop staining for C3 (shown below), while all other stains are negative in glomeruli.
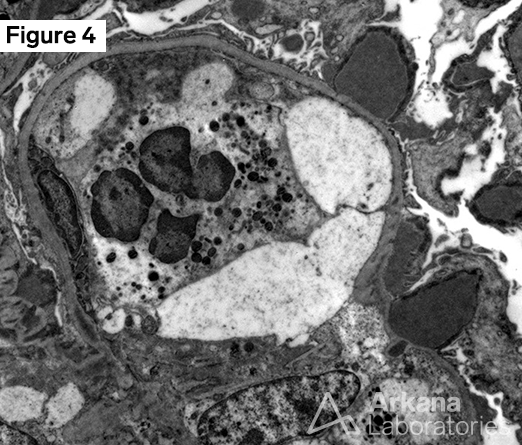
Finally, ultrastructural examination by electron microscopy showed frequent subepithelial “hump-like” deposits on the glomerular basement membranes and scattered mesangial electron-dense deposits. No subendothelial or intramembranous deposits were seen.
Diagnosis: Post-Streptococcal Acute Glomerulonephritis (PSAGN):
The biopsy confirmed the diagnosis of post-streptococcal acute glomerulonephritis (PSAGN). PSAGN is a type of kidney disease that occurs after a Streptococcus infection. PSAGN typically develops 1-3 weeks after a streptococcal infection such as strep throat or impetigo. The enigma of PSAGN lies in its elusive nature. One moment, a person may be recovering from a routine respiratory infection, and the next, they find themselves struggling with kidney disease.
So how does a simple infection turn into a serious kidney disease?
PSAGN is likely caused by a combination of immune-mediated and direct toxic effects. The streptococcal infection triggers an immune response that not only targets the bacteria but also attacks the kidneys, leading to inflammation and damage to the glomeruli. The streptococcal bacteria’s surface M protein and other virulence factors facilitate infection, immune system evasion, and tissue damage. Additionally, streptococcal antigens, such as streptococcal pyrogenic exotoxin B, may be involved in the immune-complex formation, where antigen-antibody immune complexes deposit in glomeruli, leading to kidney damage.
Furthermore, the streptococcal bacteria produce neuraminidase that can directly activate complement and cause kidney damage. However, the exact mechanisms by which streptococcal infections lead to the development of glomerulonephritis are unclear and require further research.
Treatment typically involves addressing the underlying infection and providing supportive care. In some cases, immunosuppressive medications may be used to reduce the immune response and prevent further damage to the kidneys. Most cases of childhood PSAGN have a positive outcome. However, adult cases have a more uncertain outlook and carry an increased risk of end-stage renal disease.
References:
Colvin, Robert, B. and Anthony Chang. Diagnostic Pathology: Kidney Diseases. Available from: Elsevier eBooks+, (3rd Edition). Elsevier – OHCE, 2019.
Jennette JC, Olson JL, Silva FG, D’Agati V, Heptinstall RH *1920 *, eds. Heptinstall’s Pathology of the Kidney: Includes Interactive EBook with Complete Content. Seventh edition. Wolters Kluwer; 2015.
Nasr SH, Radhakrishnan J, D’Agati VD. Bacterial infection–related glomerulonephritis in adults. Kidney International.2013;83(5):792-803.
Quick note: This post is to be used for informational purposes only and does not constitute medical or health advice. Each person should consult their own doctor with respect to matters referenced. Arkana Laboratories assumes no liability for actions taken in reliance upon the information contained herein.