The patient is a 50-year-old female who presents 2 days after a renal transplant with a delay in graft function and a creatinine of 7. Her end-stage renal disease was due to diabetic glomerulopathy. She was on dialysis for 3 years. She received a kidney from a 22-year-old deceased donor (motorcycle accident). The kidney at time of transplant looked normal grossly and microscopically. What is the most likely cause of the patient’s delay in graft function?
A. Acute Cellular Rejection
B. Surgical manipulation of a vessel
C. Recurrent diabetes
D. Donor-derived disease
The correct answer is (B) surgical manipulation of a vessel.
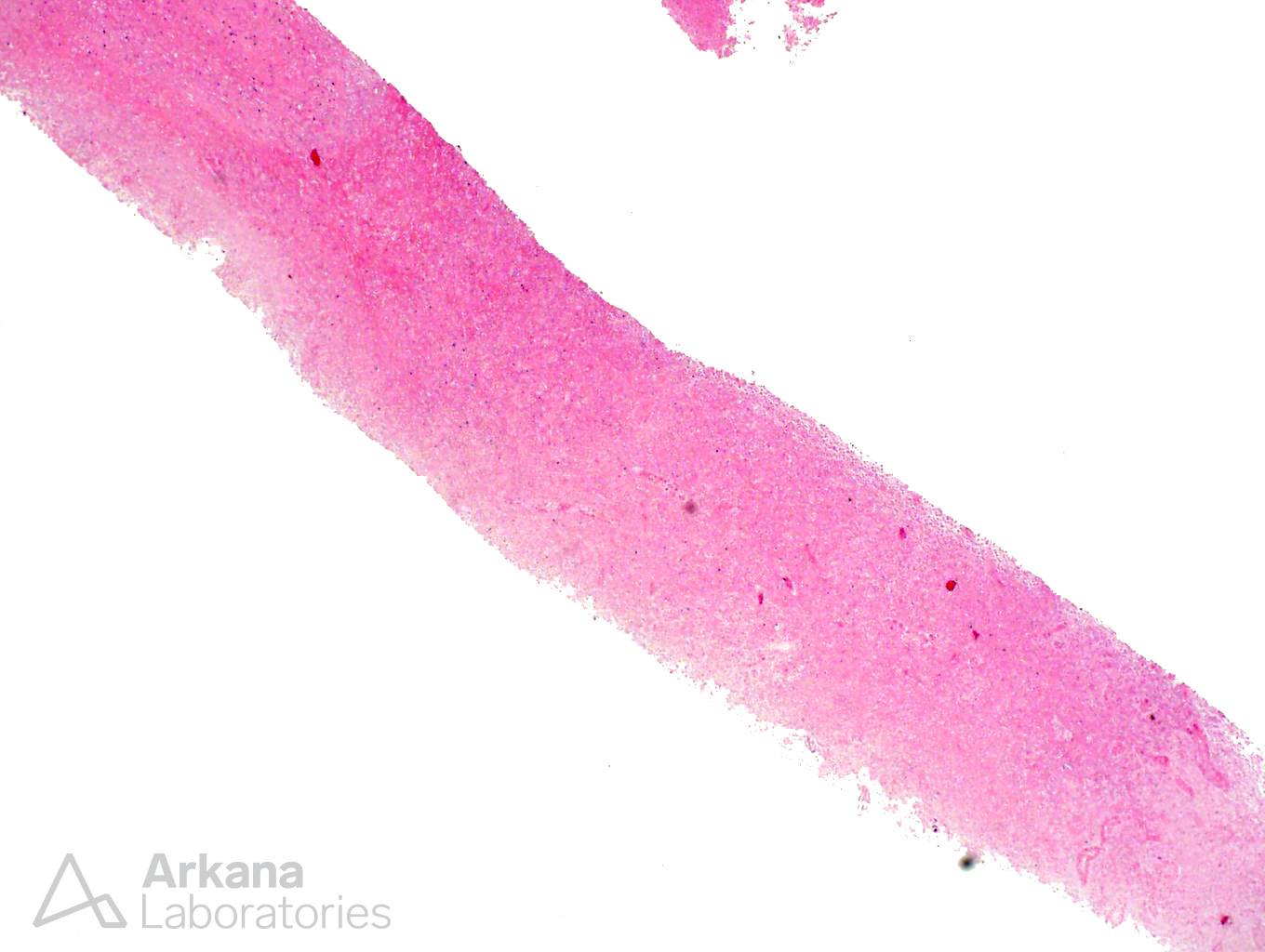
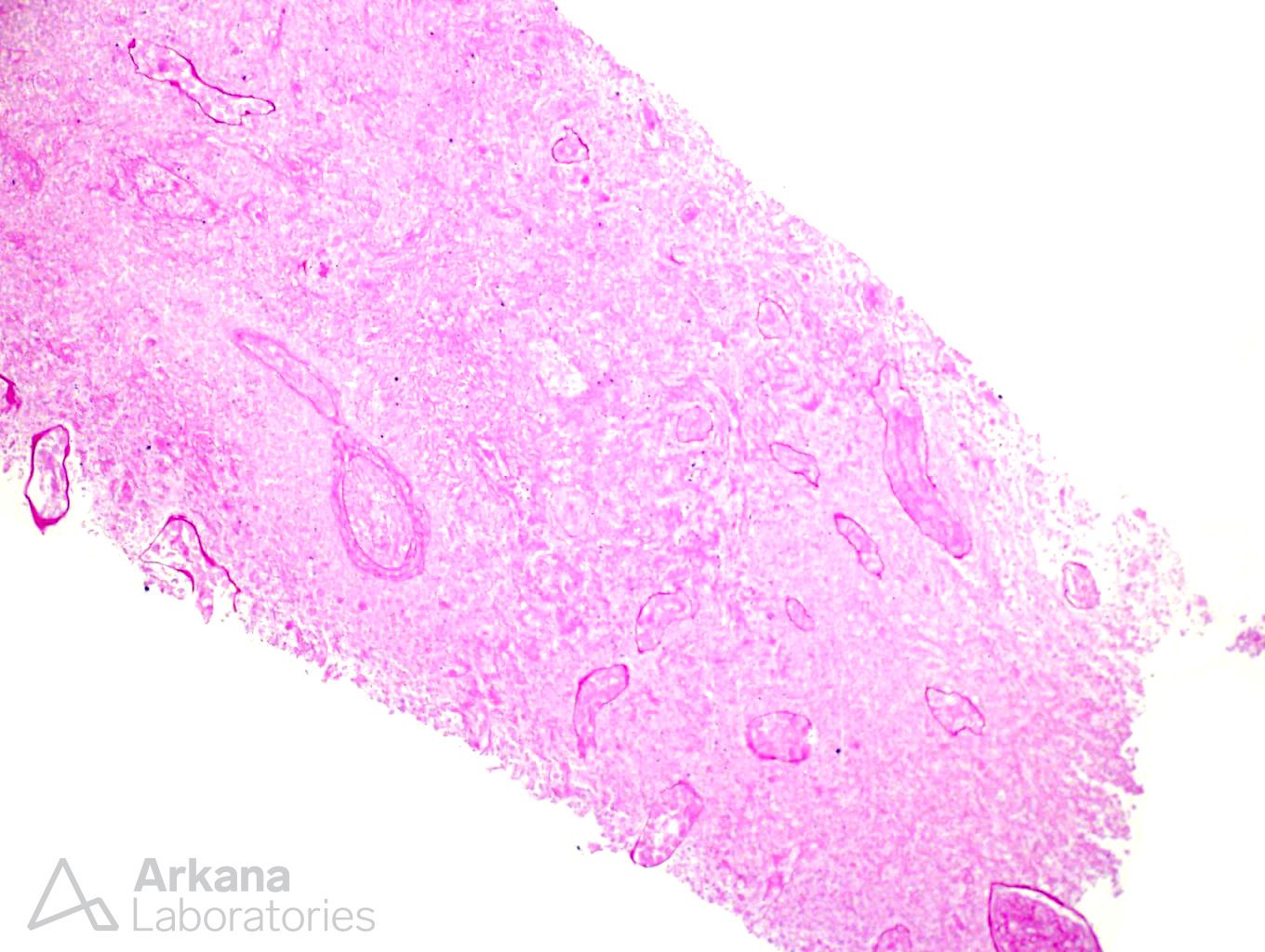
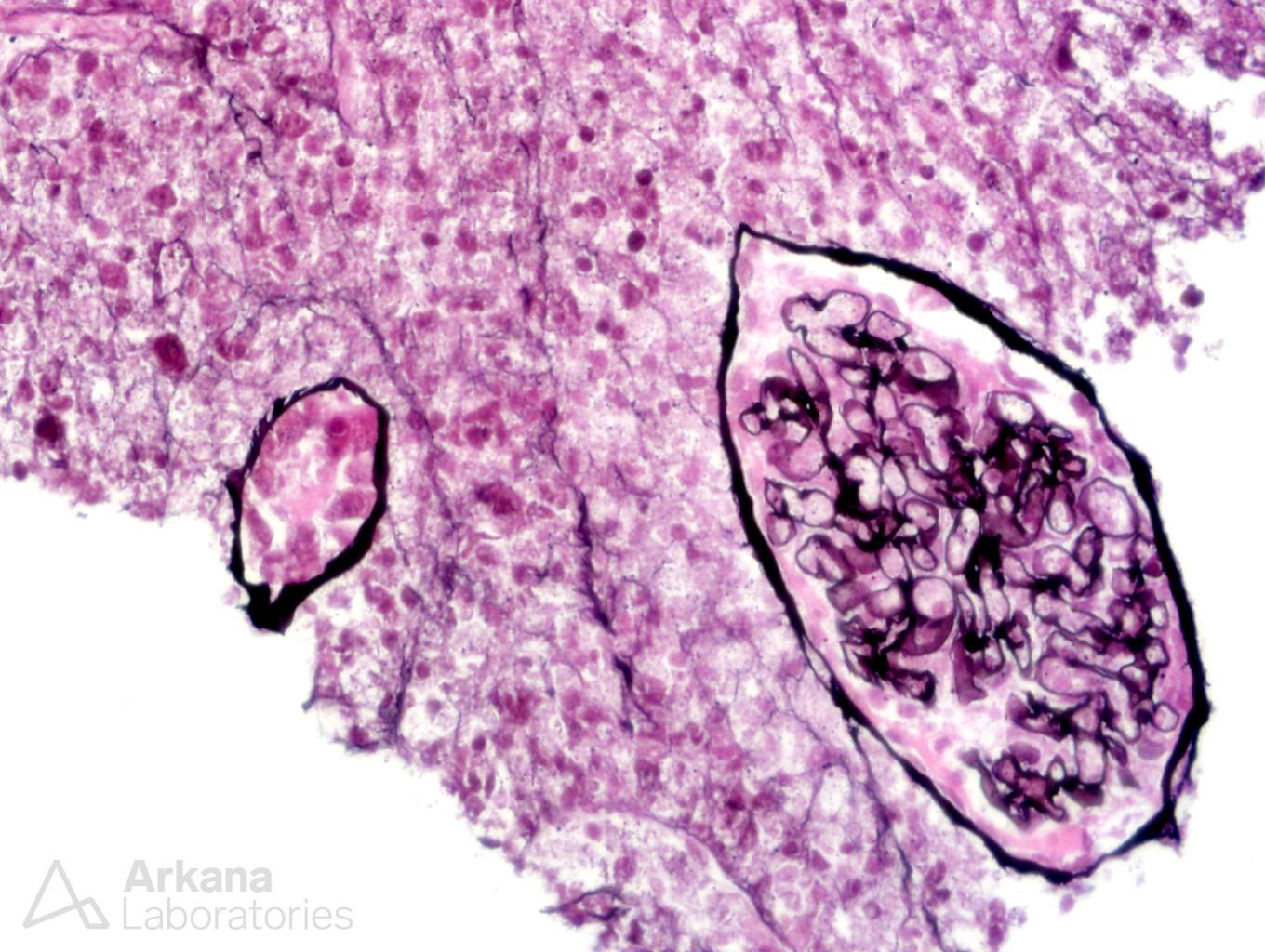
The biopsy shows diffuse coagulative necrosis. It is difficult to tell that this is kidney parenchyma on H&E, but silver and PAS stains outline the remnants of glomeruli and vessels. Surgical manipulation of a vessel is the best answer because this would explain the coagulative necrosis from occlusion of a feeding vessel during the transplant operation. Hyperacute rejection has been known to cause coagulative necrosis, but this form of rejection is extremely rare because of pretransplant cross matching studies. Hyperacute rejection is an antibody-mediated rejection which is a consequence of circulating preformed anti-donor antibodies in the recipient. Acute cellular rejection could theoretically cause coagulative necrosis, but you would see a cellular infiltrate and vasculitis and the rejection pattern of acute cellular rejection is usually not coagulative necrosis after only 2 days transplant. Recurrent diabetes would not occur this quickly and would not lead to coagulative necrosis. Donor-derived disease could potentially lead to coagulative necrosis from hypotension, but the kidney would not look normal grossly and microscopically at the time of transplant.
Quick note: This post is to be used for informational purposes only and does not constitute medical or health advice. Each person should consult their own doctor with respect to matters referenced. Arkana Laboratories assumes no liability for actions taken in reliance upon the information contained herein.