The patient is an 80 year-old male who presents with fatigue and a creatinine of 6.5 mg/dl. He was in his normal state of health until he and his grandchild went to the park on a hot afternoon. Subsequently, he began to feel ill and fatigued and went to see his physician. He has a past medical history significant for long-standing hypertension which is treated with a loop diuretic. Based on this history and images, what is the best diagnosis?
A. Waldenstrom macroglobulinemia
B. Light Chain Deposition Disease secondary to lymphoplasmacytic lymphoma
C. Light Chain Deposition Disease secondary to small lymphocytic lymphoma
D. Amyloidosis, AL-type
The best answer is (B) light chain deposition disease secondary to lymphoplasmacytic lymphoma
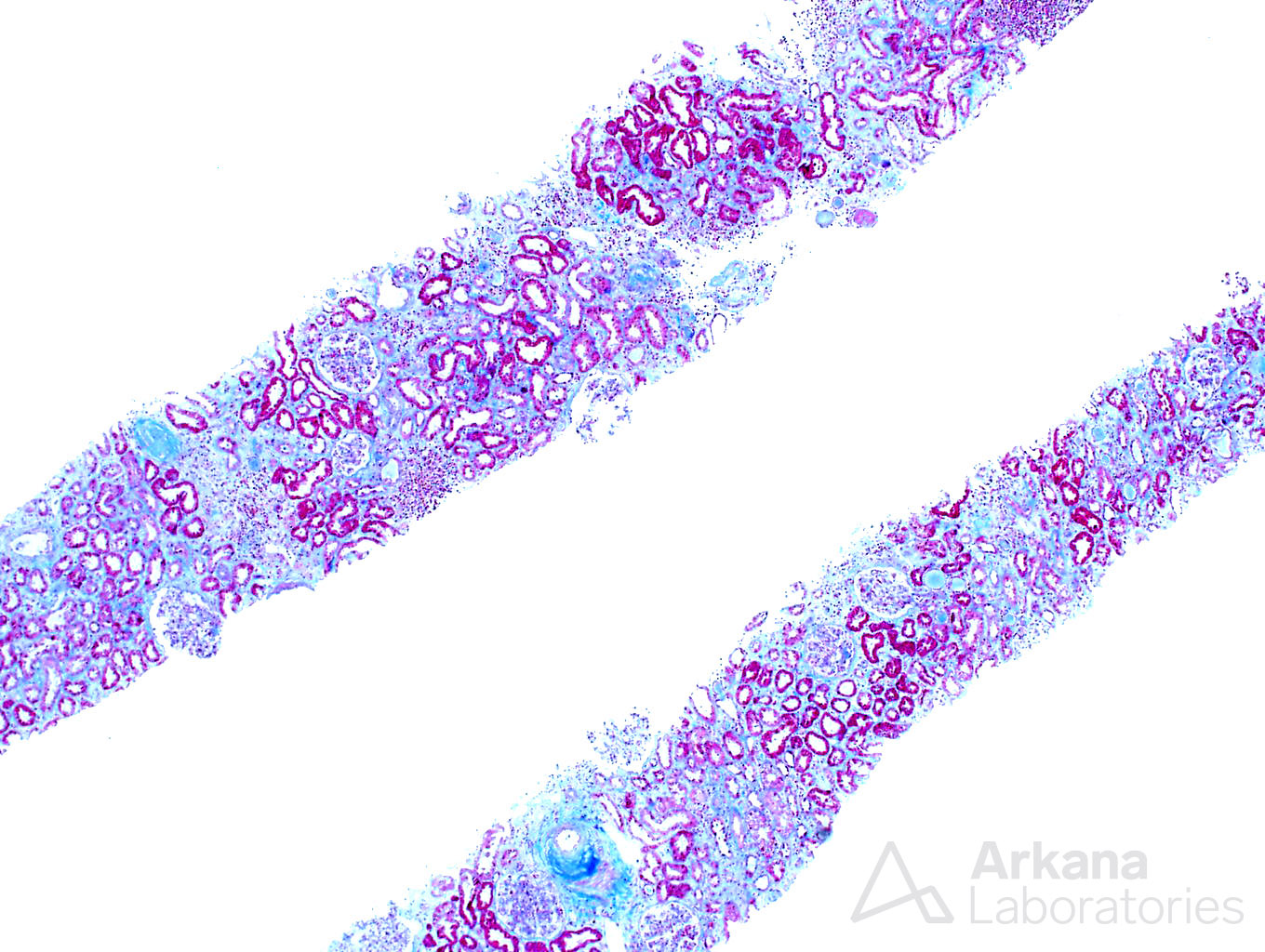
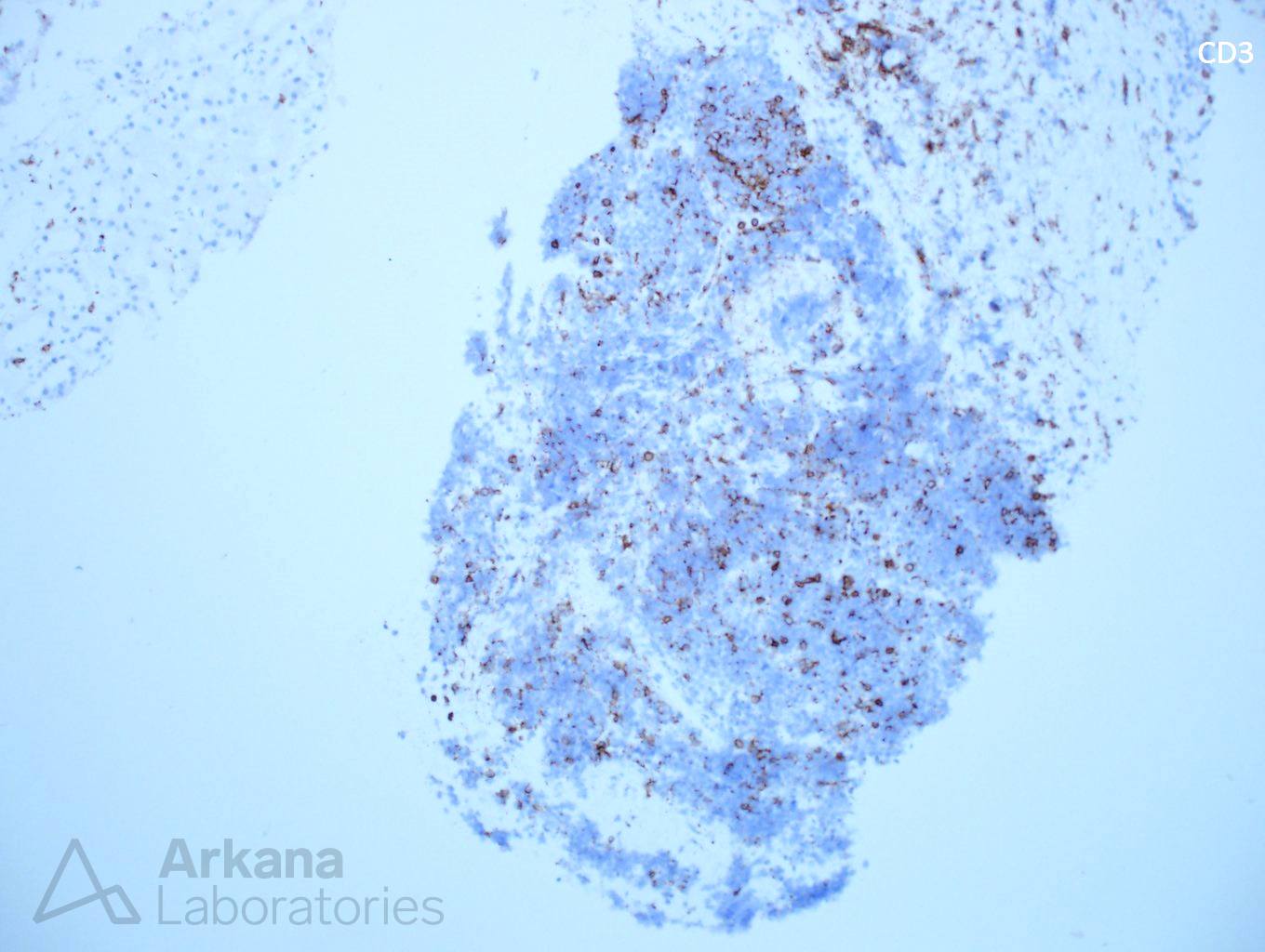
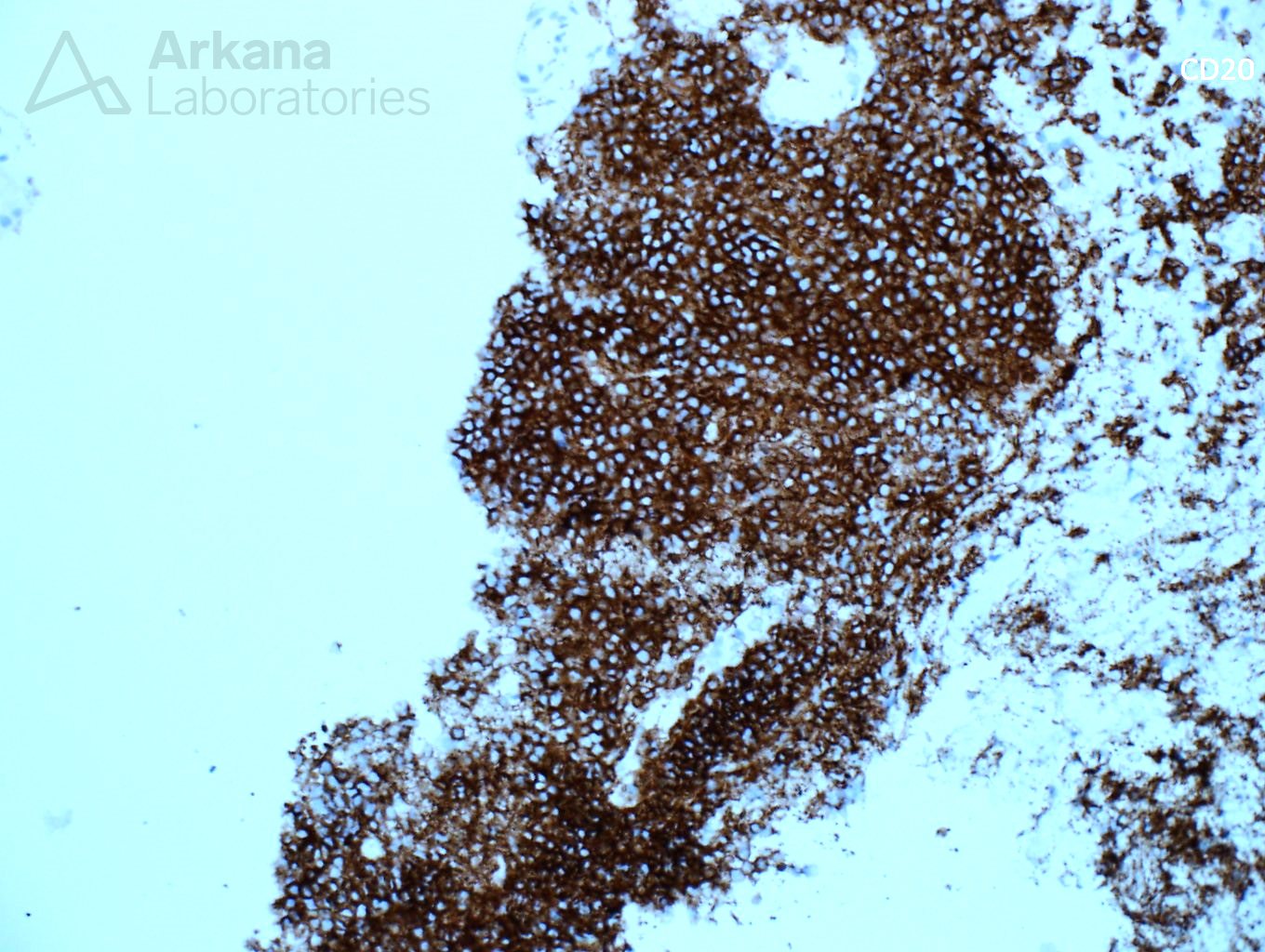
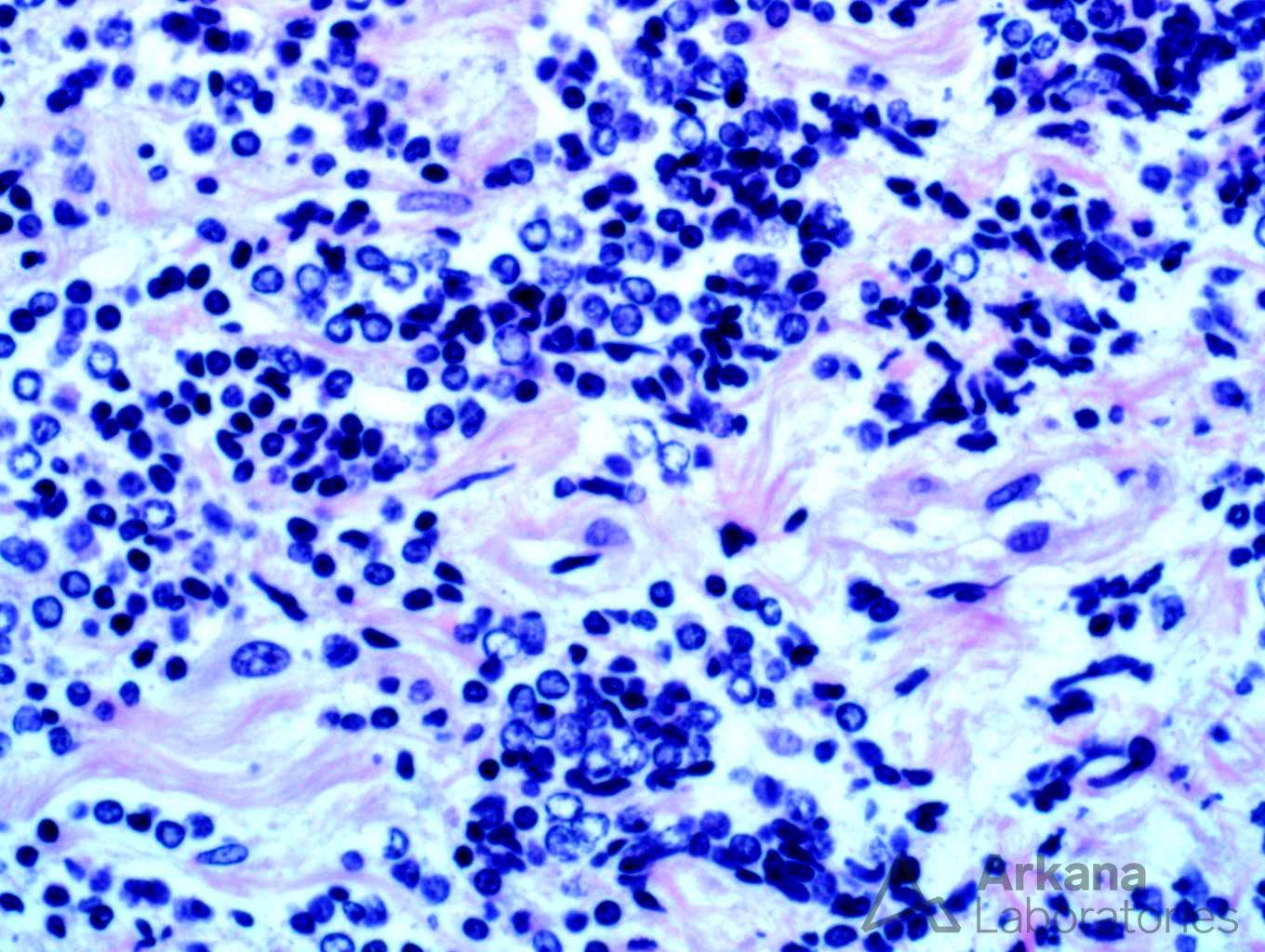
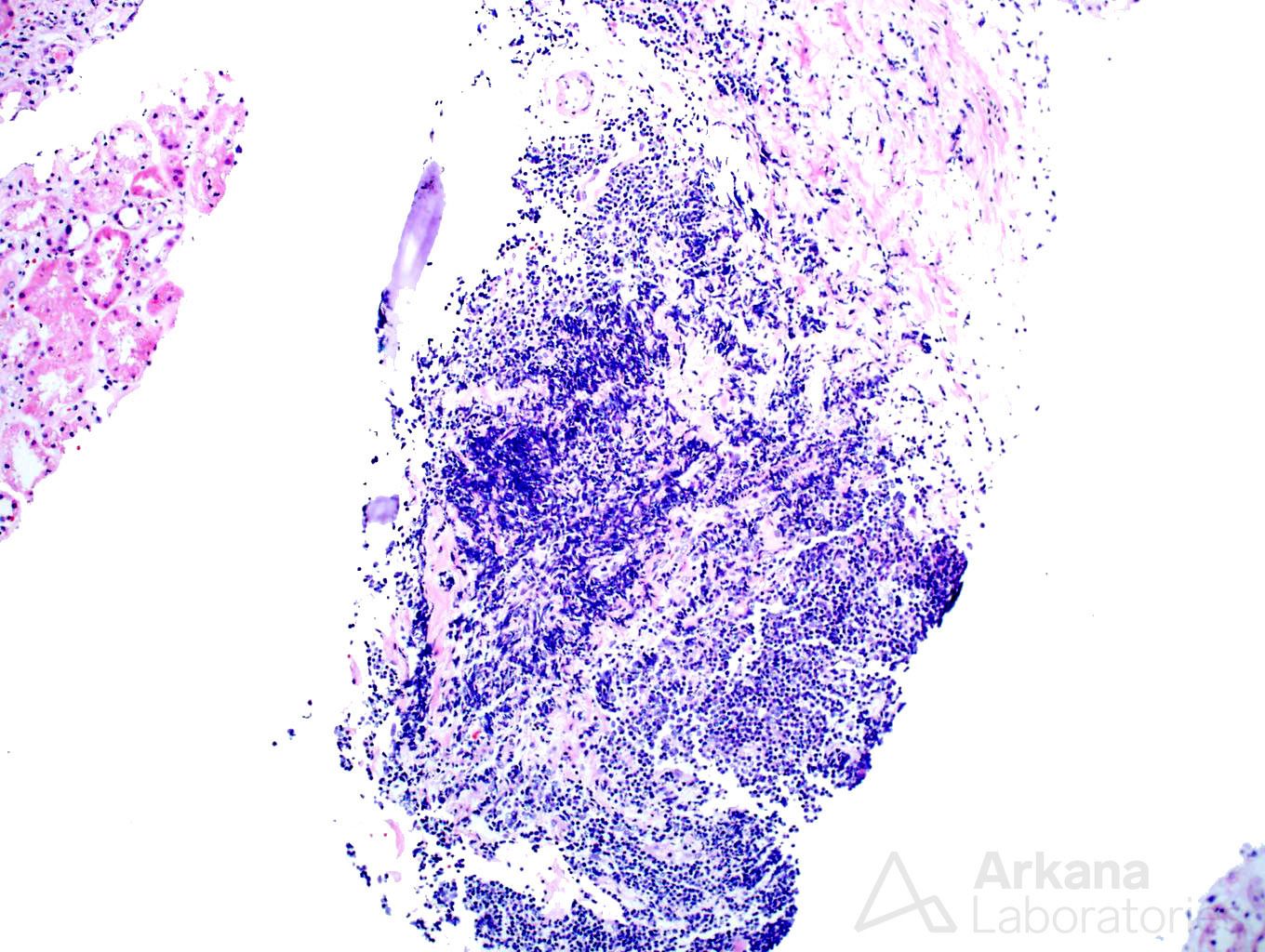
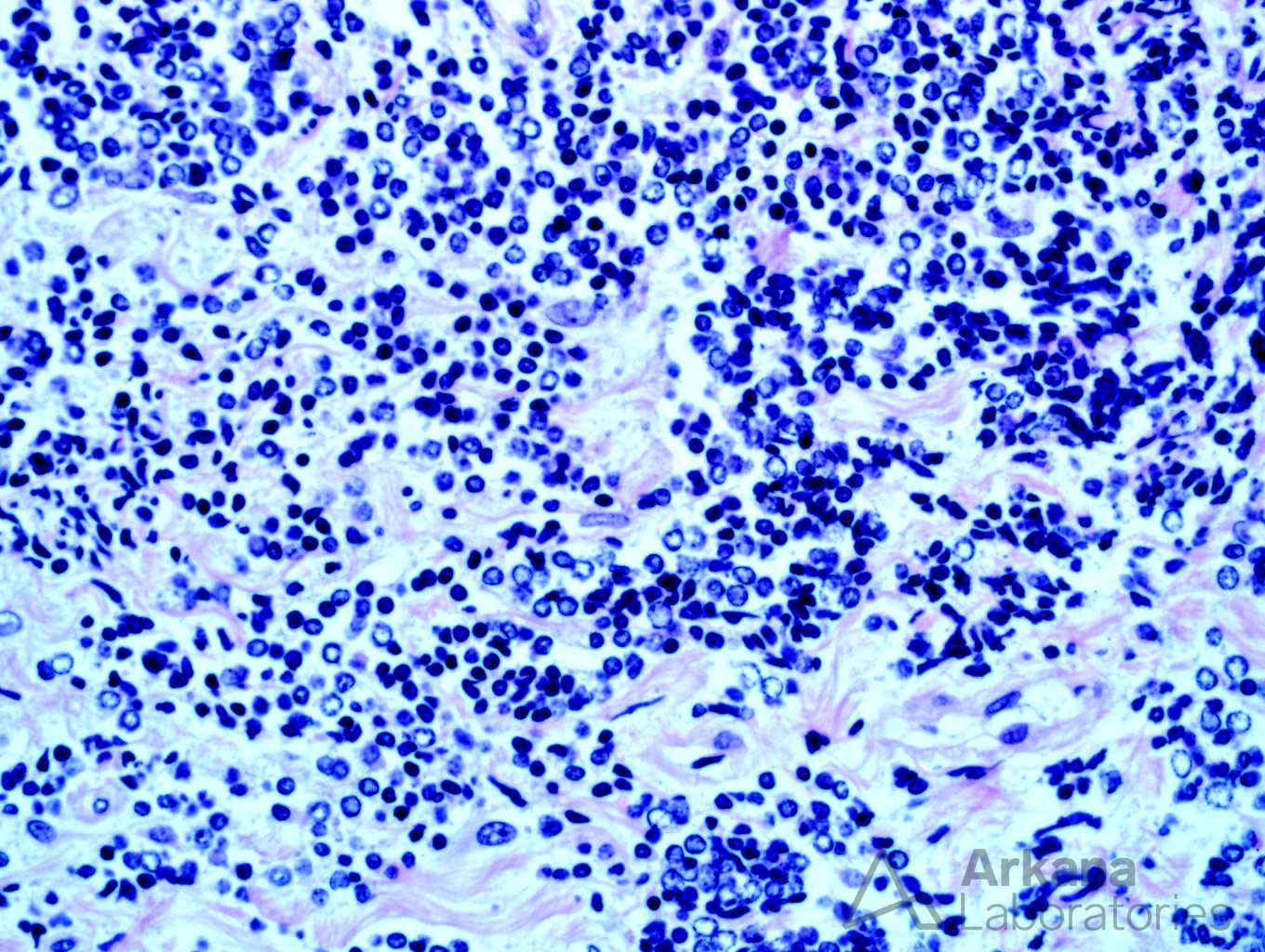
Explanation: The biopsy shows a combination of dense, atypical lymphocytic infiltrate, and light chain deposition disease. On high power examination, the lymphocytes are small, monotypic, and show occasional nucleoli. Small cell lymphoma (SLL) typically shows CD20 and CD5 staining, however, in this case, no CD5 staining is present, excluding this possibility. However, the presence of intense CD20 staining in the absence of CD3, CD5, and CD10 is atypical and suggests a lymphoma with strong B-cell differentiation, such as lymphoplasmacytic lymphoma.
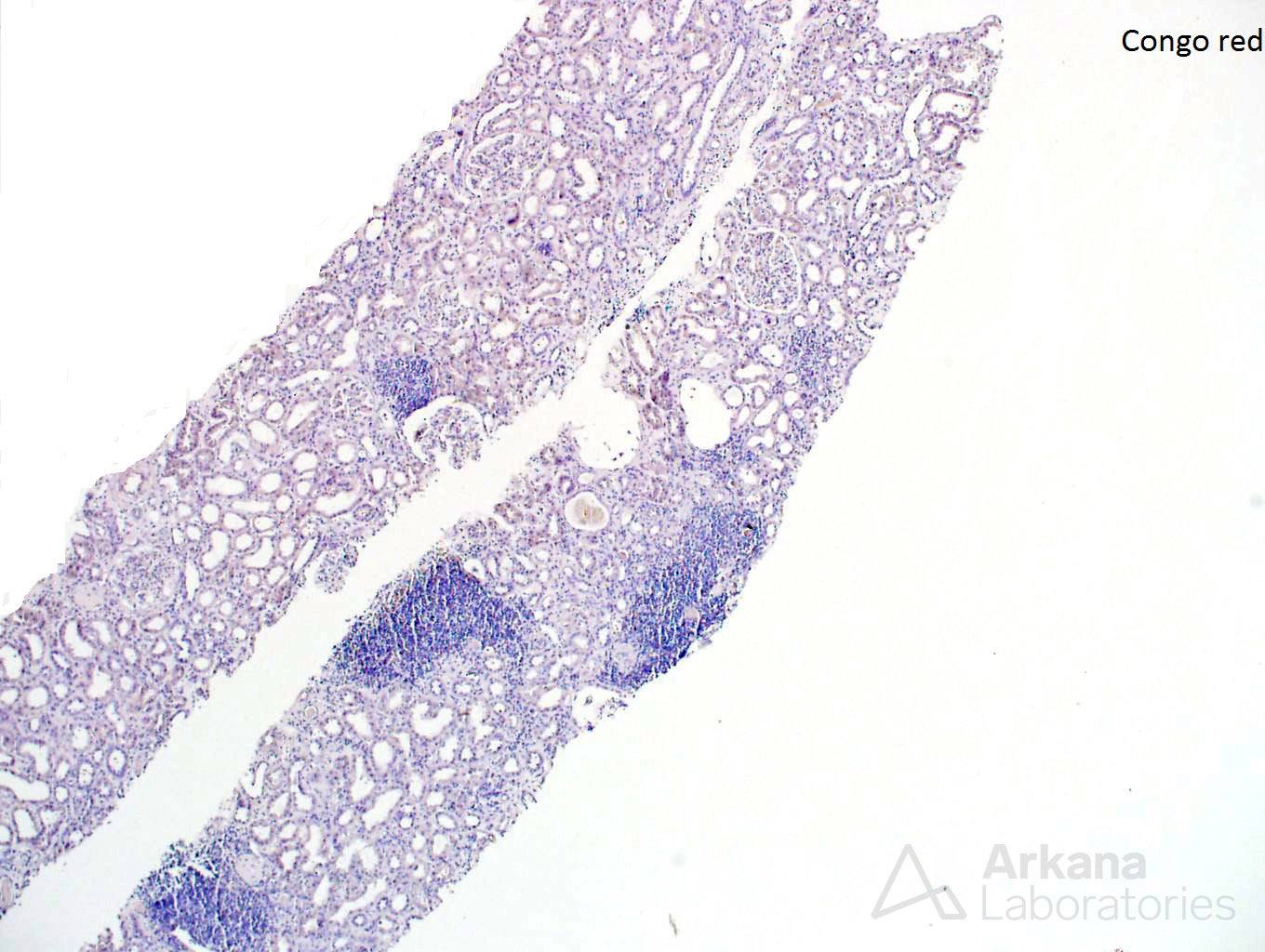
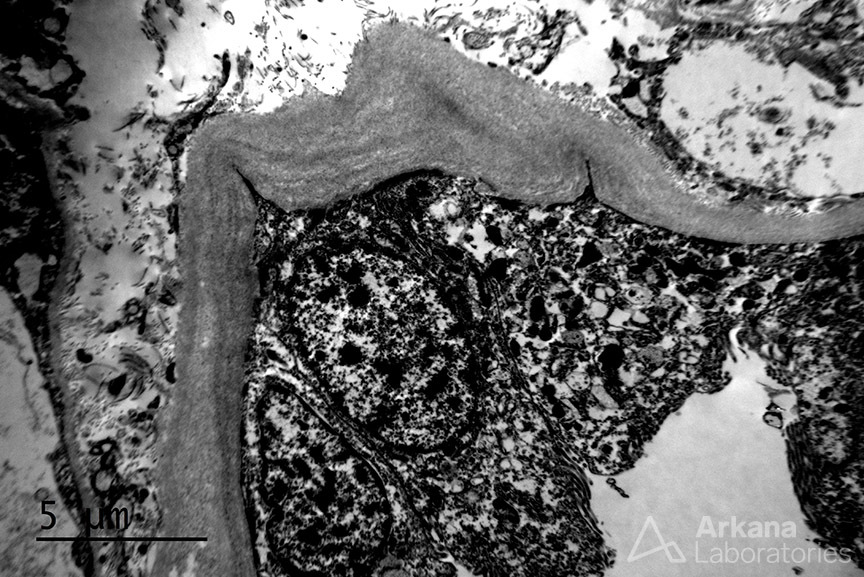
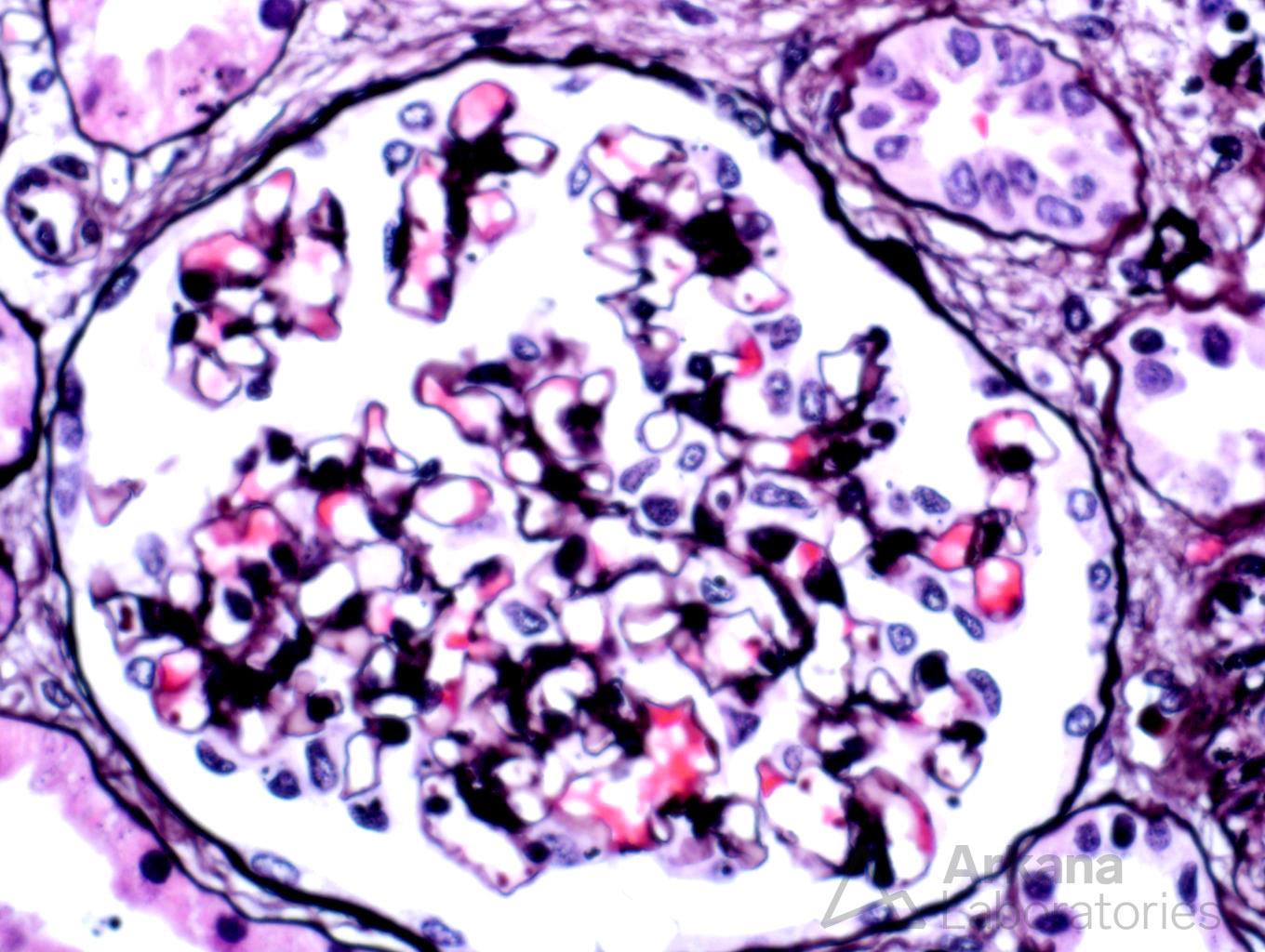
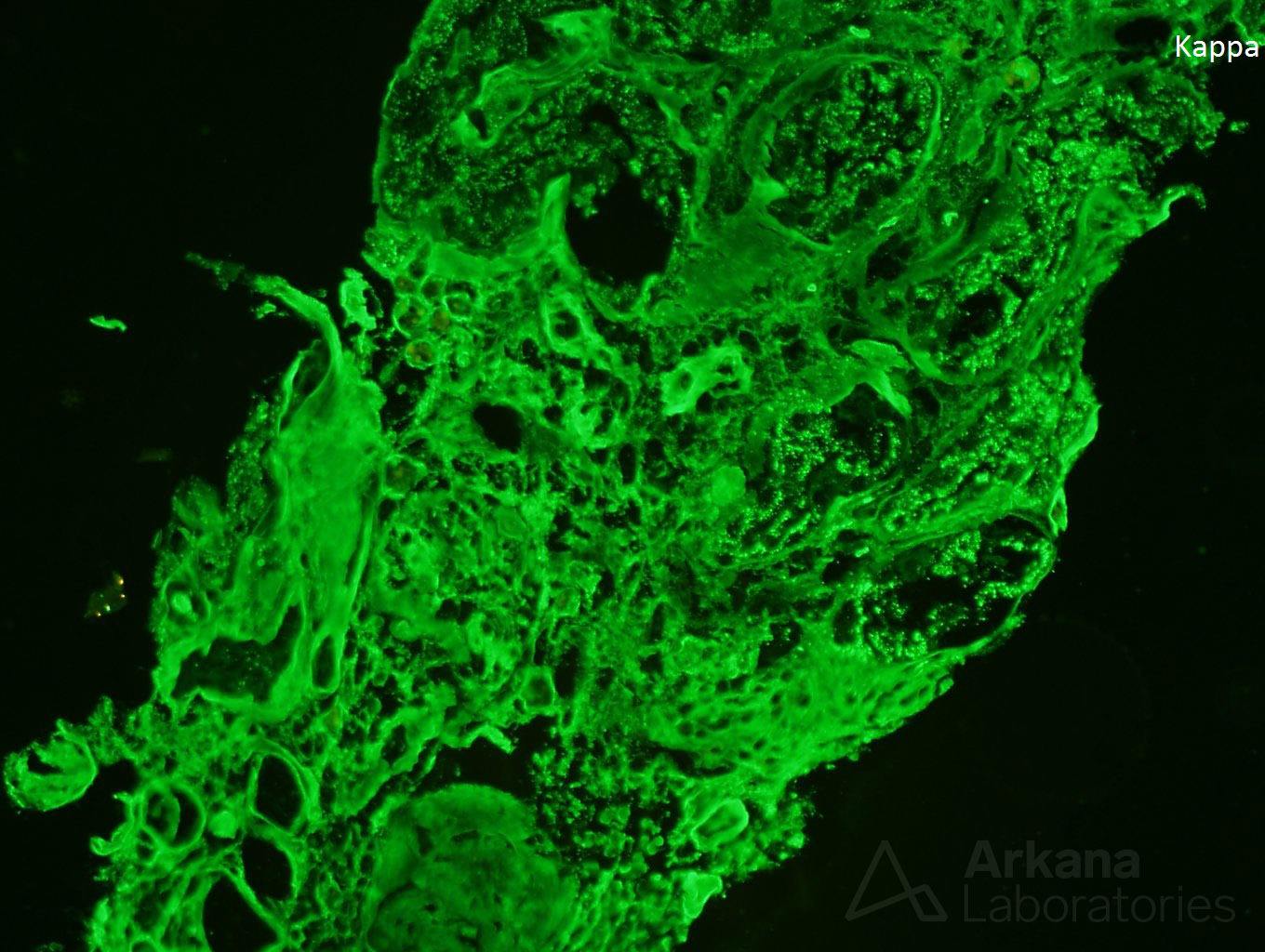
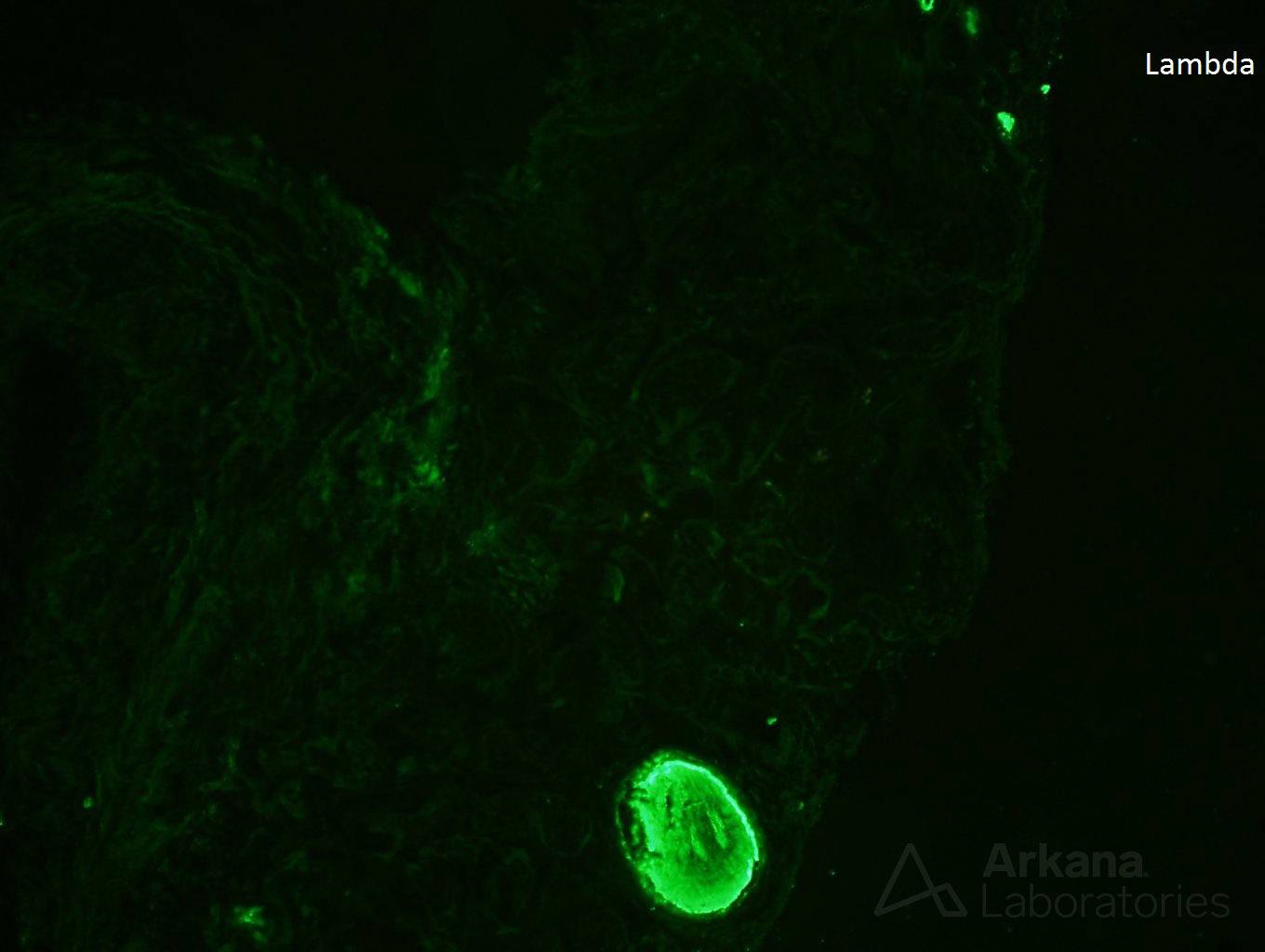
While lymphoplasmacytic lymphoma is a known cause of Waldenstrom macroglobulinemia the morphology, in this case, is not consistent with this diagnosis. There are no ‘hyaline thrombi’ within glomeruli and the pattern of immunofluorescence staining does not show the typical IgM deposition with light chain restriction within glomeruli needed to confer this diagnosis. However, the presence of kappa light chain restriction within the tubular basement membranes and powdery, electron-dense tubular basement membrane deposits by electron microscopy is diagnostic of light chain deposition disease. And, although amyloidosis can be seen as a consequence of lymphoplasmacytic lymphoma, the Congo red stain shows no positivity excluding this possibility.
Quick note: This post is to be used for informational purposes only and does not constitute medical or health advice. Each person should consult their own doctor with respect to matters referenced. Arkana Laboratories assumes no liability for actions taken in reliance upon the information contained herein.