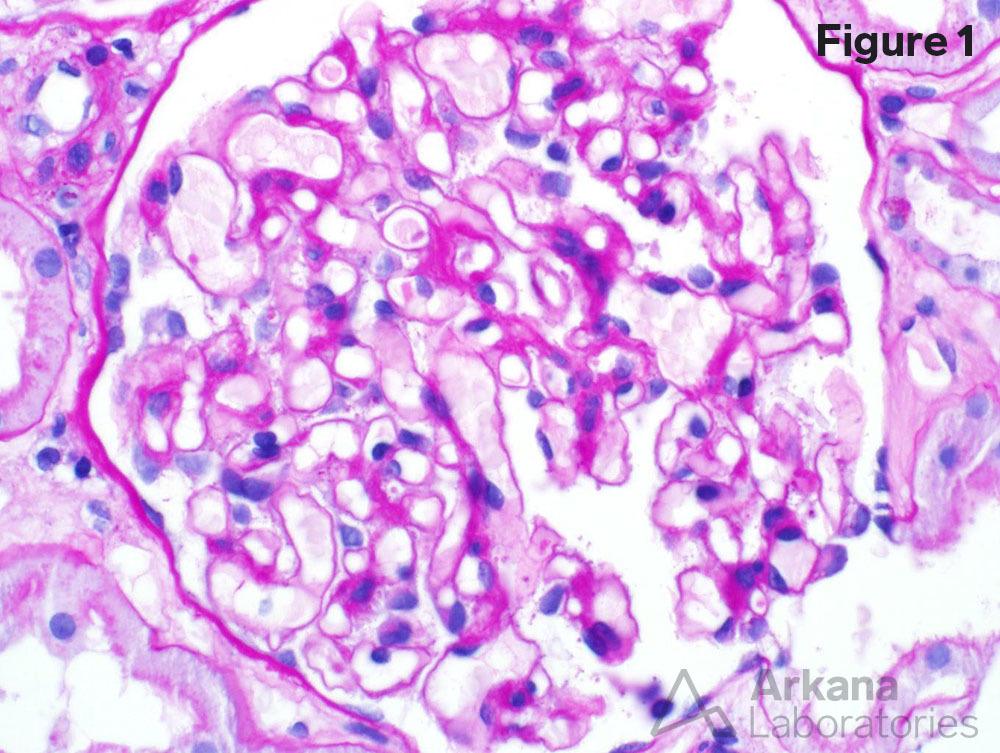
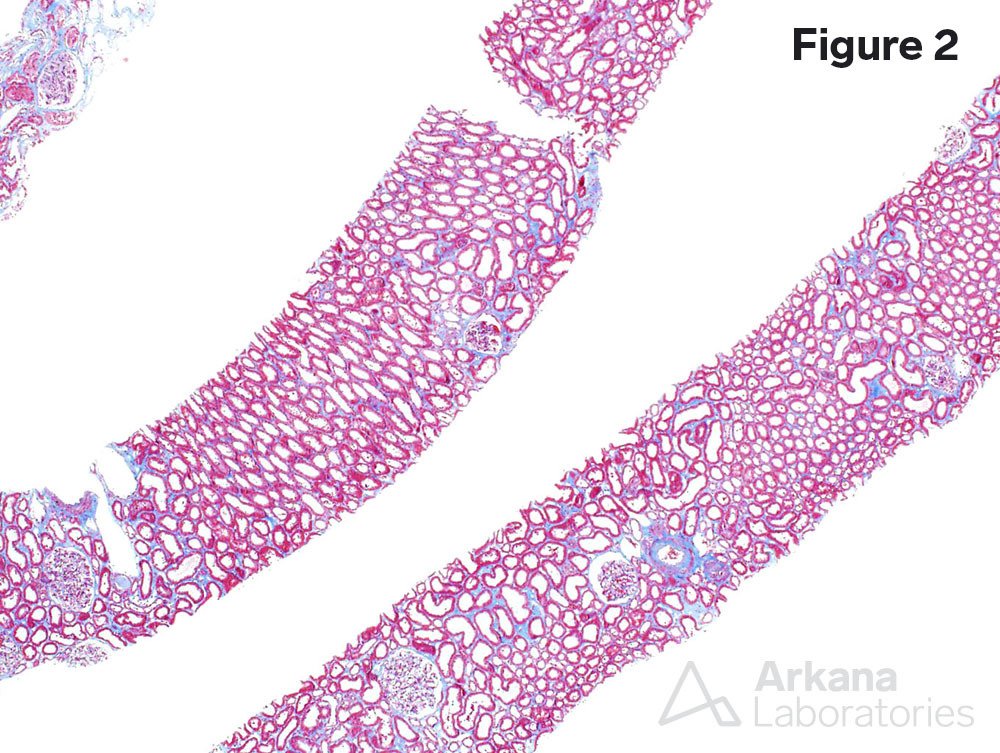
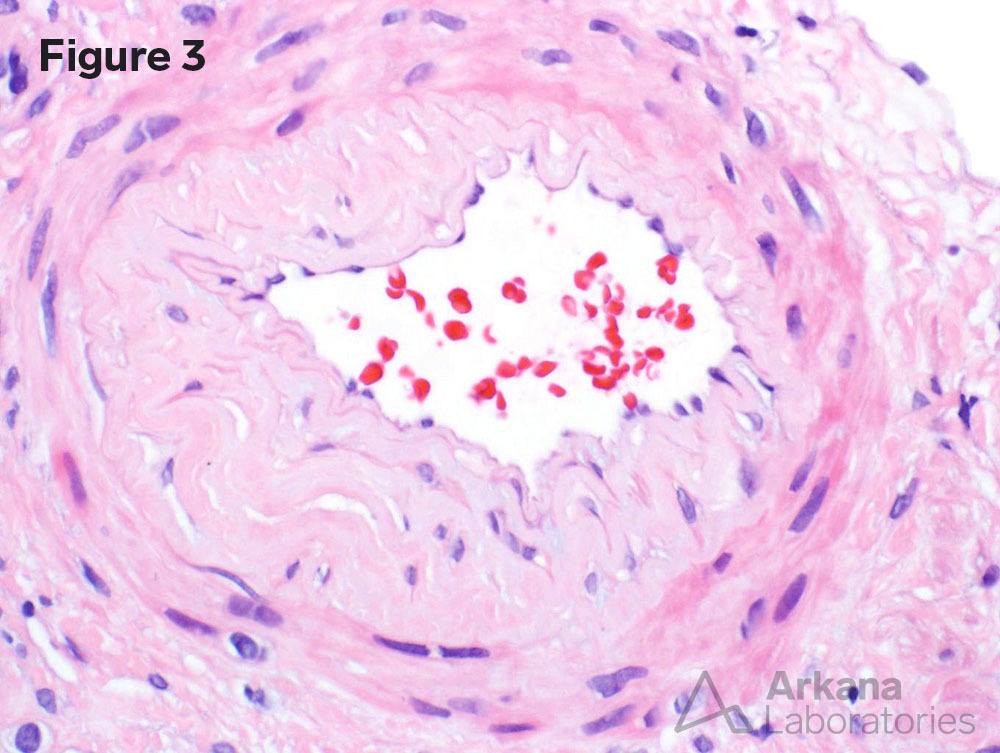
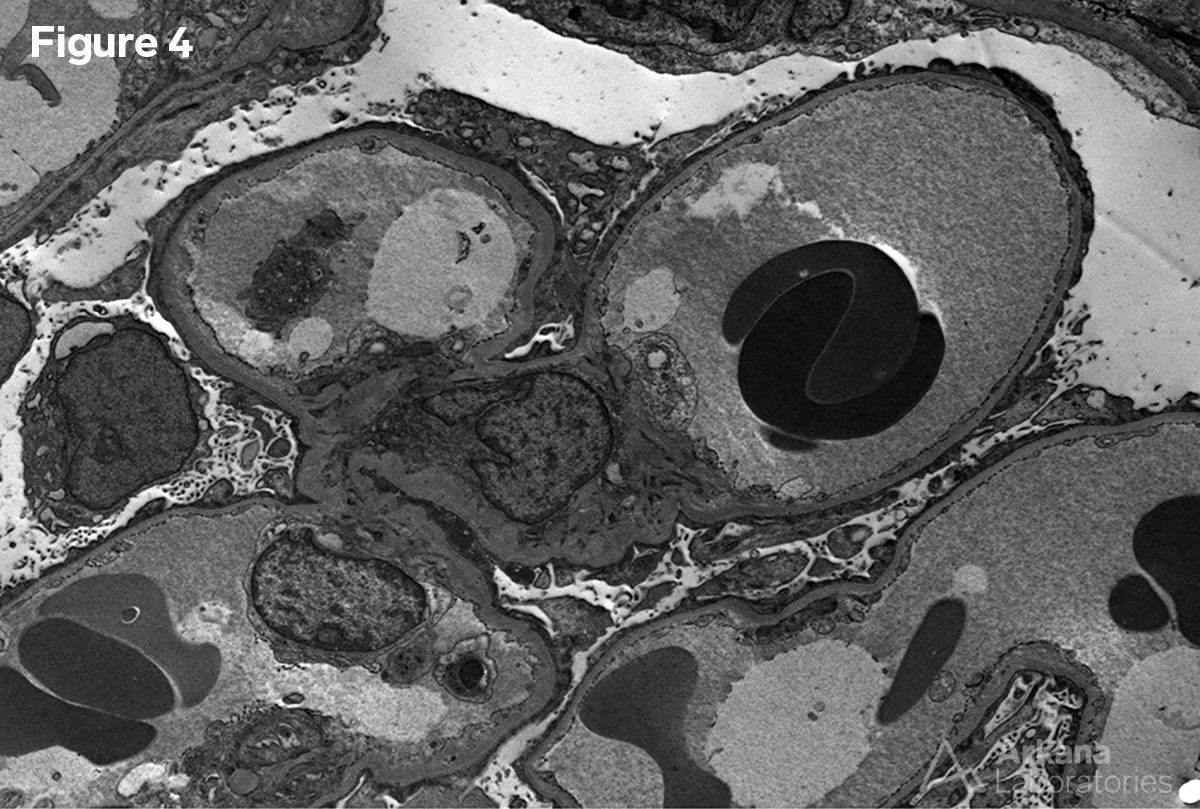
A 70-year-old female presents with nephrotic range proteinuria. She had been in her regular state of health until 2 weeks ago when she noticed swelling in her ankles and that her shoes no longer fit. She went to her family practitioner who sent her to a cardiologist to rule out congestive heart failure. Her troponin levels were normal and her creatinine on routine examination was 7.5 mg/dL. She was admitted to the hospital and an emergent kidney biopsy was requested. Figure 1 shows a normal glomerulus. Figure 2 shows no significant interstitial fibrosis. Figure 3 shows severe arteriosclerosis. Figure 4 shows complete podocyte foot process effacement.
A subset of minimal change disease occurs in older individuals and presents with nephrotic syndrome, edema, and acute renal failure. Most cases are idiopathic, but secondary etiologies must be considered. Secondary etiologies include malignancies (Hodgkin’s lymphoma, thymoma), drugs (NSAIDs, lithium), bee stings, and infections. It is presumed that arteriosclerosis plays a role by impairing compensatory response to hemodynamic stress and leads to acute renal failure in adults. T cell dysregulation and overexpression of certain interleukins are believed to be central in the pathogenesis of minimal change disease. Treatment involves immunosuppressive therapy and diuresis. Careful attention to patient’s volume status and supportive therapy for acute kidney injury is needed in adults. Albumin infusion may be considered if there is evidence of severe intravascular volume depletion and hypoalbuminemia. Over 80% of adults with minimal change disease respond to corticosteroid therapy. A minority of patients may develop irreversible renal failure.
J Am Soc Nephrol 24: 702–711, 2013
https://www.ncbi.nlm.nih.gov/pubmed/23431071
Quick note: This post is to be used for informational purposes only and does not constitute medical or health advice. Each person should consult their own doctor with respect to matters referenced. Arkana Laboratories assumes no liability for actions taken in reliance upon the information contained herein.