A 70-year-old man undergoes kidney biopsy because of worsening renal function. His medical history is otherwise significant for hyperlipidemia, type II diabetes mellitus, hypertension, gout, coronary artery disease, s/p CABG 10 years ago and congestive heart failure. Serum creatinine is 6 mg/dl. Serological studies are negative. Urinalysis shows proteinuria of up to 1.5 g/day.
What is the most potentially correctable factor contributing to his worsening of renal function?
a. Diabetic glomerulosclerosis
b. Atheroembolism
c. Uric acid nephropathy
d. Hypertensive arteriosclerosis
e. Interstitial nephritis
The answer is B. Atheroembolism.
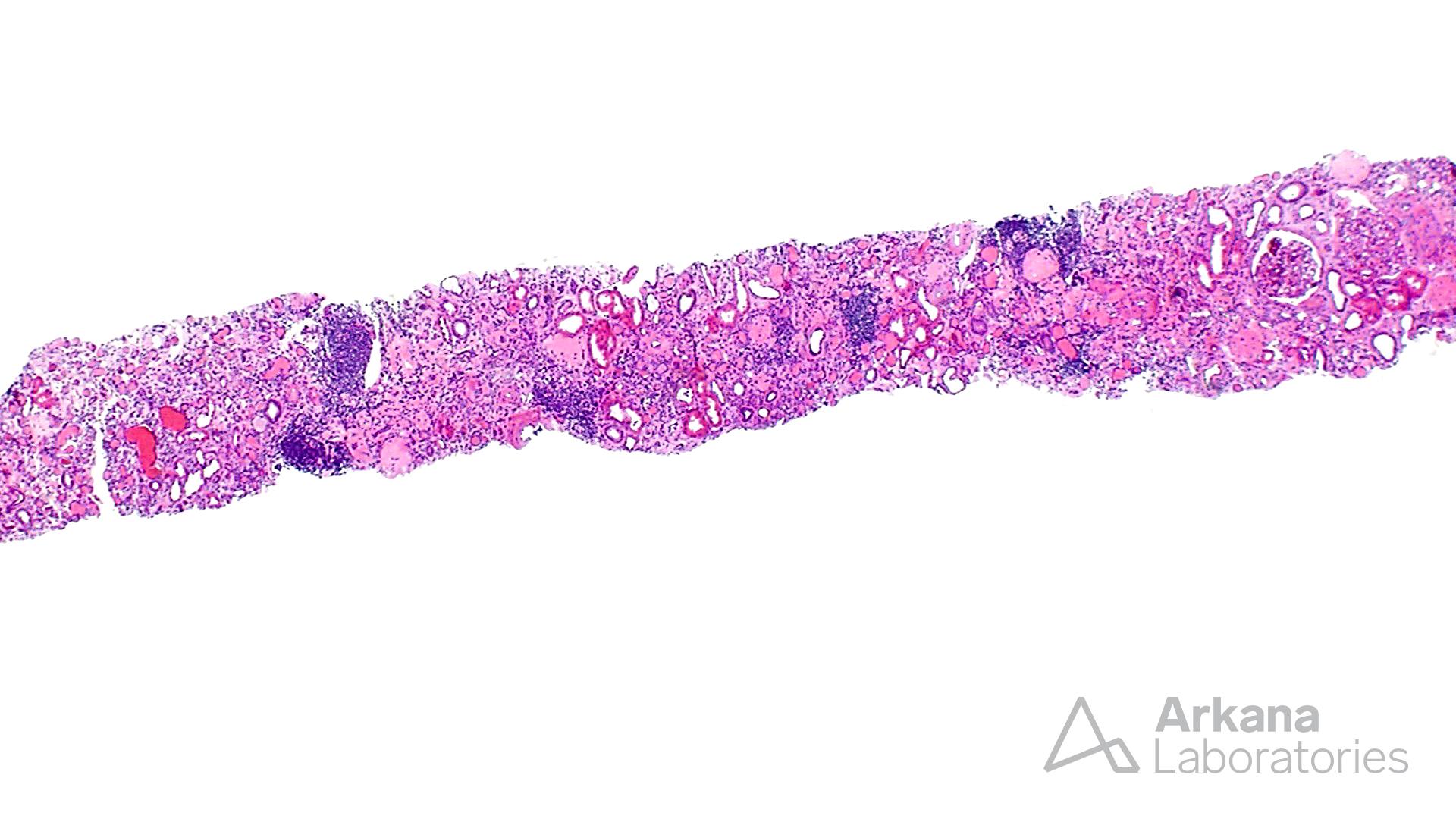
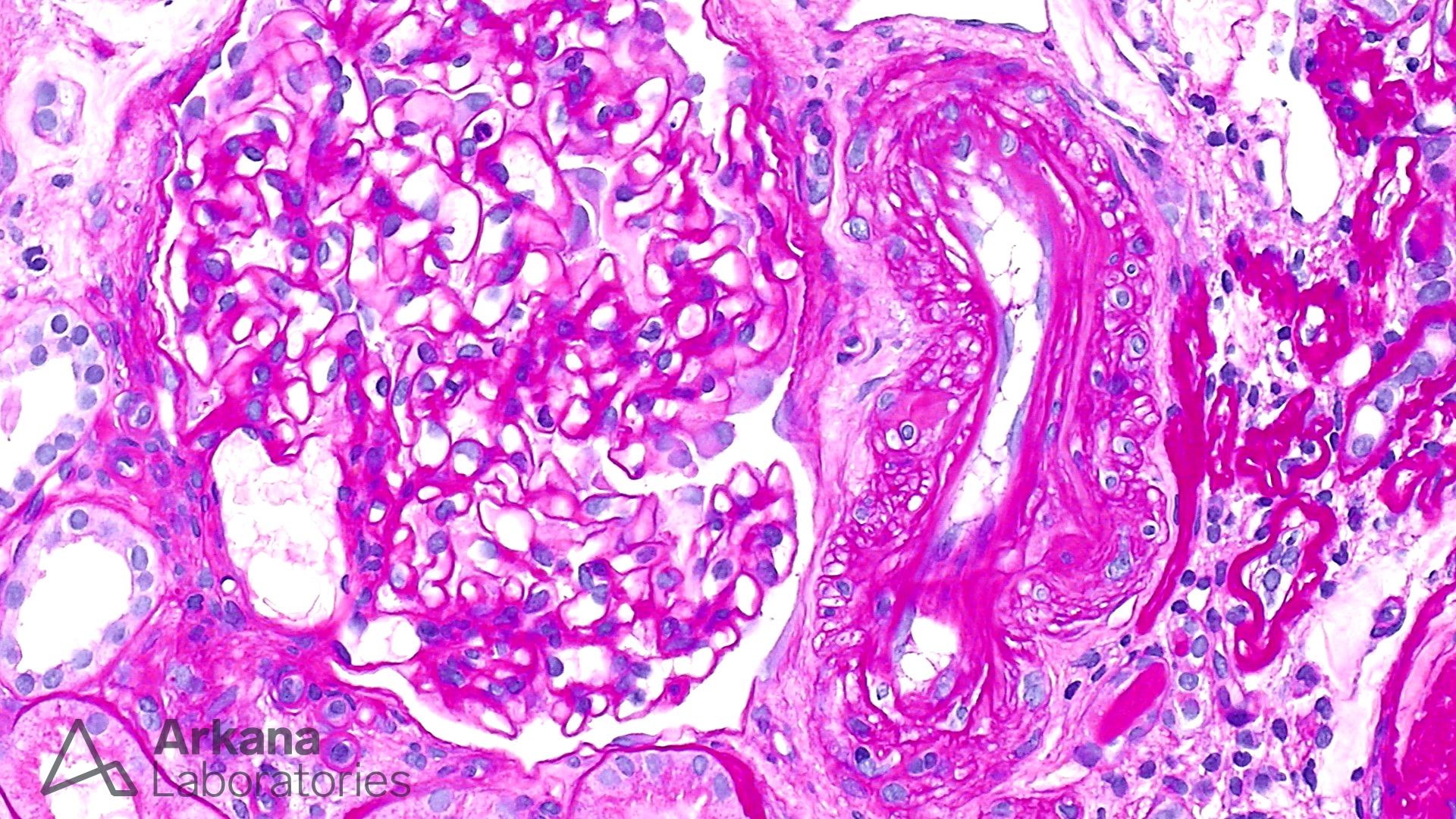
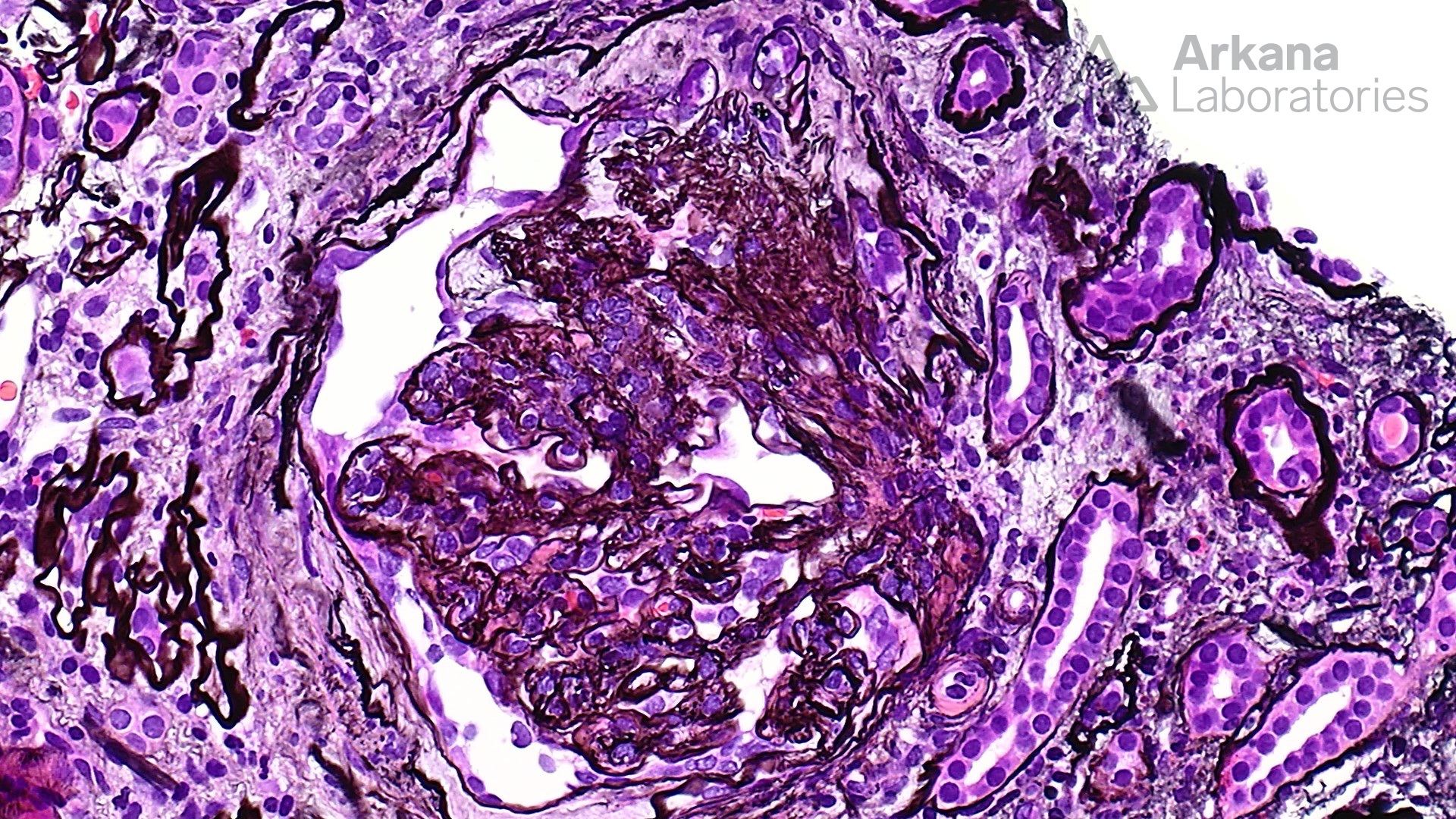
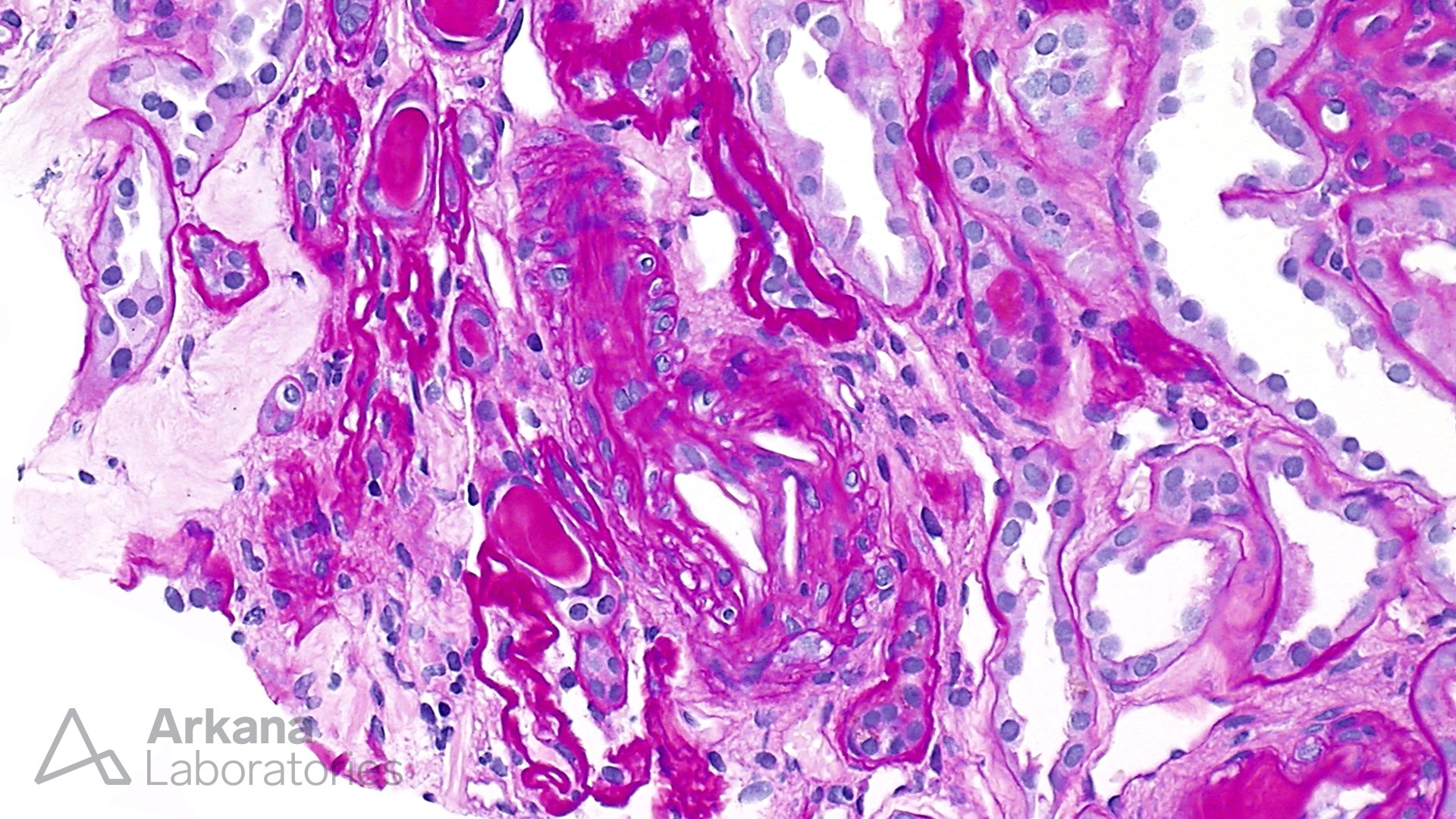
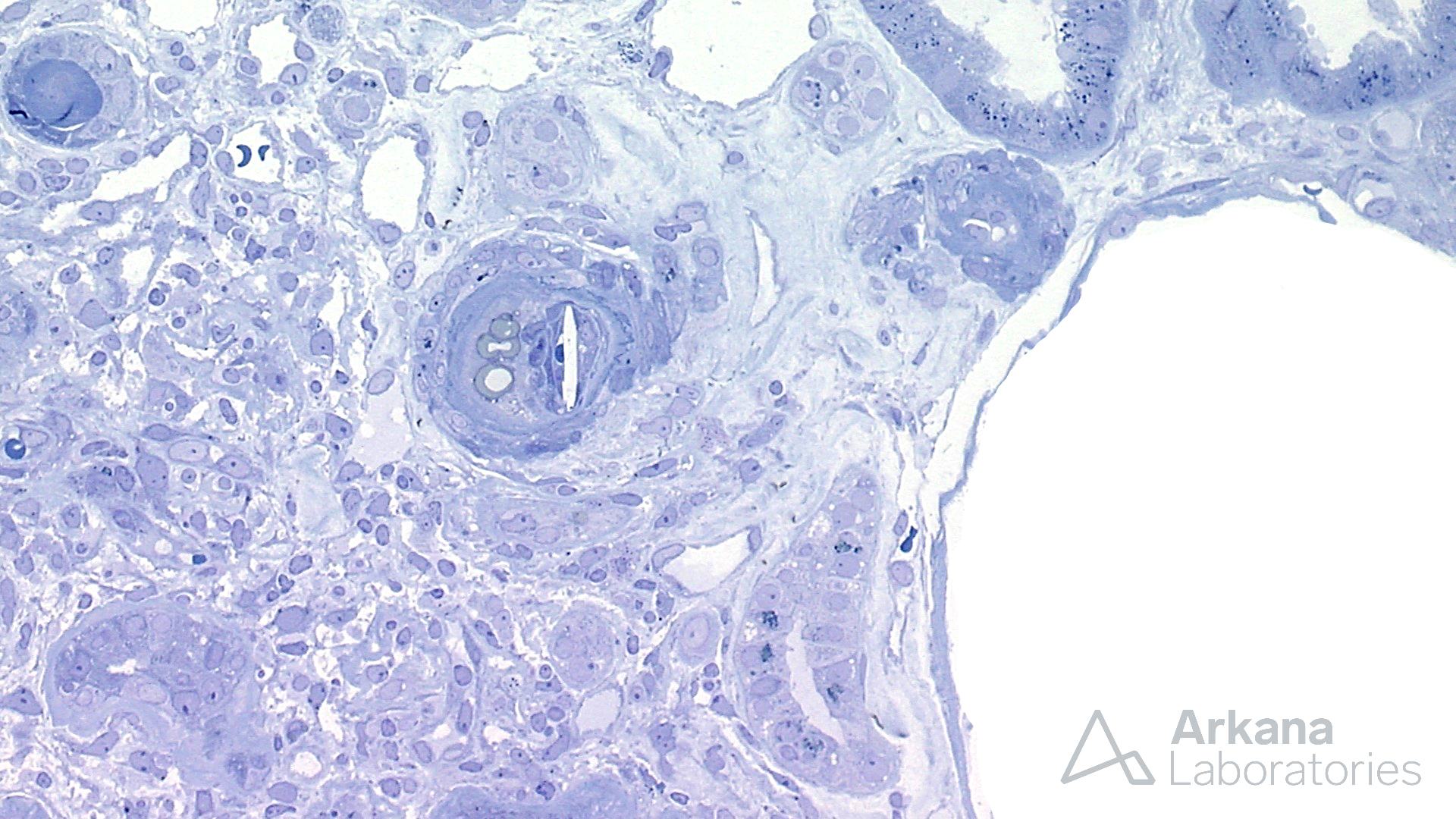
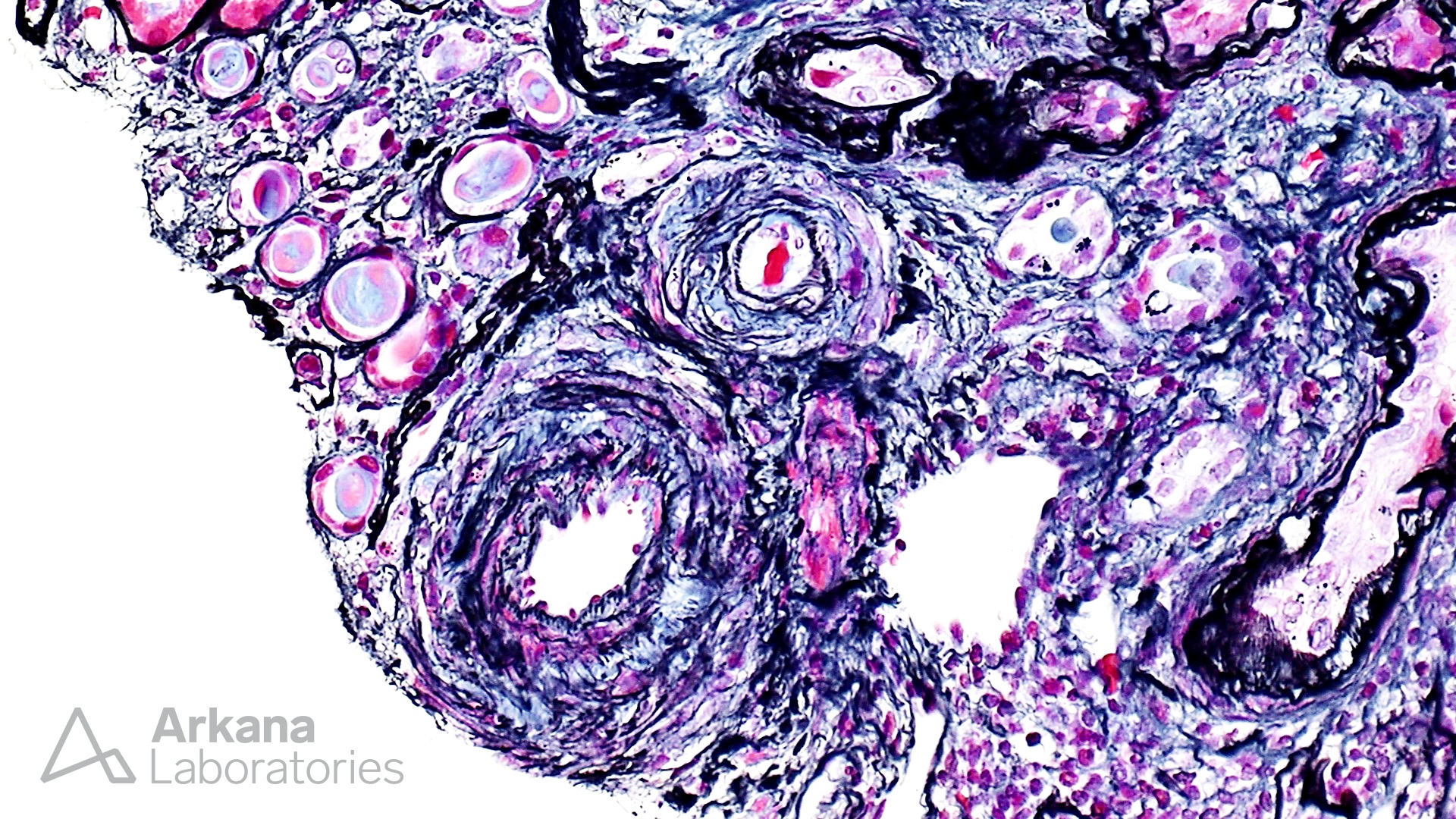
At low magnification, this biopsy shows features of advanced interstitial fibrosis and tubular atrophy. Despite the history of long standing diabetes mellitus, the glomeruli do not show features of nodular glomerulosclerosis. However, ischemic changes and segmental sclerosis is notable in the glomeruli. Several small arterioles contain needle shaped clefts, consistent with cholesterol emboli. These clefts represent residual empty spaces in the tissue created due to the dissolution of cholesterol by alcohol during tissue processing. Most cases of atheroembolism are iatrogenic, usually following shortly after an invasive vascular procedure, cardiopulmonary resuscitation, trauma, and anticoagulant or thrombolytic therapy; however, ~25% can be spontaneous. This patient did not have any recent history of invasive procedures, and apparently, the atheroembolism was spontaneous. This requires further urgent clinical and radiological evaluation. Uric acid crystals are usually medullary and interstitial and have a radiating appearance with giant cell reaction, in contrast to cholesterol emboli which are often intravascular. The patient also had arteriosclerosis and microangiopathic changes secondary to hypertension, however, atheroembolism is likely a more readily correctible cause of renal injury in this scenario.
Quick note: This post is to be used for informational purposes only and does not constitute medical or health advice. Each person should consult their own doctor with respect to matters referenced. Arkana Laboratories assumes no liability for actions taken in reliance upon the information contained herein.