The patient is a 32-year-old African American female who presents with hypertensive urgency, positive ANA, positive anti-RNA polymerase III antibody, schistocytes on the peripheral smear, forgetfulness, and a creatinine of 2. On physical examination, the skin is tight and thickened along the face (“masked face”), back, and proximal arms. Urinalysis shows 250 mg of proteinuria and no active urine sediment. Serologies for c-ANCA, p-ANCA, dsDNA, and anti-GBM are negative.
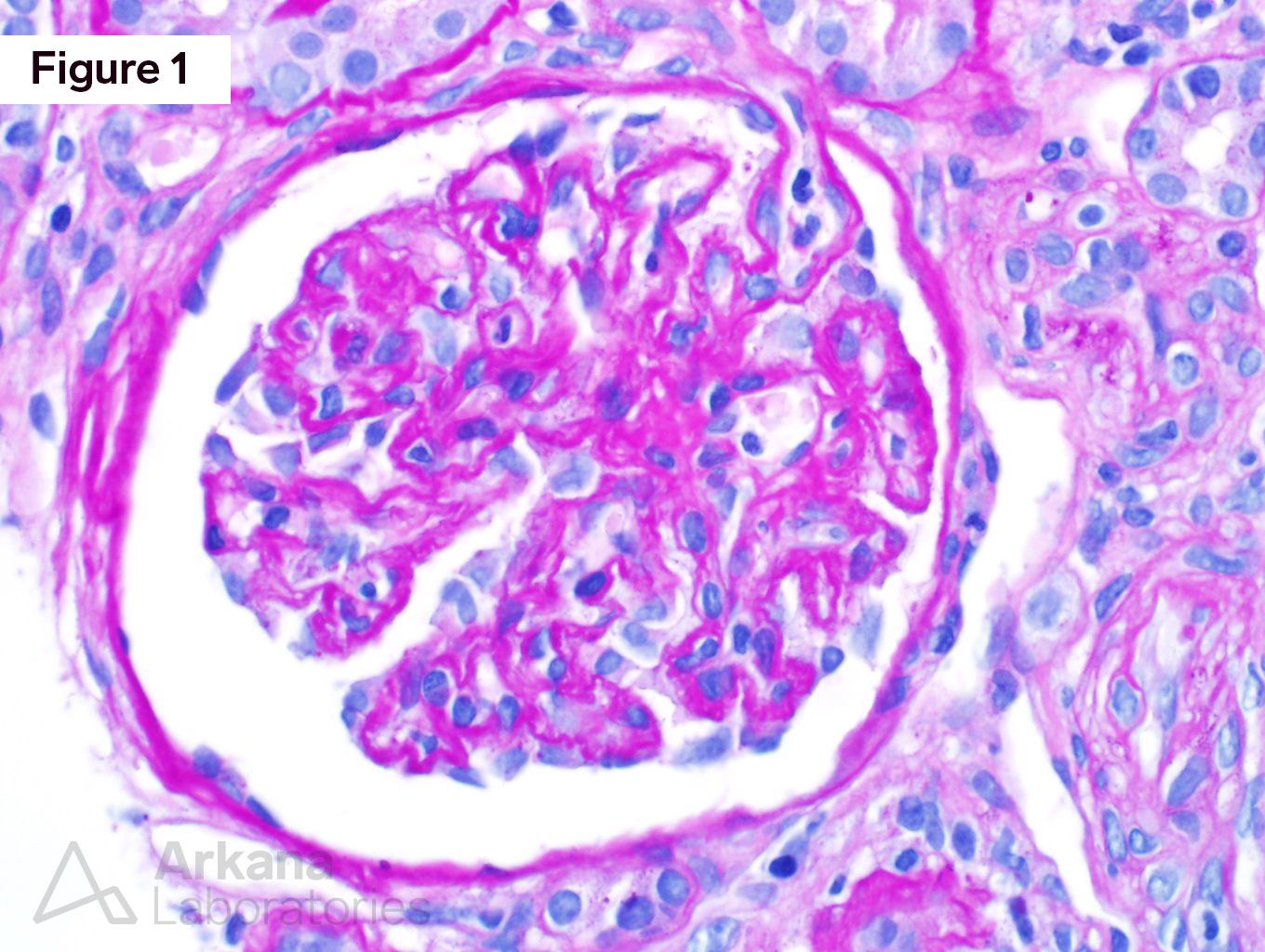
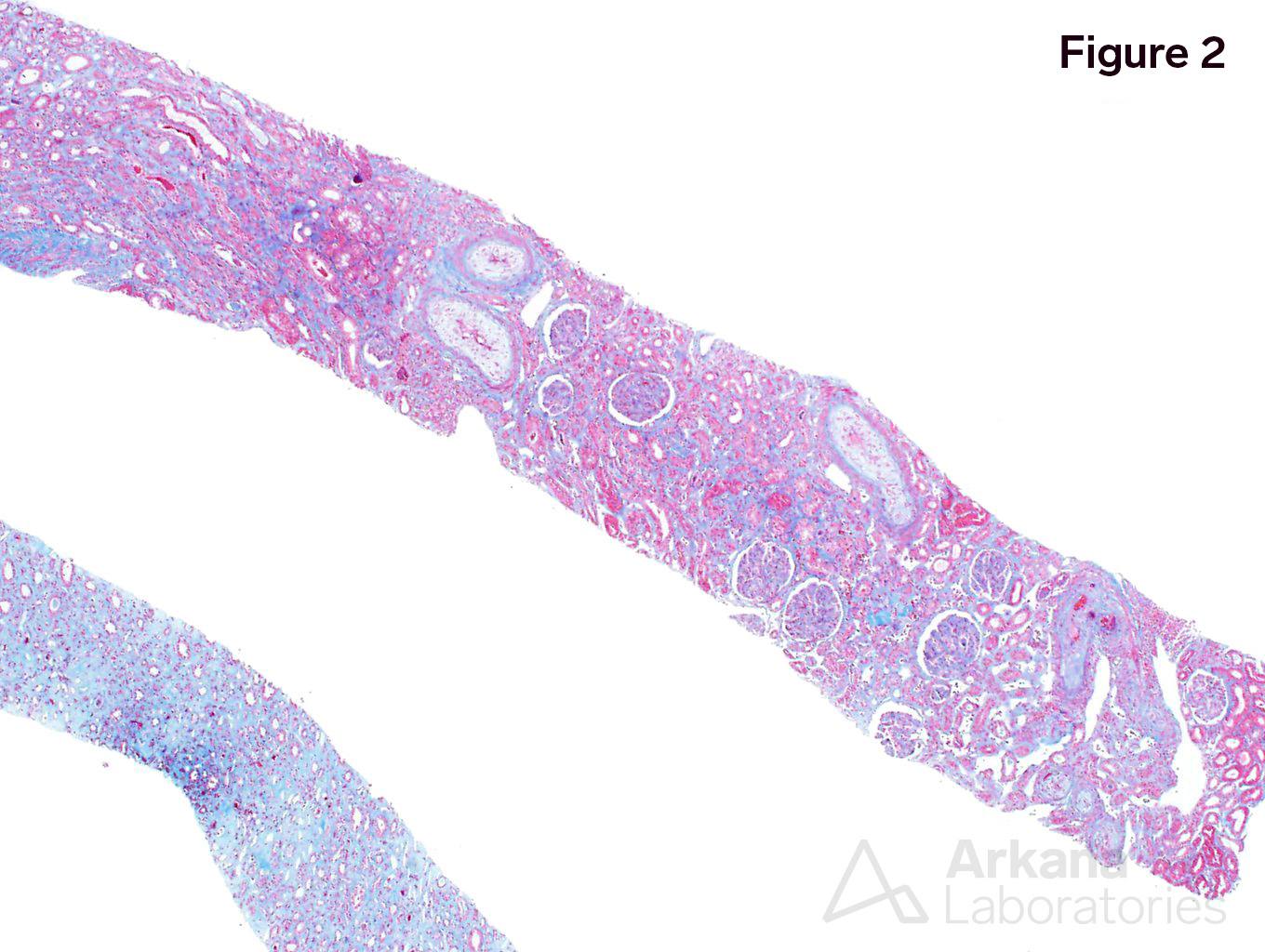
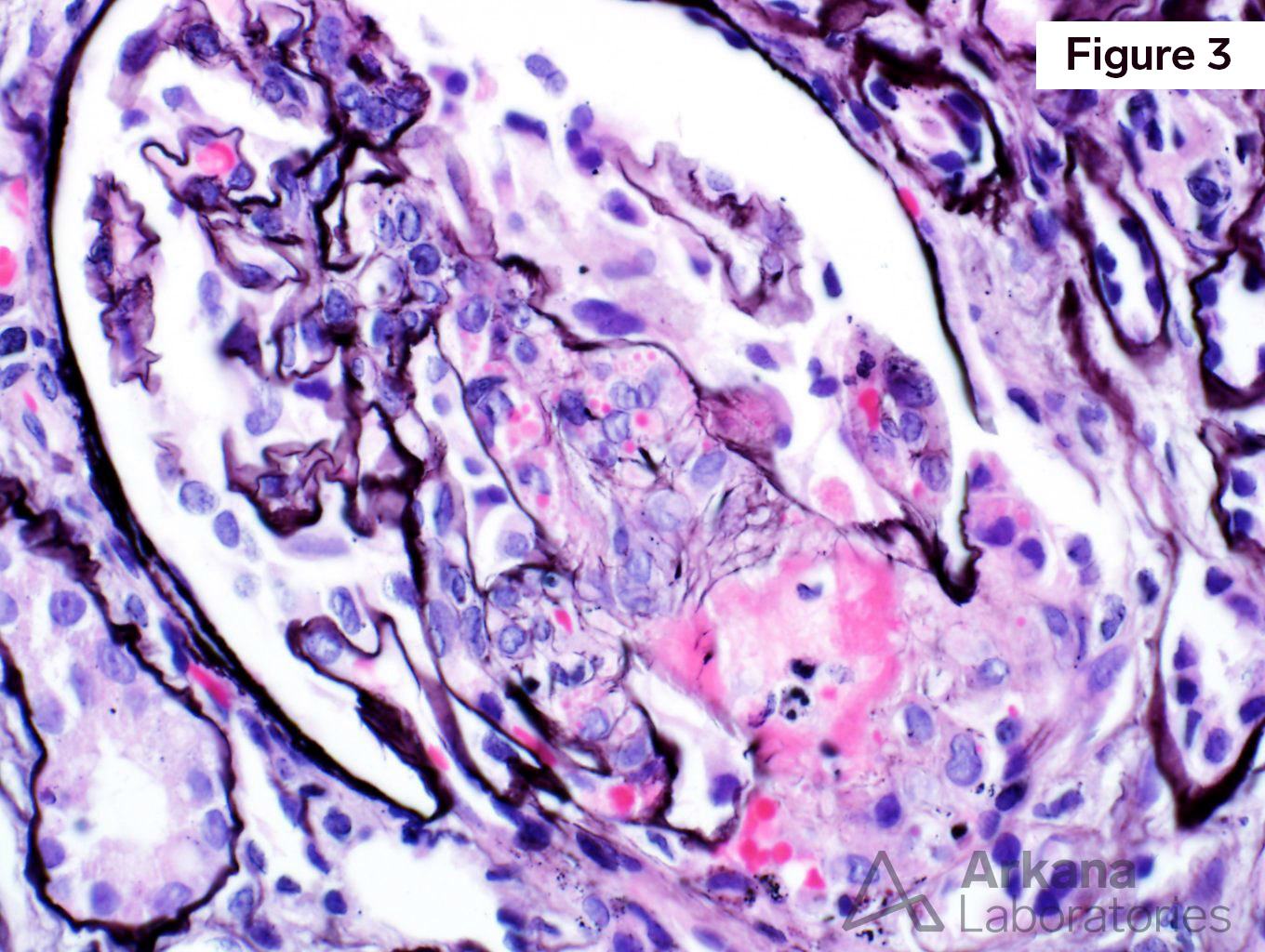
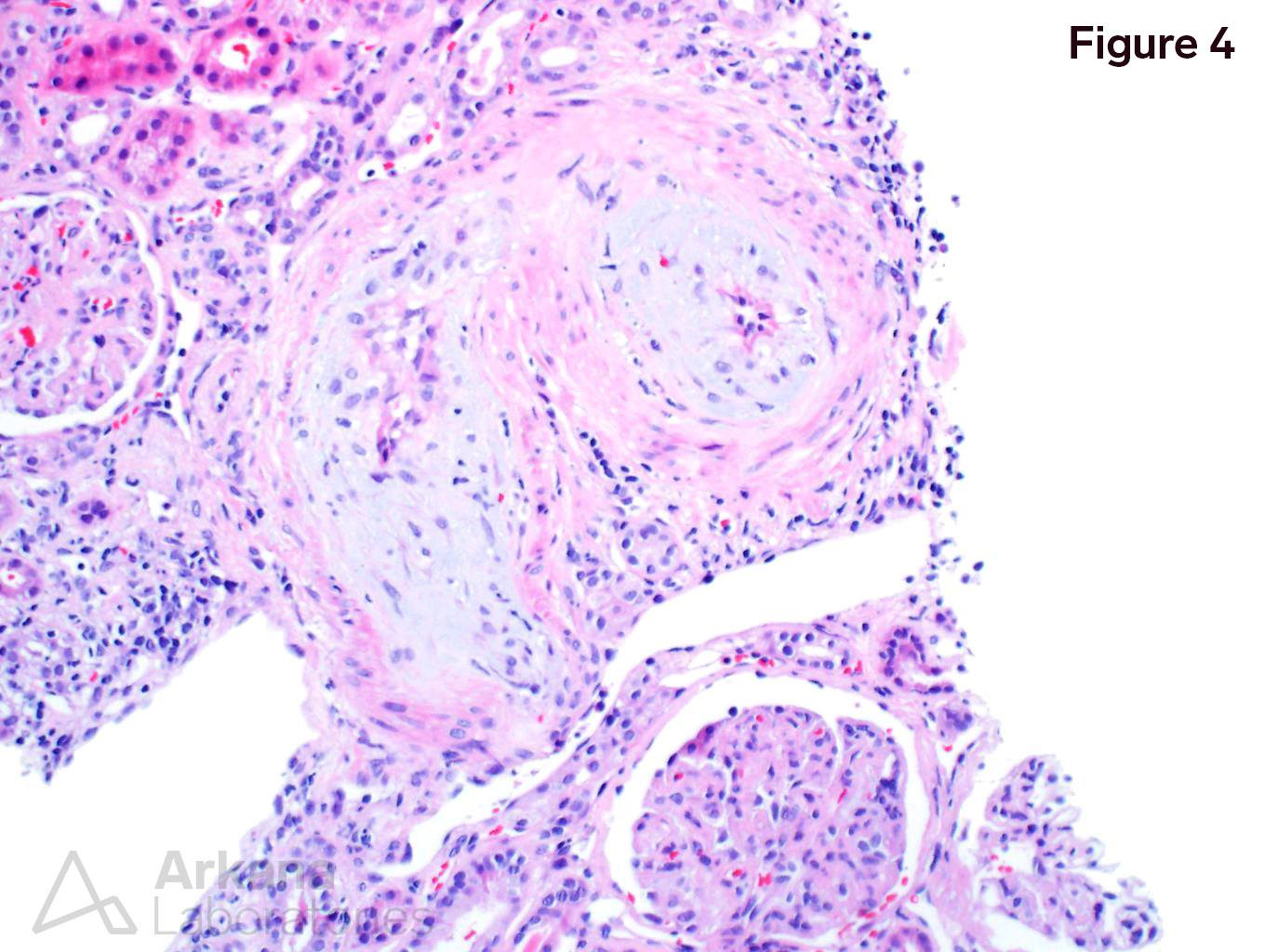
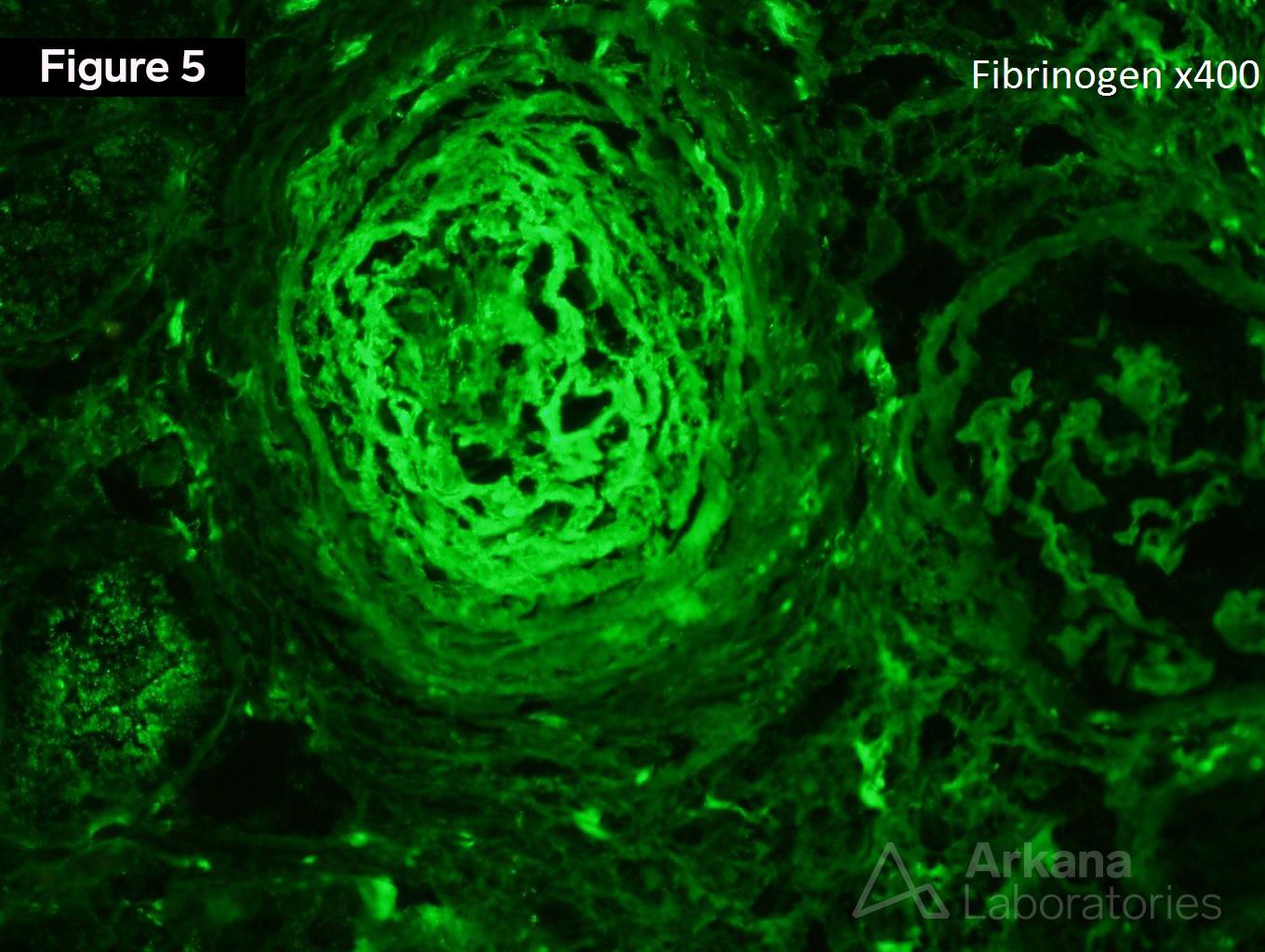
The patient has scleroderma renal crisis. Figure 1 shows an ischemic glomerulus. Figure 2 shows moderate interstitial fibrosis. From low power, the intimal edema and intimal proliferation within the arteries is prominent. Figure 3 shows a mesangiolysis and schistocytes within a glomerulus. Figure 4 shows intimal edema and almost complete occlusion the artery. Figure 5 shows fibrinogen deposition within an artery.
Scleroderma is commonly divided into a limited and systemic form. Limited scleroderma consists of Raynaud’s phenomenon, sclerosis of the skin, fingers, and face. Anticentromere antibodies occur in 50 to 90% of patients in limited cutaneous scleroderma. Diffuse scleroderma produces fibrosis of the skin of the extremities, face, and trunk. Patients with diffuse cutaneous scleroderma are more likely to develop visceral involvement including esophageal sclerosis, pulmonary fibrosis, myocardial fibrosis, and scleroderma renal crisis. Esophageal sclerosis is the most common visceral complication and lung involvement is the leading cause of death.
Scleroderma renal crisis occurs in less than 5% in patients with systemic sclerosis and less than 2% in those with limited cutaneous forms of the disease. Scleroderma renal crisis affects the intra-lobular and arcuate arteries of the kidneys with intimal proliferation leading to narrowing of the vessel lumen and to reduced blood flow. Scleroderma renal crisis has a poor prognosis with 55% patients progressing to ESRD.
Quick note: This post is to be used for informational purposes only and does not constitute medical or health advice. Each person should consult their own doctor with respect to matters referenced. Arkana Laboratories assumes no liability for actions taken in reliance upon the information contained herein.