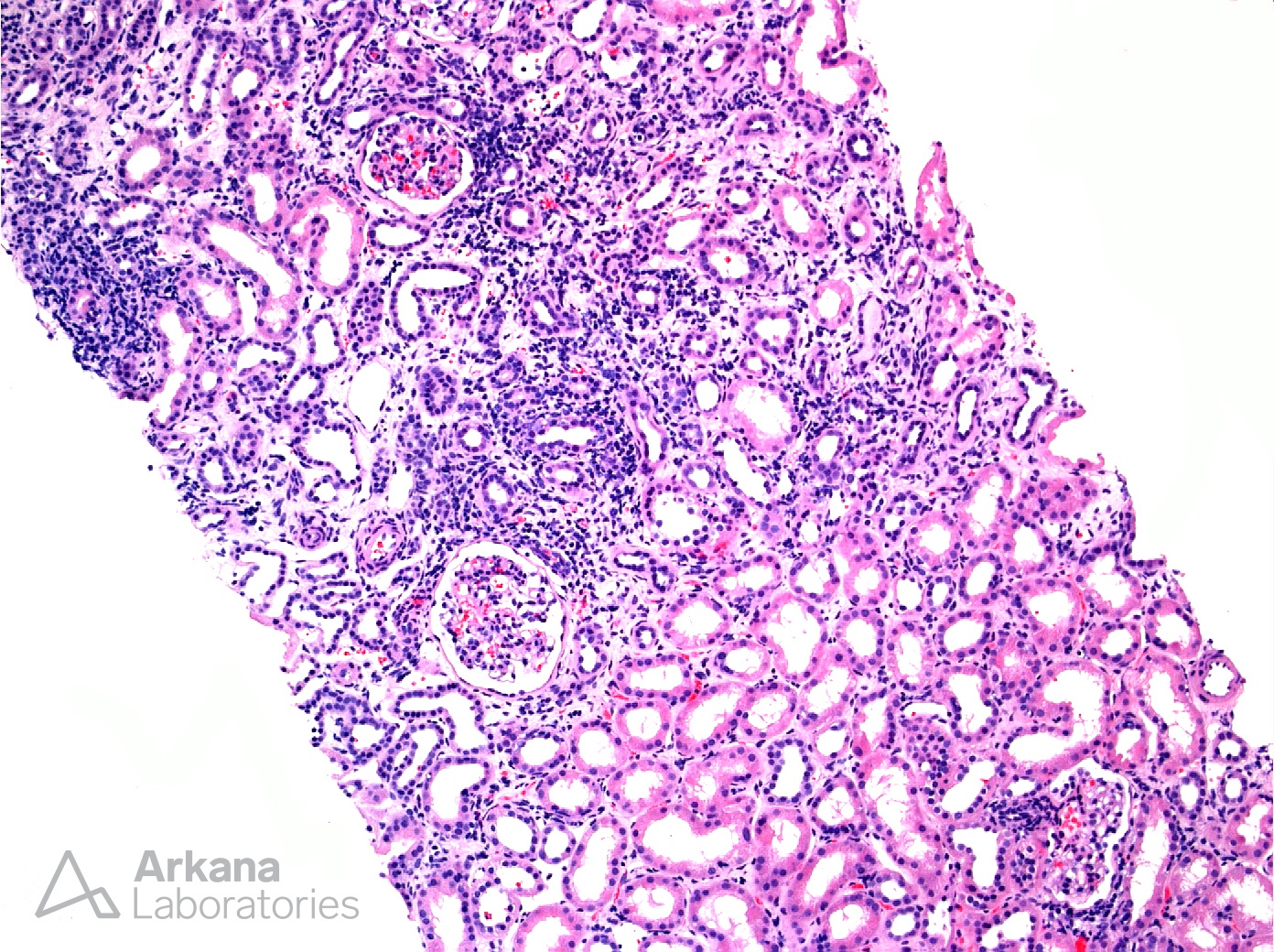
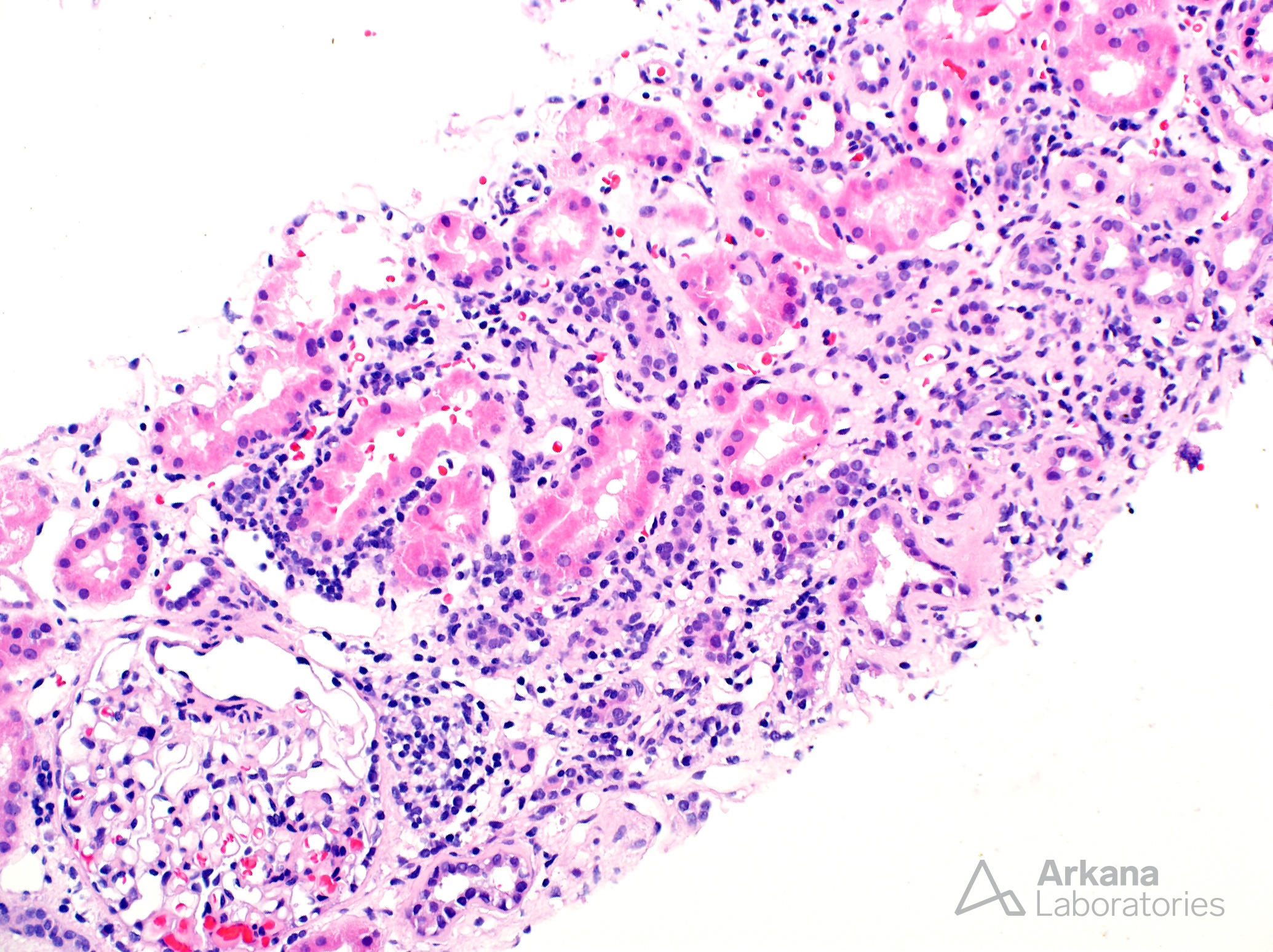
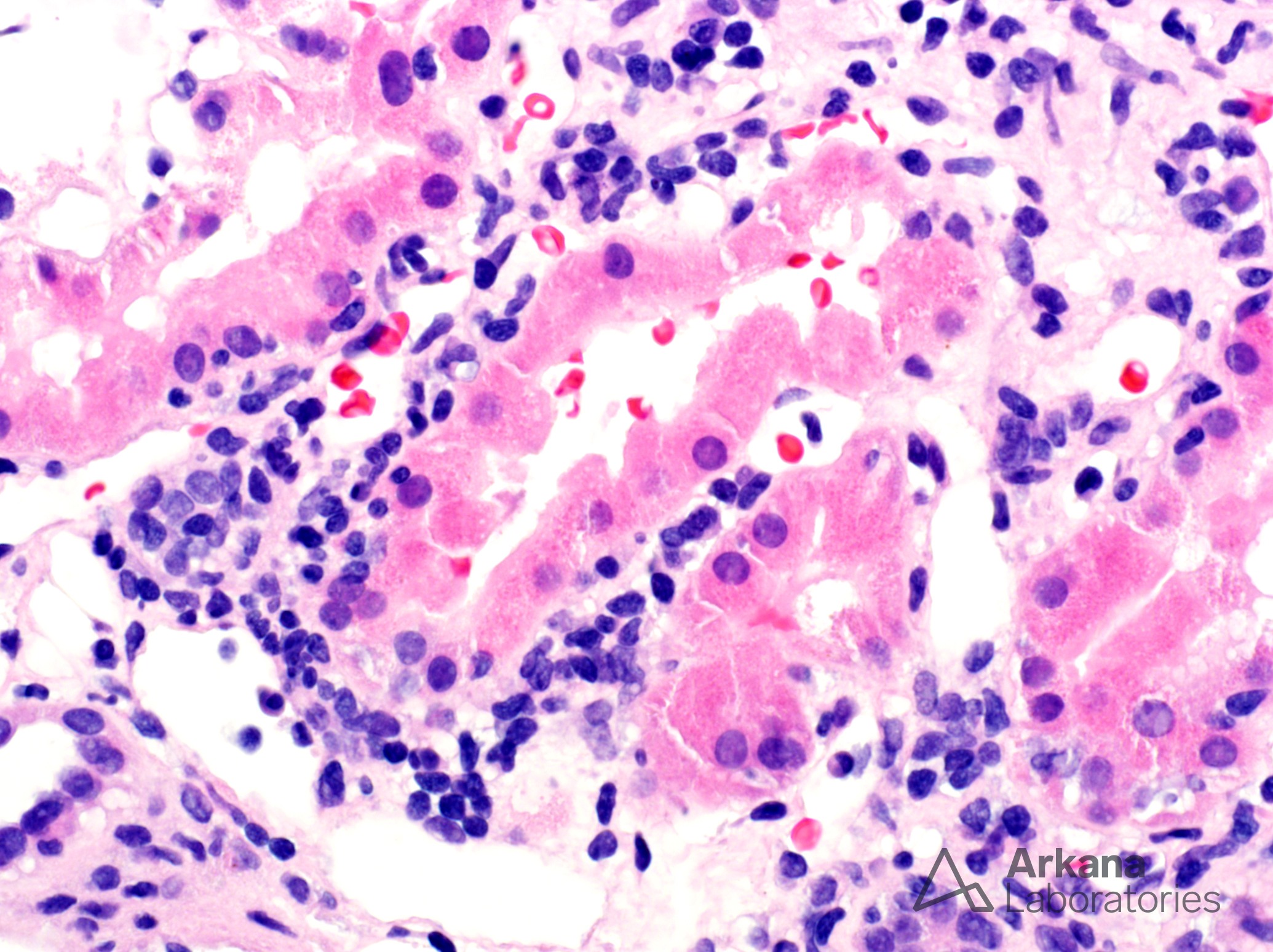
Tubulointerstitial nephritis with uveitis (TINU) was first described as a distinct entity by Dobrin, et al. in 1975. TINU primarily affects young females (median age 15 years) who commonly have associated systemic signs and symptoms of the disease including weight loss, fever, fatigue, malaise, abdominal or flank pain, arthralgias or myalgias, and headache. The syndrome is likely underdiagnosed as a result of the asynchronous presentation of the renal and ocular symptoms. In fact, the ocular symptoms lag behind the interstitial nephritis diagnosis in two-thirds of cases by up to 14 months. TINU should be considered a diagnosis of exclusion only after other etiologies of uveitis have been excluded such as Sjögren syndrome, sarcoidosis, syphilis, SLE, Behçet disease, IgG4-related disease, toxoplasmosis, and ANCA-associated disease. The renal biopsy findings of TINU are relatively nonspecific, consisting of interstitial inflammation and tubulitis. The interstitial inflammatory cells are predominantly lymphocytes in most cases (as shown in the photomicrographs here). However, the infiltrate is reported to include eosinophils in one-third of cases, neutrophils are in 25% of biopsies, and noncaseating granulomas in approximately 10% of renal biopsy specimens. The tubulitis is often most severe in proximal tubules which, as shown here, can also display lymphocyte cuffing. Immunofluorescence studies are negative throughout the tissue including the tubular basement membranes.
References:
Dobrin RS, Vernier RL, Fish AJ. Acute eosinophilic interstitial nephritis and renal failure with bone marrow-lymph node granulomas and anterior uveitis. Am J Med 1975; 59: 325-333
Mandeville JTH, Levinson RD, Holland GN. The Tubulointerstitial nephritis and uveitis syndrome. Survey of ophthalmology 2001; 46: 195-208
Herlitz LC, Chun MJ, Stokes MB, et al. Uveitis and acute renal failure. Kidney Int 2007; 72: 1554-1557
Quick note: This post is to be used for informational purposes only and does not constitute medical or health advice. Each person should consult their own doctor with respect to matters referenced. Arkana Laboratories assumes no liability for actions taken in reliance upon the information contained herein.