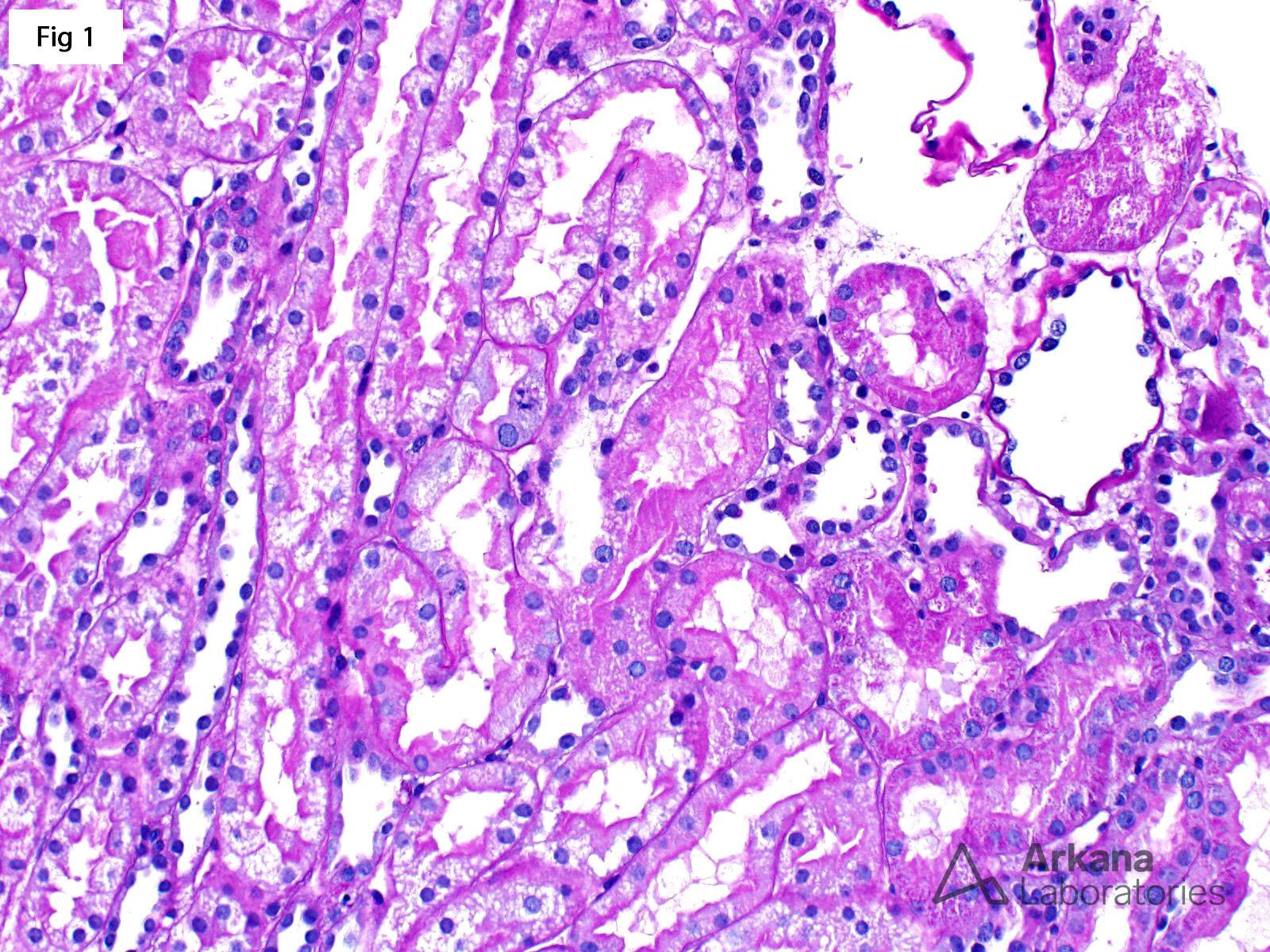
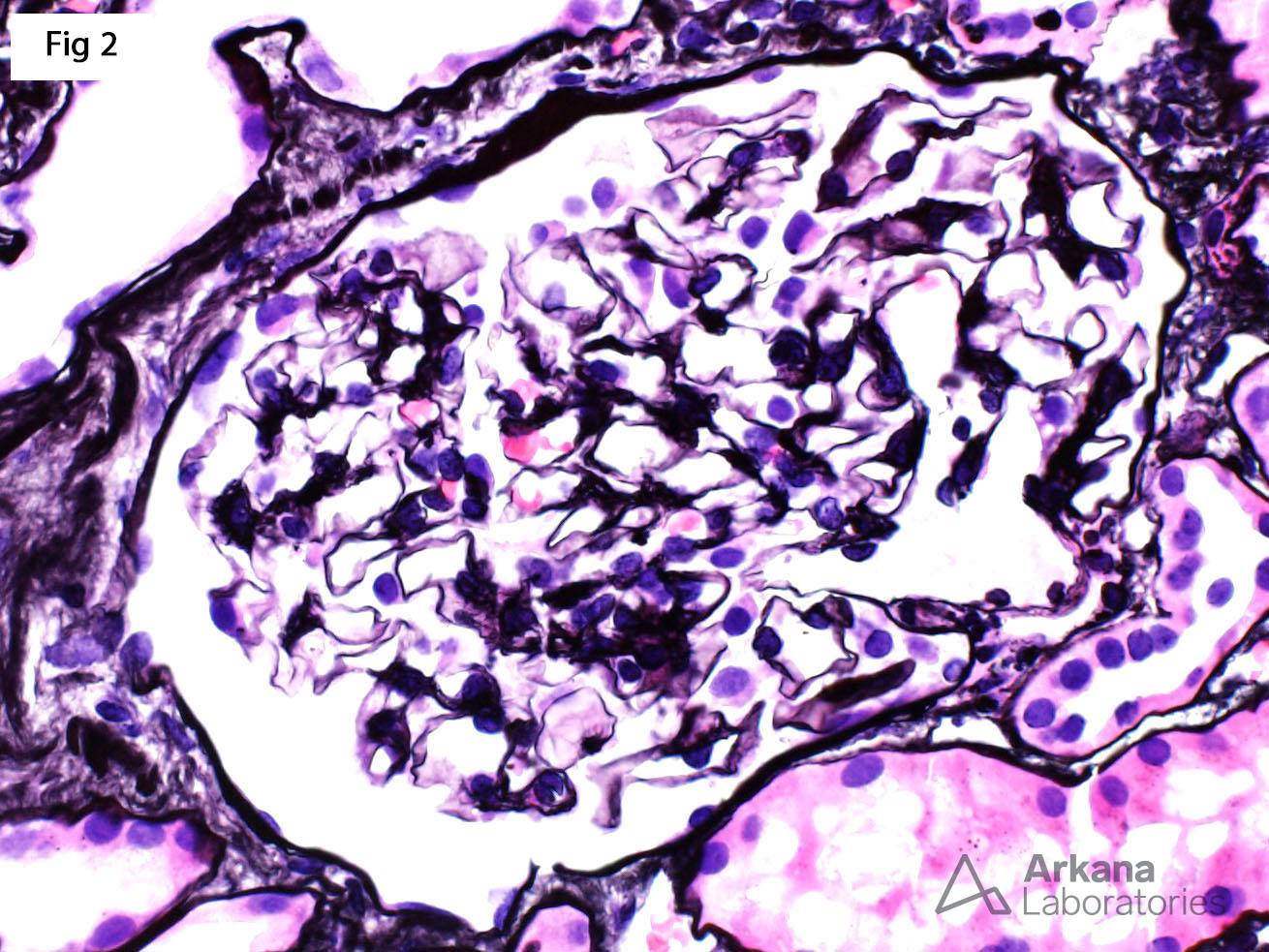
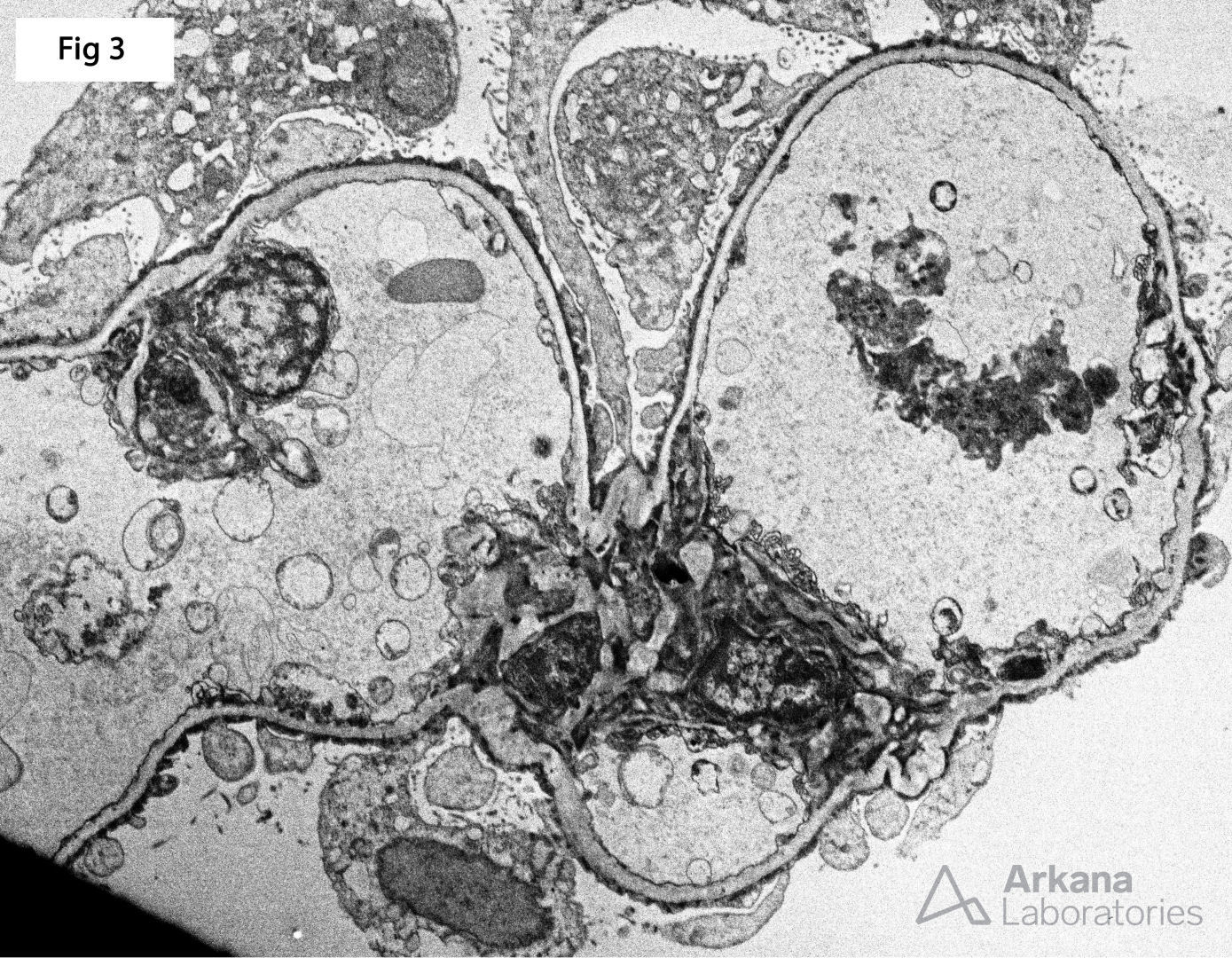
This 81-year-old male with past medical history of hypertension and coronary artery disease presents with acute kidney injury (Cr = 4.6 mg/dl). A renal biopsy was performed and shows acute tubular injury characterized by markedly vacuolated and reactive tubular epithelium with loss of the proximal tubular brush border (Fig 1). The glomeruli are completely unremarkable by light microscopy (Fig 2) and there is no evidence of immune complex deposition by immunofluorescence. However, electron microscopy shows diffuse epithelial foot process effacement with microvillous transformation (Fig 3). The morphologic findings are consistent with minimal change disease. After further review of the medical chart and laboratory data, it was noticed that the patient did have 3+ protein on a urinalysis performed during his initial presentation. Subsequently, 24 hr. urine protein was measured and was found to be in nephrotic range (5.1 gm). While the great majority of patients with minimal change disease present with nephrotic syndrome, there is a subset of patients who may also present with a concomitant acute kidney injury. A recent case series describing the clinical course of minimal change disease with onset in adulthood or late adolescence (see reference), showed that acute kidney injury may be observed in up to 40% of patients, and recovery of kidney function is achieved in essentially all of them. For his reason, in a patient with unexplained acute kidney injury, especially older adults, ruling out a podocytopathy as the cause of the renal failure is of utmost importance.
Reference: Maas RJ, et al. The clinical course of minimal change nephrotic syndrome with onset in adulthood or late adolescence: a case series. Am J Kidney Dis. 2017; 69: 637-646.
Quick note: This post is to be used for informational purposes only and does not constitute medical or health advice. Each person should consult their own doctor with respect to matters referenced. Arkana Laboratories assumes no liability for actions taken in reliance upon the information contained herein.