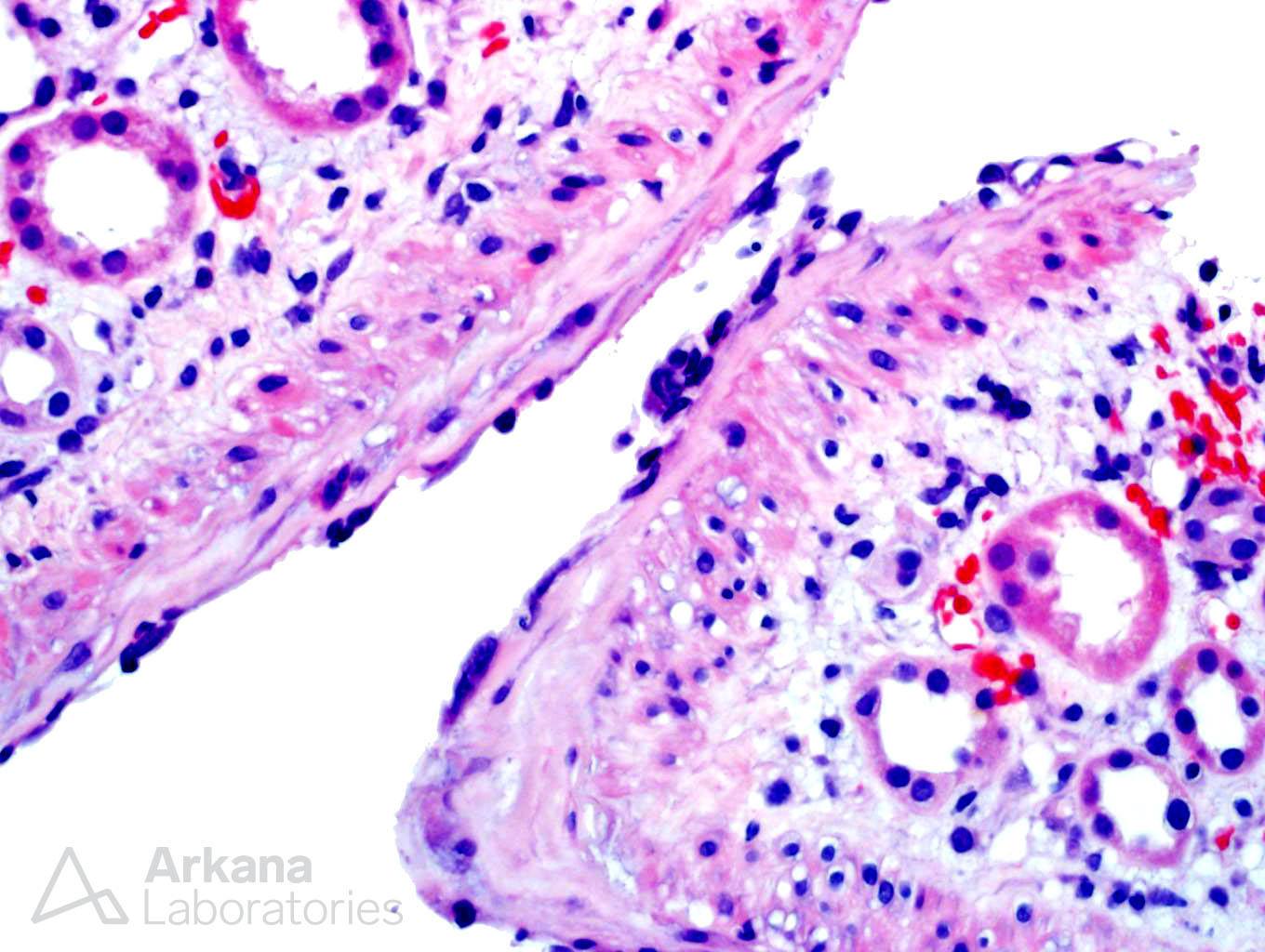
The patient is a 50-year-old African-American female with a past medical history significant for ESRD secondary to lupus nephritis who presents two weeks after a renal transplant with a delay in graft function. Her creatinine at the time of presentation is 9. She reports feeling fine and does not have any rashes or joint discomfort. A renal biopsy is performed on the transplanted kidney.
Which is the best diagnosis?
A. Acute Tubular Injury
B. Thrombotic thrombocytopenic purpura
C. Acute Antibody-Mediated Rejection
D. Vasculitis
The correct answer is c (acute antibody-mediated rejection).
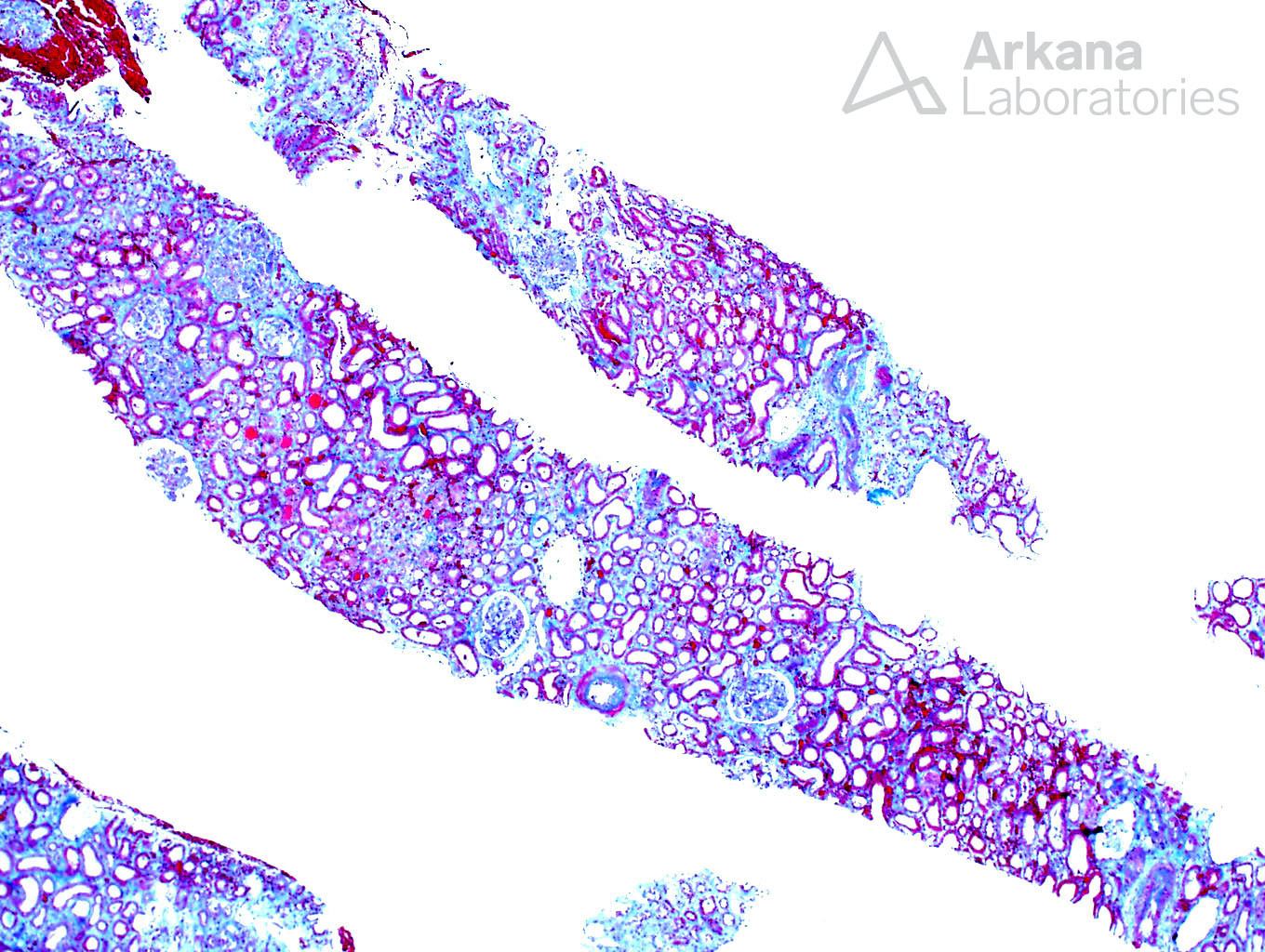
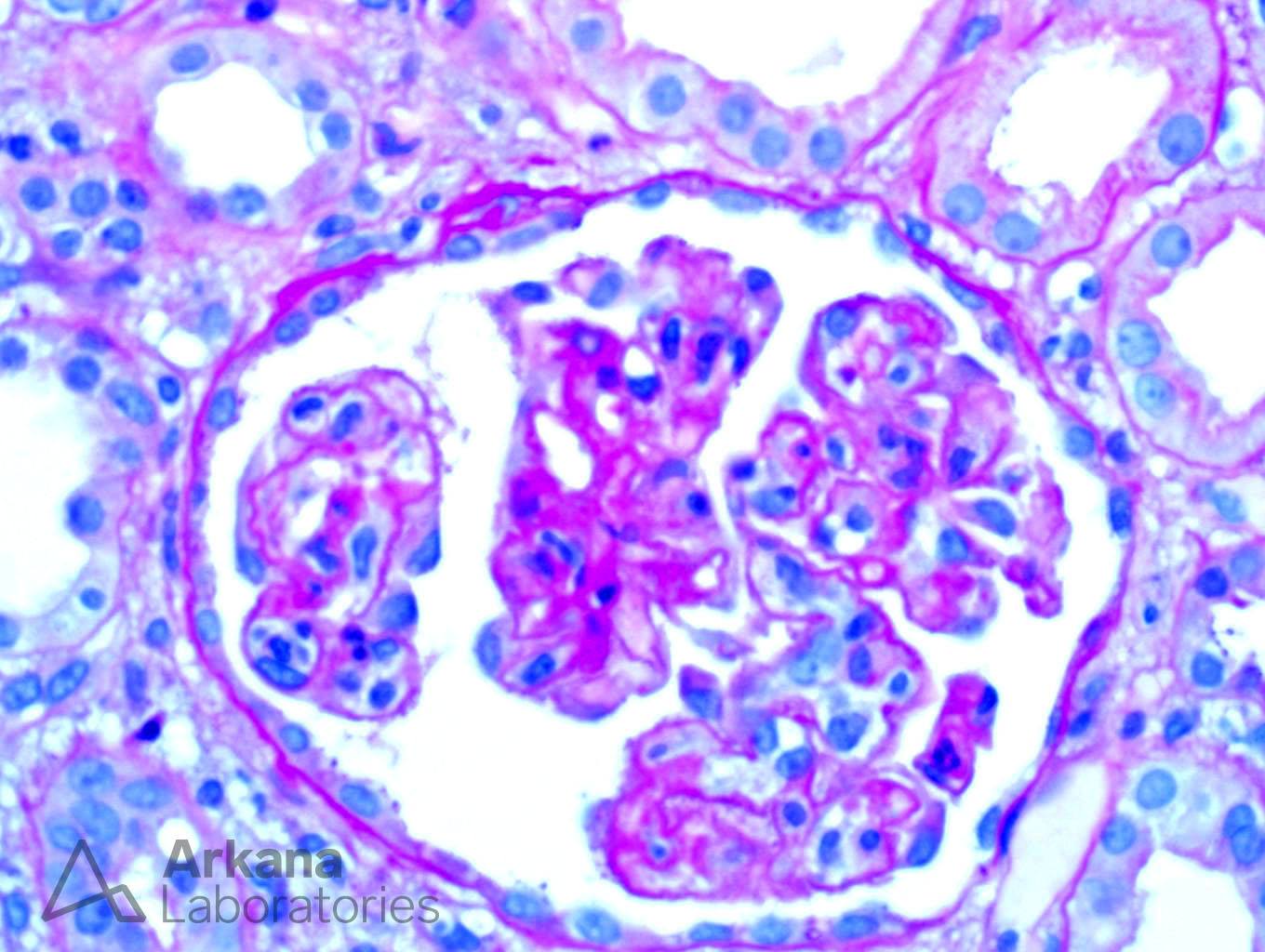
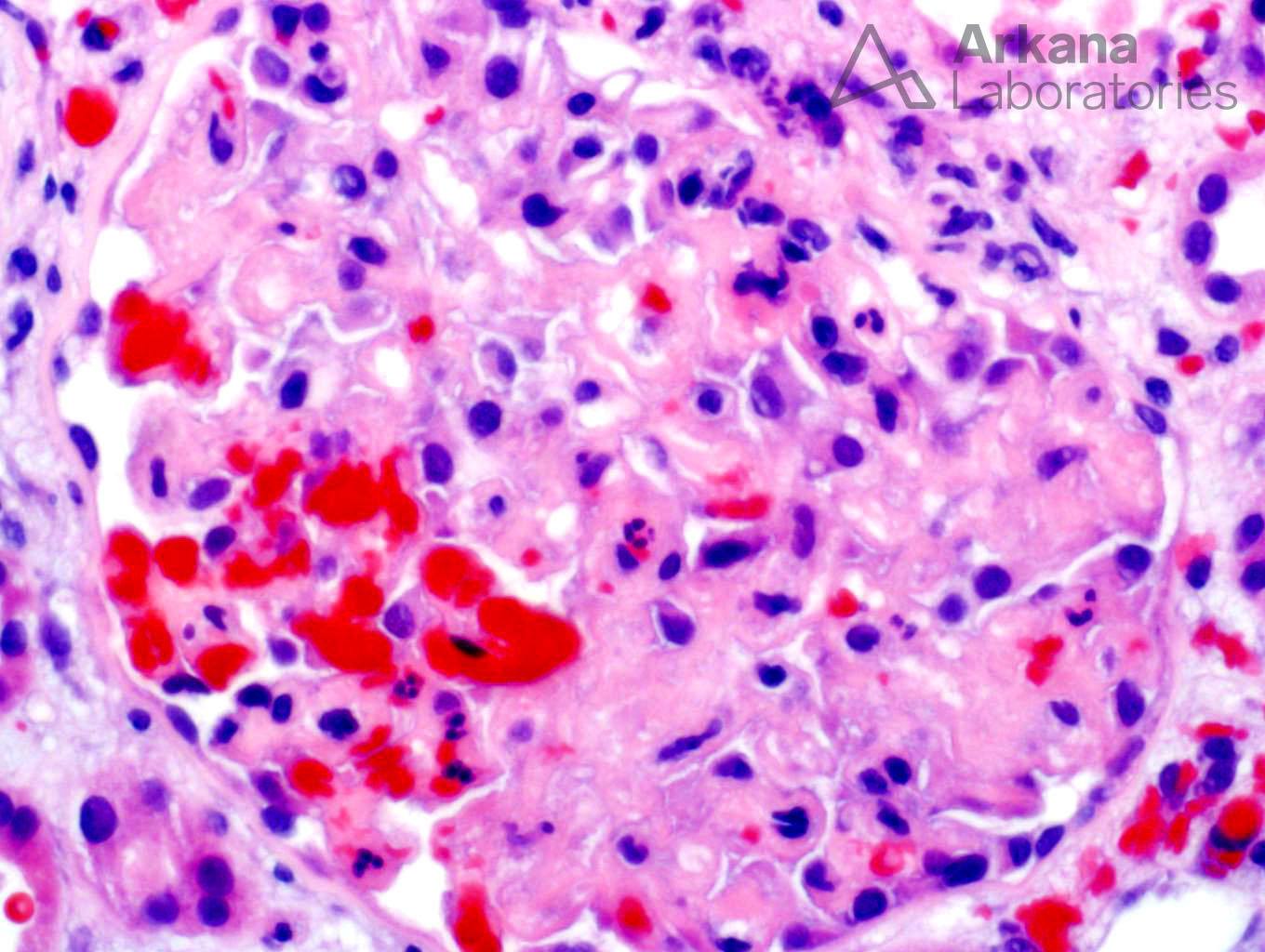
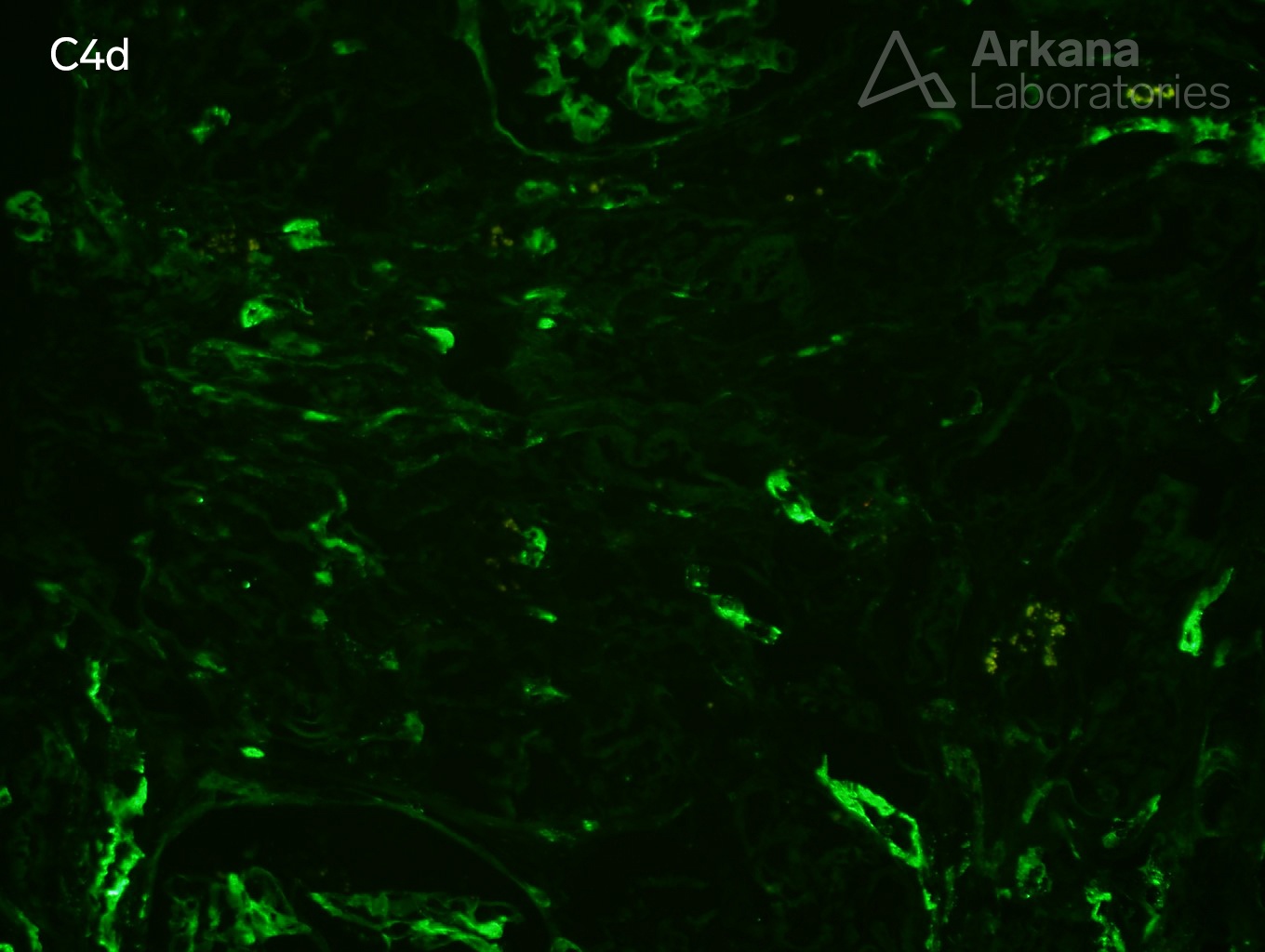
The biopsy shows a constellation of findings. This includes acute tubular injury, glomerulitis, acute thrombotic microangiopathy, positive C4d staining in peritubular capillaries, and endothelialitis. All of these histological findings have been reported in an acute antibody-mediated rejection which is the best answer. It is true that the acute tubular injury is probably the cause of the patient’s delay in graft function, but it is likely secondary to the antibody-mediated rejection and the presence of glomerulitis and a positive C4d makes acute antibody-mediated rejection a better selection. Whenever you see acute thrombotic microangiopathy, thrombotic thrombocytopenic purpura is in the differential. However, in the transplant setting, one of the most common causes of thrombotic microangiopathy is antibody-mediated rejection and the other findings in this biopsy points toward this diagnosis. Vasculitis is the destruction of the vascular wall with fibrinoid necrosis and acute inflammation (neutrophils) which is not present here. However, the biopsy shows lymphocytes undermining the endothelial cell layer within arteries which can be seen in either antibody-mediated or cellular-mediated rejection.
Quick note: This post is to be used for informational purposes only and does not constitute medical or health advice. Each person should consult their own doctor with respect to matters referenced. Arkana Laboratories assumes no liability for actions taken in reliance upon the information contained herein.