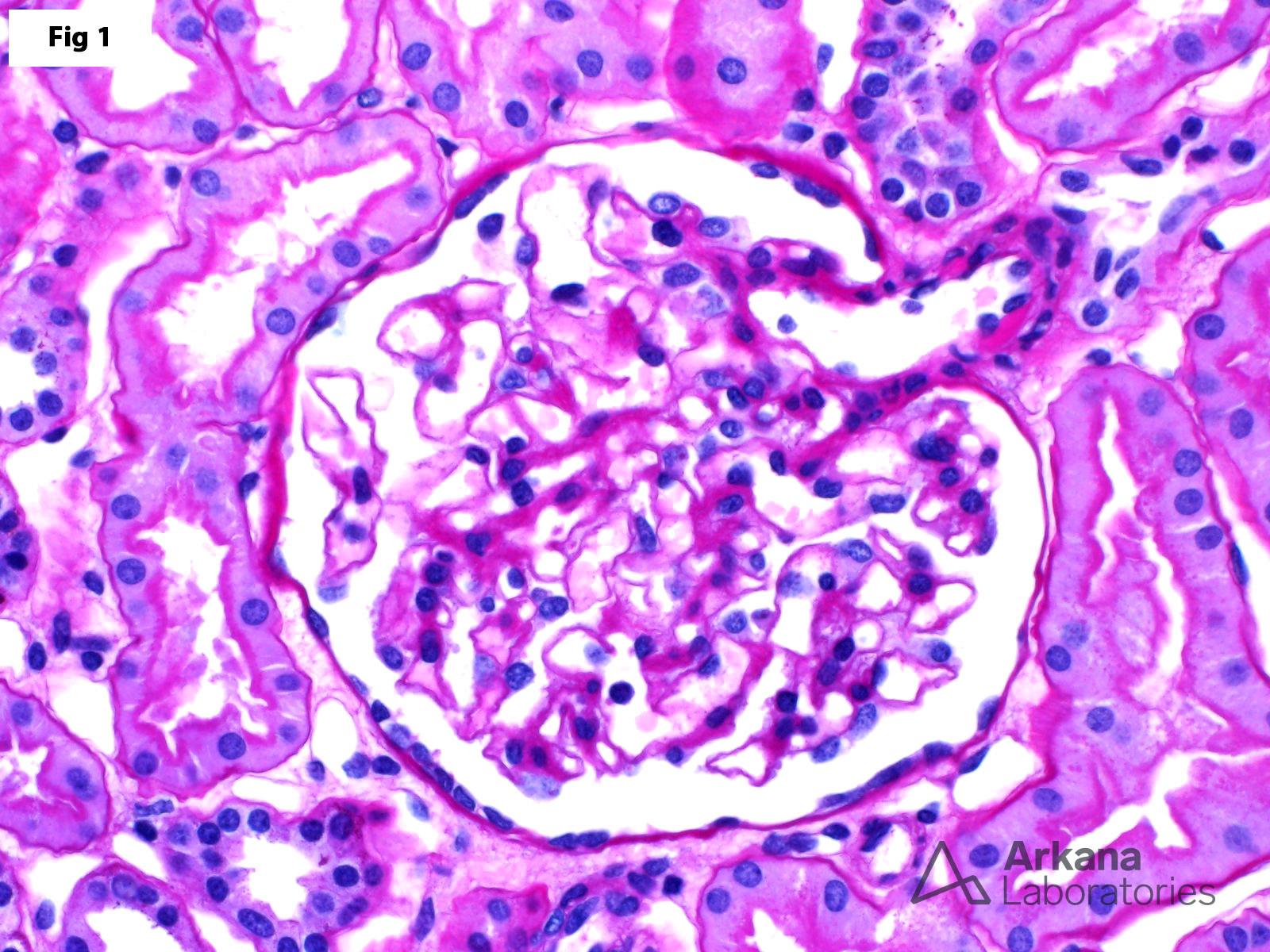
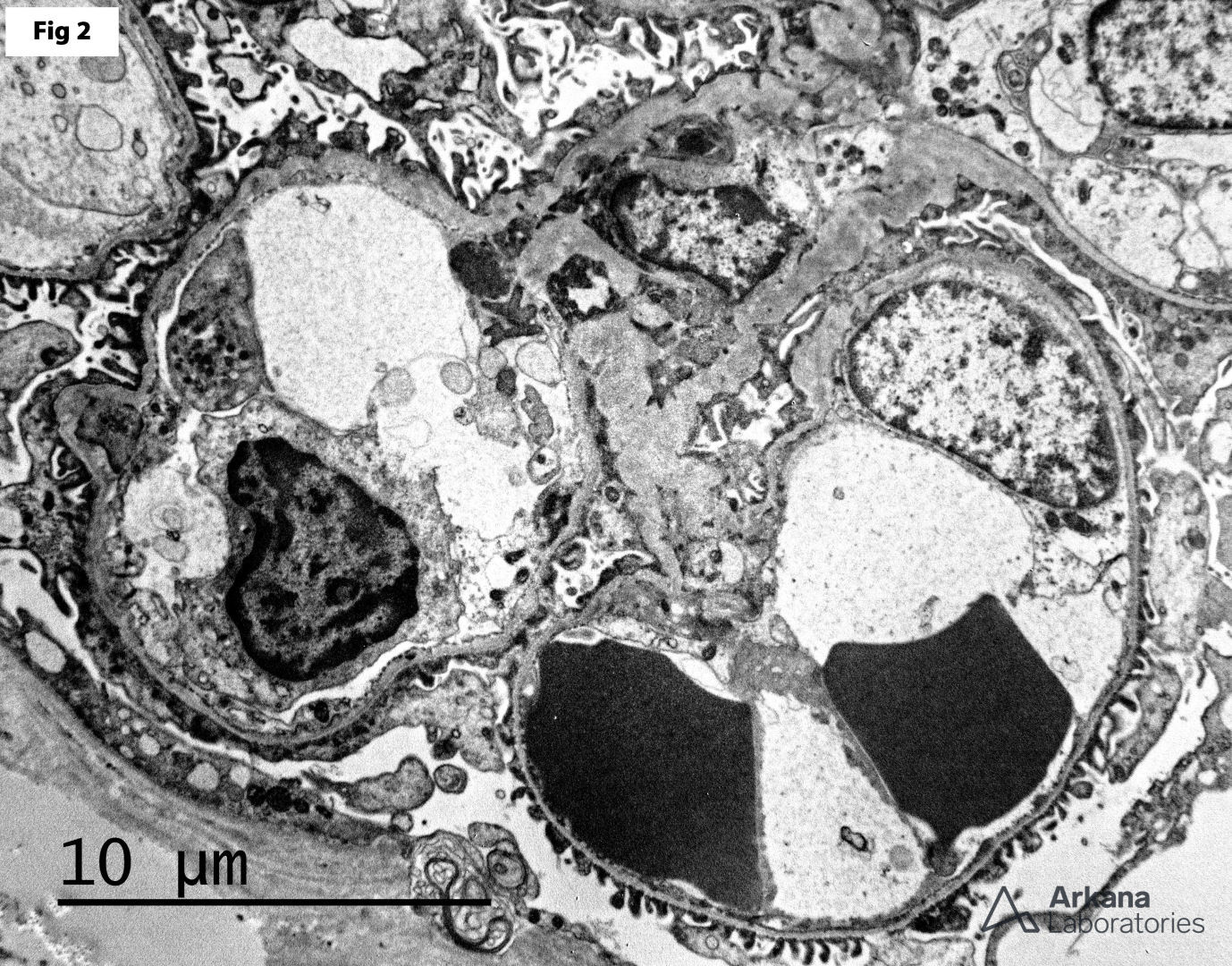
This 41-year-old female presents with microscopy hematuria and subnephrotic proteinuria. The clinical workup is negative for urinary tract infection, nephrolithiasis or other lower urinary tract diseases. A renal biopsy shows essentially unremarkable glomeruli by light microscopy (Fig 1), with scattered red blood cells within the tubular lumens and marked, uniform thinning of the glomerular basement membranes by electron microscopy (Fig 2). These findings are consistent with thin basement membrane disease (TBMD). TBMD affects approximately 1 to 5% of the general population. Mutations in the COL4A3 and COL4A4 genes are identified in up to 40% of affected patients. Furthermore, TBMD may be the initial presentation of X-linked Alport syndrome or may be seen in heterozygous carriers of the disease. Most patients present with microscopic or macroscopic hematuria; however, a small subset of these patients may also show subnephrotic proteinuria. Nephrotic range proteinuria, renal failure or hypertension are not usually seen in these patients and should raise suspicion for autosomal recessive Alport syndrome. There is no specific therapy for this condition, and the prognosis is usually excellent.
Quick note: This post is to be used for informational purposes only and does not constitute medical or health advice. Each person should consult their own doctor with respect to matters referenced. Arkana Laboratories assumes no liability for actions taken in reliance upon the information contained herein.