This renal biopsy shown here is from a 25-year-old male who presented with acute kidney injury in the setting of hypertensive emergency (260/140). He has no significant past medical history. Serum creatinine is 3.1 and proteinuria is 3.2 g. Hemoglobin is low but platelet count is normal.
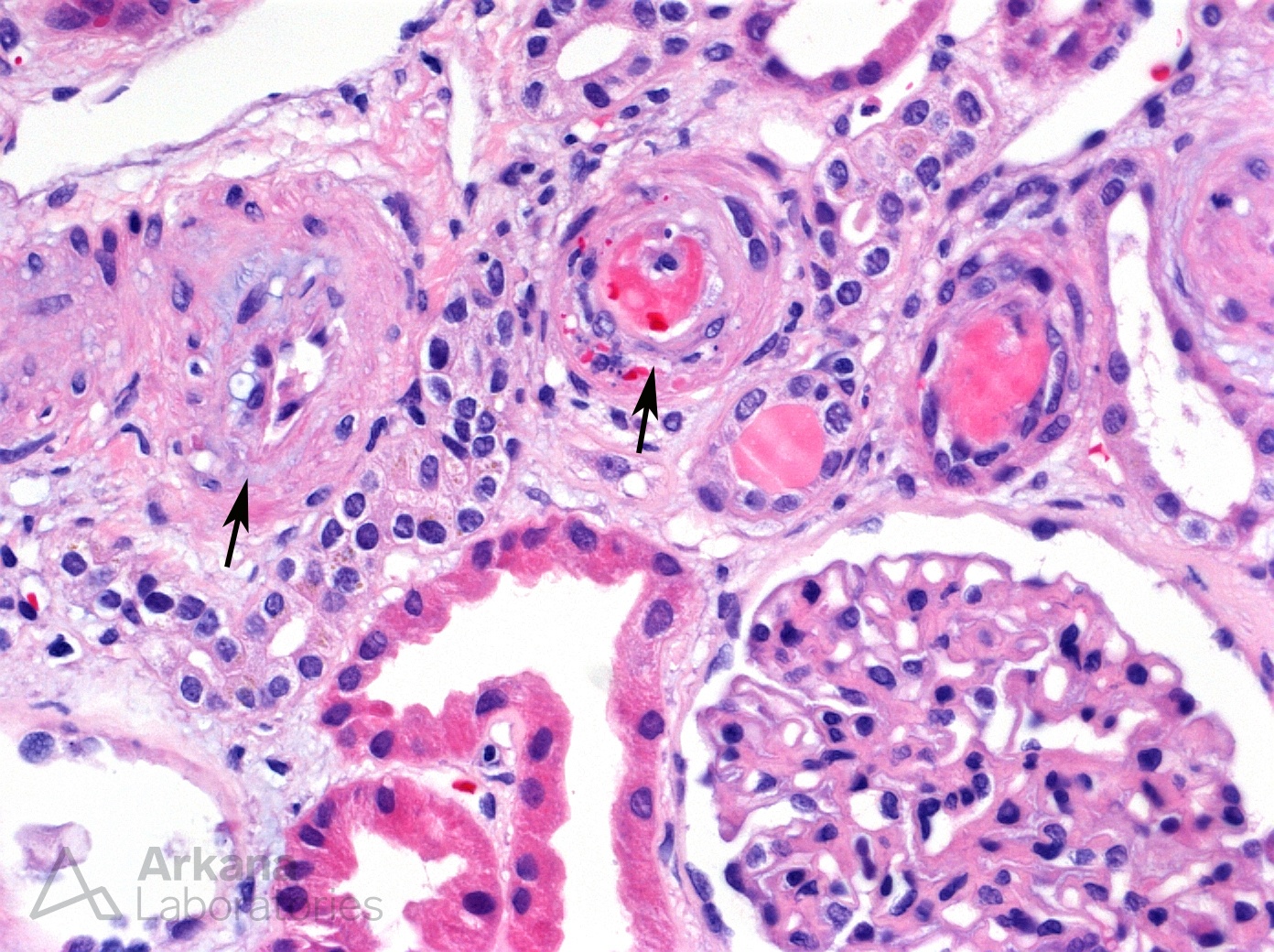
This photomicrograph is representative of the changes in the biopsy including vascular microangiopathic changes (arrows) such as intimal edema with associated fibrin thrombi and schistocytes. Glomeruli were ischemic in appearance but did not show involvement by fibrin thrombi.
The findings are consistent with those classically described secondary to accelerated/malignant hypertension. However, given the morphologic overlap, the differential diagnosis would also include other etiologies of TMA such as autoimmune disease (such as scleroderma renal crisis, antiphospholipid antibody syndrome), drug abuse (specifically, IV Opana and cocaine), disorders of complement regulation (atypical HUS), infection (particularly those due to E. coli and S. pneumonia), ADAMTS13 abnormalities, and malignancy.
A recent case series (see reference below), however, has raised awareness that a number of these patients with malignant hypertension-associated TMA may actually represent atypical hemolytic uremic syndrome. However, the renal biopsy from the patients in this series showed more active glomerular disease including glomerular fibrin thrombi.
Reference: Timmermans SA, Abdul-Hamid MA, Vanderlocht J, et al. Patients with hypertension-associated thrombotic microangiopathy may present with complement abnormalities. 2017 Jun;91(6):1420-1425.
Quick note: This post is to be used for informational purposes only and does not constitute medical or health advice. Each person should consult their own doctor with respect to matters referenced. Arkana Laboratories assumes no liability for actions taken in reliance upon the information contained herein.


