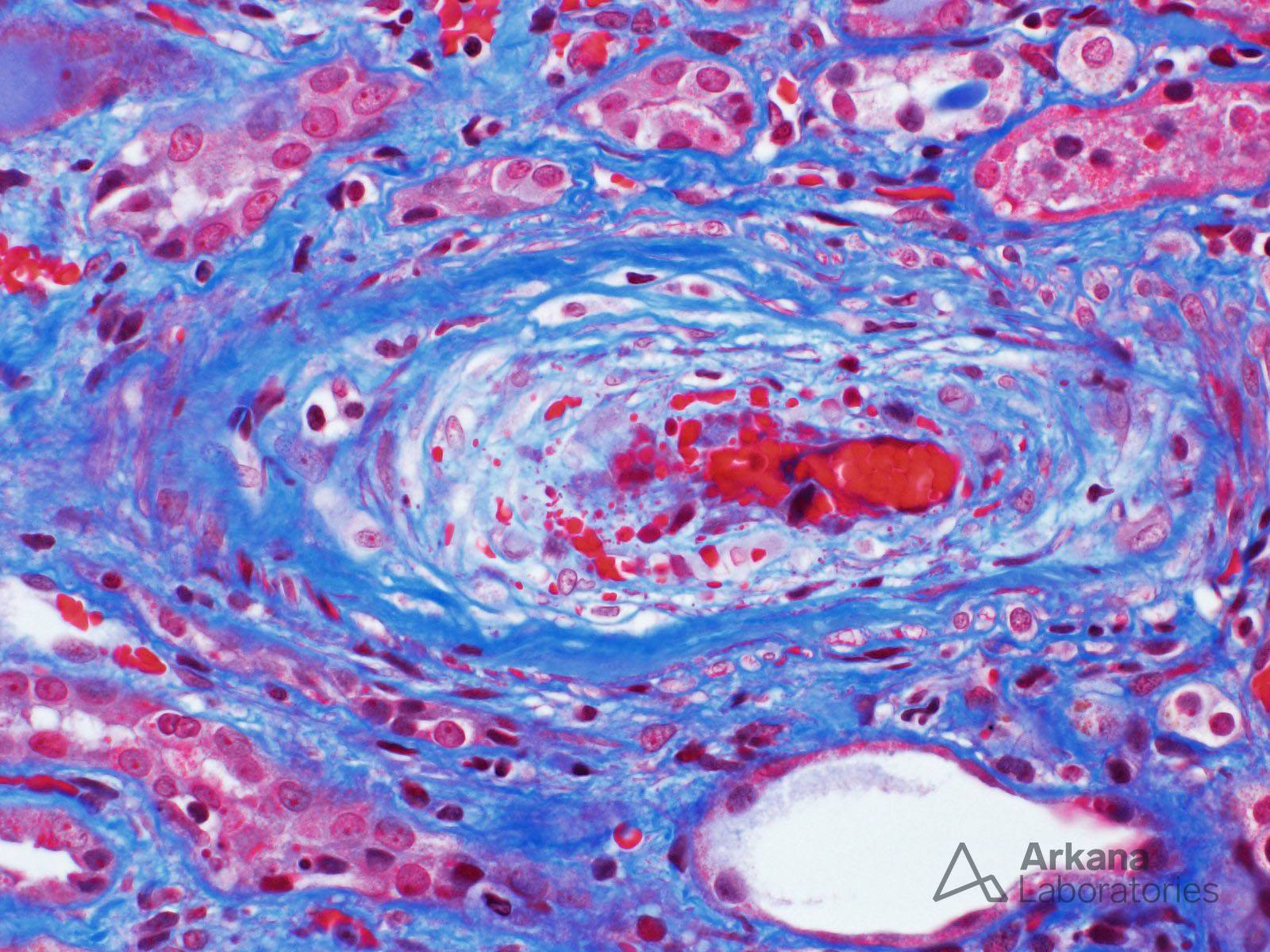
The image (trichrome stain) shows the characteristic arteriolar lesion of acute thrombotic microangiopathy. Note the prominent mucoid intimal edema and extensive red blood cell fragmentation. The differential diagnosis based on this morphologic lesion is broad, and it includes infection, accelerated hypertension, antiphospholipid antibody syndrome, and malignancy, among others. The kidney biopsy was from a 75-year-old Caucasian woman seen in consultation for acute renal failure and hypertension which developed one week after the onset of severe diarrhea. Laboratory tests showed microangiopathic hemolytic anemia, and stool cultures were positive for Shiga toxin-producing E. coli. Hepatitis, ANA, anti-glomerular basement membrane, and ANCA tests were negative, and her C3 and C4 levels were normal. The patient was treated for infection-associated hemolytic uremic syndrome (HUS).
See the article by Ferraris et al. if you’re interested in learning about the activation state of the classical/lectin and alternative pathways of complement during the acute phase of endemic HUS.
Ferraris JR, Ferraris V, Acquier AB, Sorroche PB, Saez MS, Ginaca A, Mendez CF. Activation of the alternative pathway of complement during the acute phase of typical haemolytic uraemic syndrome. Clin Exp Immunol. 2015 Jul;181(1):118-25. https://www.ncbi.nlm.nih.gov/pubmed/25677399
Quick note: This post is to be used for informational purposes only and does not constitute medical or health advice. Each person should consult their own doctor with respect to matters referenced. Arkana Laboratories assumes no liability for actions taken in reliance upon the information contained herein.